Delirium in Addiction Treatment: What Families Should Watch For
Delirium during addiction treatment can be life-threatening. Learn the warning signs, risk factors, and when to seek immediate medical help for your loved one.
Delirium during addiction treatment can be life-threatening. Learn the warning signs, risk factors, and when to seek immediate medical help for your loved one.
Learn how histrionic personality disorder intersects with addiction. Silicon Valley Recovery offers specialized dual diagnosis treatment and family support.
Nocturnal enuresis in adults often signals underlying health conditions. Learn the causes, when to seek help, and treatment options at Silicon Valley Recovery.
Acute stress disorder requires immediate care. Learn symptoms, causes, and evidence-based treatment options at Silicon Valley Recovery. Get help today.
Specialized avoidant personality disorder treatment addressing co-occurring addiction. Compassionate care helps you build confidence and lasting recovery.
Caffeine induced anxiety disorder can undermine recovery efforts. Learn how your daily coffee intake may be triggering anxiety and sabotaging treatment success.
Obsessive–compulsive personality disorder affects high achievers through perfectionism and rigidity. Discover evidence-based treatment at Silicon Valley Recovery
Dependent personality disorder and addiction require integrated treatment. Discover why treating both conditions simultaneously leads to lasting recovery.
Learn how drugs and alcohol cause amnesia and memory loss. Discover evidence-based treatment options and cognitive recovery strategies at Silicon Valley Recovery today.
“Drunk eyes” is a term used to describe the observable eye and facial changes that follow alcohol consumption. While drinking, many people notice signs like bloodshot eyes, unfocused staring, slow blinking, and abnormal eye movement. These changes are not random.
They happen because alcohol influences your brain, the muscles of the eye, and the processing systems of vision. Recognizing these changes can help you spot common intoxication signs in yourself or others, especially in social and safety-related situations.
Drunk eyes result from alcohol’s direct interference with brain function and eye movement. Alcohol affects muscle coordination, attention, and movement control. This makes the eyes appear glassy, sluggish, or unnaturally wide. These disruptions are usually accompanied by vision impairment, slow reaction, and loss of concentration.
Alcohol makes blood flow increase in the face and the eyes. This leads to facial puffiness and red eyes. The tear film also becomes unstable, which can cause dryness and a burning sensation. These visible signs are classic indicators of intoxication, caused by the underlying physical changes alcohol triggers.
Your eye muscles must work together to keep images clear and aligned. Alcohol weakens this teamwork. When muscle timing becomes uneven, people experience double vision, drifting gaze, and difficulty tracking objects. This loss of control also connects with impaired coordination during walking and hand movement.
One of the earliest drunkenness indicators is visible bloodshot eyes.
Alcohol causes tiny blood vessels to expand around the eyes. This creates redness and a tired appearance. It also reduces the supply of oxygen to small tissues, making the eyes seem irritated.
The effects of alcohol on the circulation and nervous system activity to cause redness in the face and eyes are well explained through reliable medical advice offered by the National Institute on Alcohol Abuse and Alcoholism.
Dilated pupils can appear during drinking because alcohol interferes with the brain’s control of light response. Usually, pupils become small in bright light. This reflex is less accurate during intoxication.
Dilated pupils alone don’t confirm intoxication. They usually appear alongside other signs, such as slowed reactions, unsteady balance, and slurred speech. According to the National Eye Institute, alcohol disrupts the nerve signals that control pupil size and visual clarity.

Alcohol gradually disrupts visual clarity, focus, depth perception, and everyday visual performance.
Alcohol reduces the brain’s ability to combine light signals into clear images. This leads to blurred edges, delayed recognition, and poor depth judgment. These changes explain why driving, reading signs, and recognizing faces become more difficult while intoxicated.
Eye tracking and body balance rely on the same brain systems. Vision impairment and unsteady movement go hand in hand when these shared brain systems are compromised. This relationship is supported by research from the Centers for Disease Control and Prevention.
These indicators can help people recognize dangerous alcohol consumption early, particularly in social settings, behind the wheel, and in the workplace.
Alcohol affects both the body and behavior during progressive intoxication and daily functioning.
Eye changes rarely appear alone. Alcohol also interferes with speech, balance, memory, and judgment. Visual disruption is usually followed by poor attention, slow decision-making, and emotional changes. When people ignore these early warnings, the risk of injuries and unsafe choices increases significantly.
| Area affected | Common changes during drinking |
| Brain | Slower thinking and delayed responses |
| Balance | Increased falls and poor posture |
| Speech | Slurring and reduced clarity |
| Memory | Short-term recall problems |
| Behavior | Risk-taking and emotional swings |
In case alcohol consumption is becoming a problem for your health, social life, or general stability, professional help can make all the difference. Silicon Valley Recovery is a non-judgmental and confidential treatment center for those with drinking problems. Our clinical team helps individuals identify their triggers, build healthier coping strategies, and regain control over their recovery.
Whether you’re concerned about recurring binge drinking, chronic dependence, or early warning signs like vision changes and loss of control, reaching out for help can prevent long-term damage.
To learn more about the different treatment approaches, to schedule a personal consultation, and to start a healthier, safer future today, reach out to our recovery experts who genuinely care about your well-being.

Yes, redness may not be a requirement of dilated pupils. Other intoxication signs will normally indicate alcohol involvement. Pupil changes can occur due to nervous system effects even without visible redness.
Most eye changes fade within several hours. Heavy drinking may cause effects that last longer. Recovery time also depends on how quickly the body metabolizes alcohol.
Medical eye conditions tend to be chronic and persistent. Drunk eyes resolve with sobriety, while medical conditions do not. If symptoms continue after alcohol has worn off, a medical evaluation may be necessary.
Yes, alcohol weakens contrast and distance judgment. This increases accident risk at night. It also slows visual processing speed, making reactions to movement less accurate.
The extent to which drunkenness indicators are noticeable depends on body size, tolerance, hydration, and fatigue. Genetics and individual sensitivity to alcohol also influence how visible these signs become.
When you are not considered to be an addict, it is uncomfortable to stop taking a drug that influences your nervous system. Hydroxyzine withdrawal causes symptoms in many individuals who suddenly quit or reduce the dose too rapidly. The symptoms may be mild, like slight discomfort, or severe emotional distress.
Quite often, knowing what will happen reduces fear and helps avoid unwarranted panic. This article explains why withdrawal occurs, the duration of withdrawal, and how the withdrawal may be safely managed without harming the body as you wean off hydroxyzine.
Hydroxyzine works by calming histamine activity and lowering the arousal of the nervous system. The brain gets accustomed to that constant relaxing effect.
Once the medication is stopped, the body will have to learn again how to control stress, sleep, and alertness independently. It is this adaptation stage that most individuals identify as the withdrawal.
The nervous system may also respond intensely to abrupt changes, although hydroxyzine is not a controlled substance. A study published by MedlinePlus offers an explanation of the antihistamine effects on brain chemistry, particularly during habitual use.
Hydroxyzine withdrawal is often mistaken for a discontinuation syndrome. Withdrawal typically involves physical and emotional symptoms that occur during the body’s adaptation.
Discontinuation syndrome is a short-term reaction brought about by an imbalance of chemicals and not addiction. Both experiences are uncomfortable, yet neither of them necessarily points to substance misuse or long-term damage.
Your body prefers stability. Stress signals are reduced when hydroxyzine is taken on a regular basis. After it is removed, the nervous system temporarily overcorrects. This response causes anxiety, sleep disturbances, and mood swings. This reaction relates to short-term medication dependency rather than addiction.
| Phase | Time Frame | Typical Experience |
| Initial response | 6–24 hours | Mild restlessness, headache, and early withdrawal symptoms. |
| Adjustment period | 1–3 days | Sleep disruption, irritability, nausea. |
| Peak phase | 3–7 days | Strong anxiety rebound, fatigue, shakiness. |
| Stabilization | 1–2 weeks | Symptoms gradually lessen. |
| Recovery window | 2–4 weeks | Emotional and physical balance returns. |
The Mayo Clinic and the National Institute of Mental Health also offer educational information on how to schedule medications.
The initial stage is usually uncomfortable, not critical. Individuals become aware of their heartbeat, feel tense, and sleep lightly. These symptoms tend to be signs of nervous system adaptation rather than failure.

The third through seventh days are usually the toughest. The anxiety can skyrocket and become even more severe than it was prior to therapy. This stage is often confused with benzodiazepine withdrawal, although hydroxyzine does not act in the same way.
These withdrawal symptoms normally subside as the nervous system normalizes.
One of the most unpleasant aftereffects of hydroxyzine withdrawal is anxiety rebound. It is an anxiety symptom that becomes more severe after discontinuation. This is not to say that the anxiety disorder has gotten worse. It represents acute excessive stimulation of stress pathways.
The National Institute of Mental Health provides educational mental health resources that describe how rebound anxiety is differentiated from chronic anxiety conditions.
Rebound anxiety is abrupt and more physical. Individuals experience chest tightness, internal shaking, and restlessness with no apparent triggers. Ordinary anxiety is progressive and is related to thoughts or circumstances.
Simple measures help regulate the nervous system at this stage. Light physical exercise, regular sleep schedules, hydration, and breathing exercises mitigate the severity of the symptoms. During this adjustment, short-term counseling can help stabilize emotions.
The easiest method to avoid discontinuation syndrome is a gradual decrease. Slow hydroxyzine tapering enables the brain to adapt gradually as opposed to responding suddenly. No one-size-fits-all approach exists in terms of tapering, although the majority of plans are to decrease the dose day by day or week by week.
A medical practitioner takes into consideration dosages, period of use, and general health when designing a tapering schedule. Therapeutic changes are also not made according to fixed schedules. This will help to alleviate anxiety and help increase comfort during the process of weaning off hydroxyzine.
Medication dependence is not necessarily associated with cravings and misuse. With hydroxyzine, it is merely that the nervous system has become accustomed to chemical aid. Hydroxyzine withdrawal restores the brain’s balance of stress hormones and sleep regulation. This is the reason why fatigue and anxiety go hand in hand.
Knowledge of this physical process avoids unnecessary fear and helps patients remain adherent to tapering.
Silicon Valley Recovery offers well-organized, compassionate service to patients with hydroxyzine withdrawal or continuing withdrawal symptoms and severe rebound of anxiety. Our healthcare unit provides individual assessment, prescriptions, and emotional help during recovery.
In collaboration with prescribing providers, we develop a safe plan for hydroxyzine tapering and administer injections and consider the issue of medication dependence. Whether it is unpleasant or overwhelming, professional advice will help ease the recovery process and make it less stressful.
In case you or your loved one requires assistance in weaning off hydroxyzine, talk to a professionally trained specialist and start a safer journey.

Most hydroxyzine withdrawal symptoms improve within one to two weeks. However, mild effects may last longer. Gradual improvement is common as the body readjusts to functioning without the medication.
Yes, functional medication dependence can develop. Even when taken as prescribed. This is more likely with long-term use or frequent reliance on the medication for anxiety relief.
A slow, supervised tapering schedule guided by a healthcare provider is safest. The taper duration may vary depending on dose, duration of use, and individual response.
Anxiety rebound often resolves naturally. But short-term support may help. Behavioral coping strategies and reassurance can reduce discomfort during the adjustment period.
Benzodiazepine withdrawal is usually more severe and longer-lasting than hydroxyzine discontinuation syndrome. It may involve significant neurological and physical symptoms requiring medical supervision.
Millions of individuals across the world experience chronic and acute pain, which in most cases disrupts mobility, sleep, mood, and quality of life. Tramadol and oxycodone are among the most prescribed prescription painkillers, which, in most cases, are compared based on their capability to provide effective pain relief without jeopardizing their safety and health benefits when used on a long-term basis.
Knowledge of the differences between tramadol and oxycodone assists patients and caregivers in making sound choices about treatment, safety, and recovery. This is an elaborate comparison of opioids, which covers the mechanisms of action of these drugs, their effectiveness as drugs, side effects, addiction potential, appropriate dosage, and withdrawal symptoms.
The application of opioid therapy in patients with moderate to severe pain is based on modern medicine, which is closely monitored. Both tramadol and oxycodone are considered to be in the same opioid category, though they vary considerably in strength, pharmacology, and clinical application. Although both offer significant pain relief, their safety profiles and long-term consequences differ.
To obtain general medical information about opioid safety, see reliable sources of information about the topic in the US Centers for Disease Control and Prevention (CDC) opioids and the overview of pain management provided by the World Health Organization.
The action of tramadol is dual. weak stimulatory activity at the opioid receptors and increases the levels of serotonin and norepinephrine in the brain, which improves pain signal modulation. This effect is combined and leads to moderate pain relief, which is why tramadol is frequently regarded as weaker in the opioid comparison.
Oxycodone, in turn, acts directly on the opioid receptors, which have a higher binding affinity. This has a strong analgesic effect, which can be used in the treatment of serious injuries, post-surgery, and in chronic pain cases. This higher potency, however, increases the risks of side effects, tolerance, and risk of addiction unless closely monitored.

Doctors consider a number of things before administering either drug, such as the severity of pain, patient history, age, and risk of misuse. Tramadol is usually used when moderate chronic pain is involved, and the medical professionals desire to reduce respiratory depression or excessive sedation.
Oxycodone is normally used in cases when a patient has serious pain and other drugs are not effective. Tramadol can be administered to patients with a history of substance use because it has a relatively low abuse potential; however, care should be taken in any prescription painkiller regimen.
| Factor | Tramadol | Oxycodone |
| Strength | Moderate analgesic effect | Strong analgesic potency |
| Best for | Moderate chronic pain | Severe acute or chronic pain |
| Onset | Gradual | Faster |
| Duration | Moderate | Longer, depending on formulation |
| Overall drug efficacy | Effective but milder | Highly effective for intense pain |
Both drugs offer significant pain relief, but effectiveness depends on the level of pain, tolerance, and long-term treatment purposes.
The pharmacology of tramadol is unique and enables the drug to act on opioid receptors and neurotransmitter pathways. This decreases the intensity of pain as well as enhances the emotional response to pain, which is useful in chronic pain syndromes like neuropathic pain or fibromyalgia.
Tramadol is less likely to cause serious side effects and reduces respiratory depression, but such effects are possible because its opioid effect is less potent.
Oxycodone produces powerful and stable analgesic effects, which are very effective in major surgeries, injuries, and pain associated with cancer. The greater affinity of its receptor enhances tolerance and dependency. With time, a patient might need to change the dosage, and hence the need to monitor their health when taking the strong prescription painkillers in chronic care is essential.
The two drugs have undesirable effects. Patients are advised to take note of physical and mental changes during therapy, particularly during dose changes or during prolonged therapy.
Although tramadol has less potent side effects, the stronger opioid effect of oxycodone can lead to greater sedative effects and a higher rate of respiratory depression, especially in older patients or those with respiratory illnesses. Observation helps ensure safer analgesia, and complications are avoided.
The possibility of dependency is one of the most critical issues of the tramadol vs. oxycodone debate. Opioids modify the brain reward systems and may lead to tolerance, physical dependency, and compulsive use. The National Institute on Drug Abuse is a good source of education on opioid dependency.

It is generally considered that tramadol has less potential for abuse due to its less strong opioid receptor activity. However, long-term use may be associated with physical and mental dependence. High doses of misuse may augment the risk of seizures and serotonin imbalance. Hence, it is important to take tramadol on time as prescribed, even in this opioid comparison.
Physical dependence happens when the body becomes used to a drug, and the withdrawal symptoms in case of a sudden withdrawal are experienced. Psychological addiction entails yearning, use that is compulsive, and uncontrolled.
Both conditions can be created by either medication, with oxycodone having more euphoric effects that tend to raise addiction risk. Long-term harm from prescription painkillers can be minimized by safe prescribing, dose monitoring, and gradual tapering.
The dosage, timing, and medical support are crucial factors for safe opioid use. Doctors change dosages according to the intensity of pain, the response of the body, and the duration of the treatment.
| Medication | Typical Starting Dose | Maximum Daily Dose | Notes |
| Tramadol | 25–50 mg every 4–6 hours | 400 mg | Gradual titration recommended |
| Oxycodone | 5–10 mg every 4–6 hours | Varies by formulation | Requires strict supervision |
The right dosage would reduce the side effects, avoid overdosing, and aid in safer long-term pain management.
The initial doses of Tramadol therapy are usually low so as to check tolerance. The doctors slow down the dosage until sufficient effects of the drug are felt, and vice versa. Long-acting preparations can be administered for chronic pain to stabilize the levels of pain relief and decrease breakthrough pain. Patients are not supposed to adjust their dosage themselves, as it leads to the risk of health conditions as well as addiction.
Abrupt cessation of opioid treatment may cause unpleasant and even excruciating withdrawal effects. These can be restlessness, sweating, nausea, anxiety, insomnia, muscle aches, and irritability. Appropriate tapering helps to alleviate distress and to enhance the results of the treatment.
Reduction in doses is gradual, which enables the nervous system to adapt gradually. Mild withdrawal symptoms of anxiety and restlessness could be managed through hydration, sleep regulation, and supportive medications. Because tramadol can impact serotonin levels, tapering helps prevent mood swings and neurological pain.
Withdrawal symptoms of oxycodone may be more severe because it is a stronger opioid. Doses are usually decreased during weeks or months, depending on the duration of treatment by medical professionals.
Comfort and reduction in relapse rates in opioid discontinuation are enhanced by supportive care, counseling, and symptom-relief medications. When making any opioid comparison, special caution should be exercised in tapering when it involves long-term treatment.
Once the opioid dependence evolves, the help of a professional will help to regain physical and emotional stability. Silicon Valley Recovery is a highly personalized center that treats patients with opioid misuse and dependency on chronic pain medication, as well as provides comprehensive withdrawal management. The evidence-based programs they have are on safe detoxification, psychological support, relapse prevention, and long-term healing.
Patients are thoroughly provided with care that covers physical dependence and underlying emotional difficulties that tend to follow chronic pain and opioid dependence. Under caring clinical guidance, the patient will be able to move out of bad patterns of medications safely and be able to take control of their health and well-being.
Whether you are in pain and cannot control your opioid addiction, abusing drugs, or undergoing challenging withdrawal symptoms, you can seek professional assistance. Get personal and confidential treatment at Silicon Valley Recovery.
There should not be a combination of these medicines unless it is strictly under the advice of the doctor. Taking more than one prescription analgesic painkiller enhances sedation, respiratory depression, and general addiction. Physicians usually consider safer options and then combine opioids.
Oxycodone normally lasts longer in the body, particularly in its extended-release form, whereas tramadol is metabolized faster. Detection time, however, varies depending on metabolism, dosage, and length of use.
Tramadol has less severe withdrawal effects than oxycodone because of its weaker opioid receptor strength in most cases of opioid comparison. Nevertheless, they both need to be tapered gradually to be comfortable and safe.
The use of tramadol among the aged is believed to be safer, as it is less likely to induce respiratory depression and sedation. Nonetheless, it still needs close monitoring of dosage to prevent dizziness, falls, and drug interactions.
Tramadol generally carries a lower addiction risk than oxycodone, but neither medication is risk-free. Patients with prior substance use history should receive close medical supervision and consider non-opioid pain management when possible.
Narcan is potentially life-saving in an opioid overdose emergency. This drug has been able to save an immense number of lives by turning the tide of opioid toxicity quickly. Nevertheless, being aware of the length of staying time of Narcan is the key information that all people who have access to this overdose antidote must have.
The effects of Narcan are short-lived, and in most cases, when an overdose is involved, the drug becomes persistent. That gives a dangerous gap in which an individual who seemed to have recovered can fall into further overdose as Narcan subsides. The awareness of the Narcan period and the understanding of why emergency treatment is necessary despite successful reversal may save lives.
Naloxone is an opioid antagonist medication whose brand name is Narcan, and it reverses the effects of opioid overdose very quickly. Although naloxone also blocks opioid receptors, as opposed to opioid receptor activators, it pushes the existing opioid off the receptor, and further binding is prevented.
In case of opioid overdose, the drugs inhibit the respiratory system of the brain, slowing down breathing or halting it completely.
The efficacy of Naloxone relies on its strong affinity to opioid receptors. Naloxone molecules and opioid molecules compete for receptors when administered. Since naloxone is stronger than most opioids, it competently displaces the opioids at the receptors. The main features of this mechanism are:
The National Institute on Drug Abuse (NIDA) states that naloxone has a long history of use and has been safely and effectively used to reverse opioid overdoses for decades, and is regarded as a critical resource in overcoming the opioid crisis.
The most troubling issue regarding Narcan is the length of action question: Naloxone is generally effective between 30 and 90 minutes, depending on dose used, route of administration, and other individual factors. This Narcan period is usually less than the period of action of the opioids it is supposed to overcome.
Naloxone has a half-life, a period of time it takes to excrete half of the drug, between 30 and 81 minutes. This is a rather short half-life, which is why opioid overdose reversal may end up being worn out even as the opioid remains active in the system. The timing of an overdose is an essential fact that anyone should know when responding to it.
The window for overdose antidote administration is narrow. The causes of brain damage due to oxygen deprivation may start four to six minutes after respiratory arrest. The application of Narcan in the shortest time achieves maximum chances of full recovery without neurological losses.
The variables have a number of factors that determine Narcan time and general efficacy in a particular overdose case. By knowing these factors, it is possible to understand why there are cases of multiple-dose overdose reversals and those that do not need them.
The table provided below shows some important factors that influence the use of Narcan:
| Factor | Impact on Duration | Clinical Significance |
| Type of opioid involved | Longer-acting opioids outlast naloxone | Higher risk of re-sedation with fentanyl, methadone |
| Amount of opioid consumed | Large doses may overwhelm naloxone | Multiple Narcan doses are often needed |
| Route of Narcan administration | IV works fastest; nasal spray is slightly slower | Nasal spray is widely available for lay responders |
| Individual metabolism | Liver function affects naloxone clearance | Some individuals metabolize naloxone faster |
| Body weight and composition | Distribution varies with body mass | Standard doses are effective across most adults |
The commonly used dosage of Narcan to reverse an overdose varies based on the formulation which is used. Various products have varying doses of naloxone, and knowledge of these variations can assist the responder in making informed decisions when responding to an emergency.
The existing dosing regimens of opioid antagonists include the following:
The fact that Narcan may expire before the opioid effect subsides is one of the most serious things about opioid overdose reversal. This may make an individual who seemed to have bounced back fall into overdose, which may occur especially when a person is alone or when those around them feel that the crisis is over.

The acute treatment of opioids does not always involve a single dose of naloxone, especially in cases of severe synthetic opioids such as fentanyl. Indications of the necessity of further doses are:
When Narcan is administered, it is necessary to be continuously monitored. Indications of the possibility of a second dose include:
The administration methods of Narcan are slightly different, yielding varying onset and action durations. The nasal spray preparations so popularly introduced into the market today are almost as rapidly acting as the injection procedures, and are much easier for the untrained layman.
The effects of nasal spray are usually felt between two and five minutes, and at an optimum level of between 20 and 30 minutes of administration. The intramuscular injection takes between three to five minutes to take effect, whereas the intravenous administration takes one to two minutes to act. Irrespective of the method, the time of action is similar and is 30 to 90 minutes.
The Centers for Disease Control and Prevention (CDC) suggests that naloxone should be as accessible as possible in the community where there is an opioid overdose and offers resources on how to access and learn to use the life-saving drug.
An opioid overdose survivorship is a turning point in many cases. It may be an eye opener that makes a person want to seek help, or it may be a red flag that drug use has reached the stage of a life-threatening level.
At Silicon Valley Recovery, we offer full-scale care of opioid use disorders, which involves medically monitored detoxification, medication-assisted treatment, and evidence-based therapy that addresses the root causes of addiction.
In case you or your loved one has overdosed or is having problems with the use of opioids, there is assistance. Contact Silicon Valley Recovery today to find out more.
Surely, the efficacy of naloxone is highly dependent on the opioid. Strong synthetic opioids such as fentanyl may take more than one or several times higher doses before full reversal than heroin or prescribed opioids.
Naloxone has a half-life range of 30 to 81 minutes, and the effects of the drug start wearing out after the first hour. That is why constant observation and the ability to provide more doses are also essential in the post-reversal period.
Several doses may be required since most of the opioids, especially fentanyl and slow-acting preparations, have a longer half-life in the body as compared to naloxone. When the initial dose expires, the remaining opioid is likely to trigger re-sedation and respiratory depression.
The technique influences the time of onset but not the effectiveness and duration. Nasal spray is a little slower acting in comparison with injection and results in an equal reversal after absorption, but it is the method of choice among community responders.
Naloxone can easily be degraded by improper storage, specifically by exposure to extreme temperatures and this weakens its activity. Nevertheless, even possibly degraded naloxone is still to be used during an emergency since a certain level of effectiveness is better than no effect at all, as the individual waits to receive medical attention.
One moment you feel fine. Then the room begins to spin, and your stomach is churning, and you feel a feeling of panic. And that is why you might have greened out, should you have ever experienced this after taking cannabis. This unpleasant and even frightening experience occurs when one overwhelms the body with more THC than it can comfortably process.
One way that you can respond to it is by understanding what greening out feels like and knowing the symptoms so that you will know how to react to it in case it occurs to you or someone you know.
Greening out is a condition that happens when one consumes excess cannabis. The experience is usually of differing intensity and usually incorporates a number of physical and psychological manifestations that appear suddenly and may be overwhelming. To a significant number of individuals, it is the time when an enjoyable elevation turns out to be a very uncomfortable experience.
As soon as you are beyond the level of THC that your body can comfortably process, you have a multi-system response. The physical experience that takes place at the moment is usually:
There are obvious methods through which your body can express that it has reached a point of over-saturation by its tolerance of THC levels. These signals are the protective mechanisms when the nervous system tries to cope with excessive stimulation.
The recognition of the symptoms of greening out before they develop will enable quicker intervention and less distress. The progression normally takes a pattern, although there is a difference between individuals depending on tolerance, mode of consumption, and the level of cannabis taken.

Early signs of greening out can be used to take measures that can reduce the process. Early warning signs include:
The National Institute on Drug Abuse (NIDA) states that cannabis makes several simultaneous impacts on the brain systems, and that is why overconsumption has such a huge array of symptoms in a multiplicity of body systems.
One of the most widespread and confusing features of greening out is cannabis dizziness. The feeling may be mild instability to severe vertigo when it seems that the room is rotating out of control. This is a symptom that, in most cases, causes or increases the severity of other symptoms of greening out, especially nausea and anxiety.
THC acts on the part of the brain that is involved in coordination and balancing, which is the cerebellum. With a sudden rise in the levels of THC, the brain fails to send the usual signals between the cerebellum and other brain parts, which causes the loss of balance, characteristic of the feeling that movement is dangerous or impossible.
The issue of marijuana nausea is one of the most physically unpleasant variables of greening out. The gastrointestinal discomfort may be mild and characterized by a feeling of queasiness or severe and accompanied by vomiting, which makes the individual do nothing but wait until the feeling subsides.
Cannabinoid receptors that react to THC are found in the digestive system. In case of excessive stimulation of these receptors, the regular functioning of the digestive system is disturbed, which causes nausea, stomach cramps, and even vomiting. The factors contributing to it include:
Even though time is the only inevitable solution to nausea through green out, there are some measures to assist in the treatment. Seeking a cool and quiet spot to lie back, breathing slowly and deeply, keeping fluids coming with small amounts of water, and concentrating on a point of focus can all help a bit as THC levels just drop.
The correlation between the response to anxiety and the physical symptoms during greening out is explained in the following table:
| Physical Symptom | Anxiety Response |
| Rapid heartbeat | Fear of a heart attack or cardiac event |
| Difficulty breathing | Panic about suffocation or inability to breathe |
| Dizziness and disorientation | Fear of fainting or losing consciousness |
| Nausea and stomach distress | Worry about vomiting in public or losing control |
| Tingling or numbness | Concern about stroke or neurological damage |
The greening out sensation of spinning can be a very uncomfortable phenomenon. Such vertigo prevents any attempts to define yourself in space and frequently provokes or aggravates nausea. It has been described by many as how they feel they are on a carnival ride that they can never get off.

THC also acts on the inner ear parts of the vestibular system that generate balance and spatial orientation. When THC levels become overwhelming, the delicate systems will get contradictory or overloading signals, and this will give the typical spinning effect.
The issue of cannabis overwhelm is not confined to personal effects but rather to the entire world, where everything is too much. The lights are too bright, the sounds too loud, and the senses too strong. This overloading of the senses is the reaction of the nervous system to the amount of THC that it is unable to properly deal with.
THC overloading in the nervous system leads to hyperactivation of the nervous system instead of the normal filtering of sensory input. This results in the usual cannabis overload when normal stimuli become unbearable. Symptoms that indicate that the nervous system has overworked include:
A study conducted by the Centers for Disease Control and Prevention (CDC) indicated that the effects of cannabis differ in various factors depending on the tolerance, potency, and individual physiology, which is why some individuals have serious reactions to cannabis, whereas others do not.
Although one greening out episode does not mean that a person has a problem with substance use, recurring episodes or the use of cannabis in spite of adverse effects are possible indications that he/she would need the help of a professional.
At Silicon Valley Recovery, we know that the use of cannabis is not a binary, and not all problematic users require such vigorous care. We provide evaluations, education, and care, which can be outpatient counseling, as well as extensive treatment services based on the needs and situation of the individual.
Contact Silicon Valley Recovery today for a confidential consultation.
The majority of episodes of greening out are between 30 minutes and several hours, and the worst symptoms usually fade away within the first hour or two. The time varies according to the dosage intake, the route of drug usage, and personal metabolism.
Greening out does not permanently affect the nervous system or inner ear, but the process can be very terrifying during the process. The symptoms disappear entirely as soon as the level of THC is restored to normal.
When you shut your eyes, you remove the visual points of reference with which your brain compensates the signals in the vestibular system that are no longer present. The conflicting balance indications are even more vivid without visual anchoring, making the feeling of spinning even stronger.
Symptoms may be managed by finding a comfortable and quiet place, lying down, staying hydrated, and slow, deep breathing as the THC levels return to normal. It may help to remind oneself that it is just a temporary experience, and there is nothing to be scared of.
Although less tolerant, occasional users are more prone to greening out, regular users are also prone to greening out when taking higher potency products or more than they normally do. Tolerance offers some form of protection but does not rule the possibility out completely.
When people search for “toradol vs tramadol,” they usually want a simple answer. Which one works better, and which one is safer? The truth is that both medicines are used for pain, but they work in very different ways.
This pain relief comparison is important, especially if you are dealing with short-term injuries, surgery, or long-lasting pain. Understanding the difference between opioid and non-opioid treatment can help you make better choices with your doctor’s guidance and avoid unnecessary risks.
Toradol is usually discussed in addition to tramadol, as they belong to two different categories of drugs. Toradol qualifies as an NSAID, and Tramadol is an opioid-based drug. This variation has an impact on the way the body will respond to the drug and the speed with which the drug will relieve the pain, as well as the long-term risk of the drug.
In a clear medical approach to pain medicines, the U.S. National Library of Medicine has defined how the different classes of drugs treat pain and inflammation, and this can guide patients in understanding non-opioid and opioid classes.
NSAIDs block swelling and pain chemicals in the body. The opioids directly affect the spinal cord and brain to change the perception of pain. This simple difference creates the distinction between opioid vs. non-opioid treatment and the rationale behind each drug being appropriate in particular situations.
In emergency care settings, Toradol is very popular. Doctors would resort to it when they require effective pain management without involving opioids. It is usually used as a pain reliever in the short run after injuries, surgery, and inflammation.
Official safety guidelines for ketorolac (Toradol) provided by the U.S. Food and Drug Administration in terms of approved applications and time limits serve as helpful non-commercial information that patients can access.
Toradol alleviates pain by decreasing the cause of inflammation. In case of injuries, swelling, and irritated tissues, NSAIDs go directly to the source rather than simply covering up pain symptoms. This is why Toradol is particularly effective in the short-term treatment of muscle pain and sudden flare-ups.
Toradol is usually recommended for short-term and moderate-to-severe pain related to:
This short list shows where Toradol fits best and why doctors avoid using it for long periods.
Tramadol is an opioid medication that is considered to be less powerful than some conventional opioids. It is at times prescribed when non-opioid medicines do not suffice to provide relief.
This is because Tramadol may be effective; the drug is known to be effective. The drug affects pain signals in the brain, and therefore, pain cannot be the main cause brought about by inflammation. The Centers for Disease Control and Prevention provides general information on opioid prescribing and safety.
Tramadol alters the processing of pain in the nervous system. It is also a factor in some of the effects on mood- and pain-related brain chemicals. That is why, even in situations when the main cause of discomfort is not inflammation, people may feel relief.

A basic side effect comparison list and effectiveness summary of the two medications will be provided below to compare their performance in common conditions.
| Pain Type | Toradol (NSAID) | Tramadol (Opioid) |
| Injury-related pain | Strong and fast relief | Moderate relief |
| Inflammatory pain | Very effective | Limited effect |
| Post-surgical pain | Very common short-term option | Used when NSAIDs are not enough |
| muscle pain treatment | Works well for swelling and strain | Helps when pain is nerve-related |
| Migraine Medication | Used in clinical settings | Less commonly recommended |
| Long-term pain | Not recommended | Sometimes used with caution |
Toradol is better in most cases for the muscles that are strained or sports-injured; thus, it treats inflammation. Tramadol can be used in case of nerve irritation-induced pain or in case of NSAID intolerance.
Physicians begin to use non-opioid drugs. Toradol is mostly applied in the treatment of early post-surgical pain, as it decreases swelling and reduces the use of opioids. Tramadol can be introduced subsequently in case of pain that is uncontrolled.
The risks of both drugs are different. This means that a close side effects comparison must be done before either drug is taken.
Toradol can irritate the stomach, increase bleeding risk, and affect the kidneys. For this reason, it is usually limited to only a few days of use. People with ulcers or kidney disease must be careful.
Tramadol can result in dizziness, nausea, constipation, and drowsiness. More importantly, it has the potential for tolerance, abuse, and addiction. They are more severe when used over a long period of time, and they directly affect the safe chronic pain management planning.
Toradol has also found some applications in emergency and urgent care facilities as a migraine drug, particularly in the case of inflammation and intense pain. Tramadol is not often a first-choice treatment for migraine because it does not address inflammation related to migraine and has the potential to lead to the occurrence of medication overuse headaches.
The National Institute of Neurological Disorders and Stroke provides non-commercial data on the treatment methods of migraines, so patients know when pain relievers should be included in the overall therapy.
Toradol and tramadol are not suitable for chronic pain management on a long-term basis. Toradol is not safe in the case of long-term use because of the risk of kidney damage and bleeding. The use of Tramadol can be prolonged, but due to the dependency issues, the medication is not an appropriate long-term treatment for most patients.
Proper management of chronic pain typically entails physical therapy, behavioral health, lifestyle modifications, and occasionally, non-opioid drugs that have fewer adverse effects with extended usage. That is why contemporary pain treatment is devoted to the combination of treatment plans rather than pills.
Choosing between Toradol and tramadol is not only about how strong the medicine is. It is about your health history, your risk for dependency, and whether your pain is short-term or long-term. At Silicon Valley Recovery, we understand how pain treatment and substance use risks can overlap. In case you are running your life on pain medications or you are concerned that you are becoming an addict, then Silicon Valley Recovery can assist you in making the next step towards safer care.
Our team is aware of the pain treatment issues, the opioid exposure, and the support of recovery. Our customized courses ensure that our clients are treated for the physical pain and the emotional effects of taking the medication over a long period of time.
You do not cope with pain, fear, and uncertainty. Talk to a caring professional now and discover what support opportunities are available to assist you and your loved one. You may reach our admissions team and begin a healthier journey today!

In some healthcare settings, physicians may prescribe them together, but only under close supervision. Interactions between drugs can worsen the dosage effects and can only be advised by a professional.
NSAIDs, including Toradol, carry far less dependency risk than opioid medications like Tramadol. They are generally preferred as a first-line option when pain can be managed without opioids.
Toradol is usually limited to five days or less. Tramadol may be prescribed longer, but ongoing monitoring is essential. Long-term use of either medication should always be guided by a healthcare professional.
Tramadol may help some people, but it is not a first-choice solution for long-term chronic pain management. Non-opioid therapies, physical rehabilitation, and lifestyle adjustments are often more sustainable options.
Mixing Toradol with other NSAIDs increases the risk of bleeding and kidney problems. Always consult your healthcare provider before combining medications.
Developmental Coordination Disorder (DCD) is a neurodevelopmental condition that affects motor skills and coordination in children and can continue into adulthood. Although the exact causes of DCD are not fully understood, researchers believe that the condition is linked to abnormal brain development and is not caused by any physical illness or injury. DCD is often diagnosed in young kids when they struggle to learn how to walk, run, hold objects, or play sports.
It is estimated that up to six percent of children around the world have DCD, which makes this disorder quite common. While DCD cannot be fully cured, with a proper treatment plan, patients can learn to manage the symptoms of DCD and significantly improve their quality of life. In our article, we will explain the main symptoms of Developmental Coordination Disorder, discuss the ways DCD affects the life of a person diagnosed with this disorder, and provide a few effective treatment options.
![]()
Developmental Coordination Disorder (DCD), also known as dyspraxia, is a disorder that affects movement and coordination. This disorder is usually diagnosed in childhood when parents or caregivers of the child notice the kid is struggling to develop their motor skills. DCD is not related to the intelligence of the child—the disorder may be diagnosed in a seemingly healthy kid who meets their milestones yet has trouble with balance and coordination.
At the moment, there is no consensus within the medical community regarding the causes of developmental coordination disorder. It is possible that the disorder develops before the child is born due to the abnormal development of neurons in the brain. Some researchers have linked DCD to low birth weight and premature birth.
Here are a few signs of developmental coordination disorder you may notice in your child:
On top of the physical symptoms of DCD, kids with this disorder may have emotional and psychological issues—low self-esteem, difficulty making friends, and anxiety. For example, if a child cannot participate in sports activities together with their peers, it may negatively affect their mental health.
The diagnosis of Developmental Coordination Disorder should be made by a qualified medical professional—a doctor who specializes in pediatrics or a psychologist.
A healthcare provider will talk to the parents or caregivers of the child to learn more about their medical history and observe the child to see whether their movements are atypical for their age. There are several tests that can be performed to determine whether the child has DCD—for instance, the doctor may want to test the intelligence of the kid to see whether their cognitive functions are intact.
In general, DCD is diagnosed when a child is five years old. If you have reasons to believe your child has this disorder, talk to the doctor as soon as you detect the symptoms of DCD—the earlier the diagnosis is made, the sooner the child will start treatment.
Without proper treatment, Developmental Coordination Disorder may negatively impact the life of the diagnosed individual and persist into their adulthood. Here are a few challenges associated with DCD:
Poor Academic Performance: Children with DCD may struggle in school—their handwriting may be messy and illegible, they may have trouble focusing in class, and their low self-confidence will prevent them from participating in extracurricular activities
Health Issues: Kids with DCD are often incapable of taking part in physical activities and sports, which means they may lead a sedentary lifestyle. Moreover, there is always a risk of injury—for a child with poor balance and coordination, a simple task such as going up and down the stairs may end up in a fall.
Social Difficulties: It can be hard for a child with DCD to make friends and fit in with their peers. When your movement looks awkward and you cannot play with other kids, you may feel isolated and deal with bullying.
![]()
While there is no cure for developmental coordination disorder at the moment, there are several therapies parents can implement to help their children. Here are a few treatment options to consider:
Work With an Occupational Therapist
A certified occupational therapist will be able to teach the child skills they lack. The therapist will develop a personalized plan for the kid targeting the skills that require improvement—for example, if the child is unable to dress on their own, the therapist will focus on this skill
Introduce Physical Therapy
A physical therapist can assist the child and their parents in coming up with exercises that will be beneficial for the kid. Regular physical activity will help the child improve their strength, balance, and coordination.
Talk to a Psychologist
Children with DCD may need emotional support to cope with their diagnosis. A mental health provider will give the child tools to manage their stress and build their confidence.
Developmental Coordination Disorder (DCD) is a disorder that affects a person’s movement and coordination. This disorder is usually diagnosed in early childhood.
The most common signs of DCD are clumsiness (poor balance and difficulty holding objects), inability to master motor skills, and developmental delays.
A doctor should diagnose DCD after talking to the parents of the child and observing the child’s behavior. The diagnosis is typically made when the child is five years old.
There is no known cause of DCD. Some researchers believe the disorder develops before birth due to abnormal brain development, while others have linked DCD to premature birth.
It is possible to manage the symptoms of DCD with targeted therapy. Parents should work with occupational and physical therapists as well as enlist the help of a mental health provider to support their child.
Living with Developmental Coordination Disorder can be overwhelming for both children and their families—but you don’t have to navigate it alone. At Silicon Valley Recovery, our experienced team provides compassionate, individualized care to help individuals manage the emotional and psychological challenges that often accompany DCD. Whether you or your child is struggling with anxiety, low self-esteem, or co-occurring mental health concerns, we’re here to help. Contact Silicon Valley Recovery today to learn more about our treatment programs and take the first step toward a stronger, more confident future.
The opioid crisis has raised serious concerns about fentanyl contamination in the drug supply—including marijuana. As fentanyl continues to show up in unexpected substances, many people are asking: can weed be laced with fentanyl?
While fentanyl-laced weed may seem unlikely, reports of this dangerous combination have emerged in communities across the country. Knowing the symptoms, risks, and how to respond to a potential exposure could save your life or the life of someone you care about.
Below, we cover whether it’s possible to lace marijuana with fentanyl, the warning signs of exposure, and what steps to take in an emergency.
![]()
Yes, it is technically possible to lace weed with fentanyl. Because fentanyl is water-soluble, it can be dissolved and sprayed onto cannabis leaves—often without any visible trace. While the full effects of smoking fentanyl-laced marijuana are still being studied, inhaling or ingesting fentanyl in any form carries severe health risks, including fatal overdose.
Fentanyl is extraordinarily potent. A dose as small as 2 milligrams can be lethal, and the substance is roughly 50 times stronger than heroin. Because it is both odorless and colorless, a person could consume fentanyl-laced weed without realizing it—even if they are experienced cannabis users with a high tolerance.
There are several reasons marijuana may be laced with fentanyl, despite the obvious danger:
Whether you use marijuana recreationally or medicinally, it’s important to recognize the warning signs of fentanyl exposure. If you experience any of the following symptoms after smoking cannabis, seek help immediately:
Consuming marijuana that has been contaminated with fentanyl poses several serious risks:
![]()
If you suspect that your marijuana was laced with fentanyl and you or someone nearby is showing signs of an overdose, take these steps:
Yes. Fentanyl can be dissolved in liquid and sprayed onto cannabis during cultivation or packaging. Because fentanyl is odorless and colorless, contaminated weed may look and smell identical to uncontaminated product.
You typically cannot tell by appearance alone. However, symptoms like nausea, dizziness, difficulty breathing, and confusion after smoking cannabis may indicate fentanyl contamination. Fentanyl test strips offer a reliable way to check your supply before use.
The primary risks include opioid addiction, respiratory failure, and fatal overdose. Even a small amount of fentanyl can be lethal, making contaminated cannabis extremely dangerous.
Common reasons include enhancing the drug’s potency, creating customer dependency to boost sales, or feeding an existing opioid addiction. In many cases, the end user has no idea their marijuana has been tampered with.
Stop smoking immediately, preserve any remaining product, and monitor for overdose symptoms such as slow breathing, confusion, or loss of consciousness. Administer naloxone if available and call 911 if symptoms are severe. Seek medical care even if symptoms seem mild, as fentanyl effects can escalate quickly.
If you or a loved one has been affected by fentanyl exposure or is struggling with substance use, Silicon Valley Recovery is here to help. Our compassionate team provides evidence-based treatment for opioid addiction and co-occurring disorders in a supportive, confidential environment. Contact us today to learn about your options and take the first step toward recovery.
Fentanyl, a potent synthetic opioid, is used in medical settings to manage severe pain, especially after surgeries or for chronic pain conditions. However, like many opioids, fentanyl has a range of side effects, including addiction, when misused. One of the unexpected side effects of fentanyl is itchiness, which causes discomfort for patients taking this medication.
If you or your loved one is affected by this issue, you may want to know why fentanyl makes you itch and what you can do to address this problem. Our guide will explain the connection between fentanyl use and itchy skin and offer tips to manage this side effect.
![]()
It is not uncommon for patients to experience itchy skin after taking fentanyl or other opioids. This side effect is usually linked to the way opioids affect our bodies on the chemical level.
Fentanyl binds to the opioid receptors in our brains, blocking the pain but also triggering the release of histamine. While histamine is a natural chemical released by our bodies to get rid of allergies, an increase in histamine levels is often associated with itching, hives, and headaches.
There is a difference between normal itching caused by histamine release and an allergic reaction to fentanyl. While allergies to fentanyl are rare, you should be aware of the symptoms of an allergic reaction to this medication:
● Itchy skin and hives
● Skin rash
● Swelling of the face and neck
● Breathing difficulties
If you believe you are allergic to fentanyl, inform your healthcare provider and seek alternative pain management treatments.
Thankfully, you can tackle the itching from fentanyl with a few simple solutions:
● Moisturize your skin. Apply lotion to your skin at least once a day to prevent dryness and reduce itching.
● Use antihistamines. Over-the-counter antihistamines can be very effective against itching. Talk to your doctor to find the right antihistamines for you.
● Refrain from scratching. It may be tempting to scratch your skin when it itches, but this will only aggravate your condition, leading to skin infections and damage.
While mild itching is not dangerous, you should bring up this side effect during your next visit to the doctor and ask if you should continue taking fentanyl.
If the itching does not go away and is accompanied by other symptoms (nausea, dizziness, breathing problems, chest pain, etc.), seek medical help as soon as possible. A doctor will examine you, prescribe you medications to deal with the side effects, and suggest alternatives to fentanyl.
![]()
Yes, fentanyl stimulates the release of histamine in your body, which leads to itchy skin.
Apart from itching, fentanyl use is associated with such side effects as nausea, constipation, drowsiness, confusion, and breathing difficulties.
In most cases, the itching will subside within a few hours. If the itching persists, talk to your doctor about discontinuing fentanyl.
You can reduce the itching by taking antihistamines, keeping your skin moisturized, and avoiding hot showers.
While it is uncommon, some people are allergic to fentanyl. If you break out in hives and have trouble breathing after taking fentanyl, seek medical attention immediately
Itching is a fairly common side effect of fentanyl, and while it does not pose a threat to your health, it can be quite annoying. Luckily, you can manage this symptom if you know the reason behind the itching and have the right tools to treat it.
If you are planning to take fentanyl or have already started taking it, our team at Silicon Valley Recovery is ready to assist you. Contact Silicon Valley Recovery today and let our experts help you build a personalized treatment plan!
Heroin is a highly addictive and illegal substance derived from morphine, a natural compound found in the seed pods of the opium poppy. Recognizing heroin in its various forms can be a crucial step in identifying potential drug abuse in a friend or a loved one. The appearance of heroin can vary depending on its purity and the additives used by drug manufacturers to dilute the product and increase their profits.
In this blog, we will answer the question “What does heroin look like?”, describe all the main variations of this drug, and explain the risks associated with heroin abuse. If you or someone you care about is struggling with heroin addiction, reach out to Silicon Valley Recovery to get professional help and support.
Heroin is a drug made from morphine, a substance naturally found in opium poppy plants. In most cases, this illegal drug looks like a powder or resin and comes in a variety of colors from white to black. The color and texture of heroin depend on the method of manufacturing and the additives included in the final product.
Below you will find a detailed description of the three main types of heroin—brown, white, and black tar—and their unique characteristics. Keep in mind that while the color and the look of heroin can tell you a lot about its purity, even the purest form of heroin is extremely dangerous to your health.
As the name suggests, brown heroin is a light brown or beige powder. This type of heroin is usually made with morphine that was not fully refined, which gives the powder its distinctive brown color. Sometimes additives like caffeine, sugar, or lactose are mixed in during the manufacturing process to increase the volume of the product.
Brown powder heroin is usually smoked instead of injected. Compared to white powder heroin, this type is less refined and therefore less potent. Nonetheless, brown heroin is still an addictive and dangerous drug that can lead to many negative health consequences.
White heroin is typically found far away from its place of origin since this type of heroin is considered to be the purest form of the drug. It is made from heavily refined morphine and usually contains few additives, which makes it more potent compared to brown heroin. In addition, white powder heroin easily dissolves in liquid, making it perfect for injection.
It may be difficult to identify white heroin since it closely resembles many innocent substances, such as sugar, salt, baking soda, and certain medications. Pay attention to the behavior of your friend or family member—if they exhibit any symptoms of heroin abuse, you should reach out to them and contact an addiction specialist.
Black tar heroin looks quite different from brown and white powder heroin. Instead of a fine powder, black heroin resembles a piece of resin or rock. It can be dark brown or black, solid or sticky to the touch. This type of heroin is usually made in Mexico and sold and consumed in North America.
Due to the cheap and quick method of manufacturing, black tar heroin is an impure form of heroin. It is usually injected directly into the bloodstream—the insoluble impurities present in the drug can lead to collapsed veins, inflamed and infected arteries, and serious infections such as tetanus and sepsis.
Here are some of the most common symptoms of heroin abuse you may notice in a person who struggles with addiction
Heroin is one of the most addictive drugs in the world—it only takes a few doses for a person to develop a mental and physical dependency on the substance. Here are a few reasons to be concerned about heroin abuse
Heroin usually comes in powder form, though in some cases it may look like a rock or a piece of coal. The color of heroin varies from white to black depending on its purity.
There are three main types of heroin: brown powder heroin (an unrefined form of heroin with additives), white powder heroin (the purest and most potent type of heroin), and black tar heroin (an impure sticky substance with many additives).
The initial symptoms of heroin abuse include short-term euphoria, drowsiness, confusion, agitation, and nausea. If you suspect someone you know is taking heroin, talk to them and encourage them to see a doctor.
Yes, it is possible to overcome heroin addiction with therapy and medication. You should reach out to a certified healthcare provider to come up with a personalized treatment plan that suits the patient and their unique circumstances.
There are several things you can do to support a heroin user: educate them about the dangers of drug consumption, be there for them when they need to talk, and accompany them to the rehab center to get the treatment they need.
Whether you have spotted heroin in your house or noticed worrying behavior of your loved one, recognizing the drug and the symptoms of its use is only the first step. Get in touch with Silicon Valley Recovery—our team of addiction experts will be able to diagnose the issue, assist the patient in crisis, and come up with a tailored treatment plan for long-term recovery.
To the members of the 1970s and 1980s generations, “Quaalude” had become a colloquialism of the club scene and the recreational drug culture in the 1970s and 1980s. To the younger generations, the name might just be known through movies or documentaries of that time. However, the knowledge of what Quaaludes are and why they became so harmful is also topical today, as one can learn about addiction and pharmaceutical control and the impact of the mass abuse of drugs.
Quaaludes were also prescribed as a presumably safe substitute for barbiturates in the treatment of insomnia and anxiety. This resulted in their rapid popularity as a recreational drug with disastrous consequences, such as mass dependence on Quaalude, overdose fatalities, and eventually, their total separation from the pharmaceutical market. Quaalude’s history provides valuable clues about how depressant drugs may become instruments of medicine and health disasters in the hands of the people.
Methaqualone (brand name Quaaludes) was a synthetic hypnotic-sedative drug that was initially produced in India in 1951. The drug was originally meant to be a safer substitute for barbiturates, which had a high potential for overdose and extremely harmful withdrawal effects. In 1965, methaqualone was introduced into the pharmaceutical market of America under different brand names, Quaalude being the most popular.
The mechanism of action of methaqualone is an increase in the gamma-aminobutyric acid (GABA) activity in the brain, which causes the feeling of euphoria, relaxation of the muscles, and sedation. This chemical structure enabled it to cross the blood-brain barrier quickly and produce immediate Quaalude effects that users found enjoyable. Methaqualone has the following major properties:

While Quaaludes belong to the same sedative-hypnotic category as barbiturates and benzodiazepines, there are critical distinctions. By contrast, methaqualone was thought to have a broader therapeutic-to-fatal ratio than barbiturates. Contrary to benzodiazepines, which would subsequently take over both groups, methaqualone generated increased euphoria, which is one of the reasons why it has the potential to be abused.
The history of Quaaludes in America is no exception, as the trajectory is familiar: first promoted as being safe, then most people began abusing it, and then the government decided to step in. This can be shown on the following timeline:
The Drug Enforcement Administration (DEA) declared that methaqualone would be placed on Schedule I because the drug was found to have a high abuse potential and there was no established medical use of the drug in the United States.
To learn about the Quaalude effect, it is necessary to consider the interaction between the drug and the central nervous system. Methaqualone is a depressant drug, like other such drugs, which decelerates brain activity, a process leading to varying degrees of physical and psychological effects depending on the drug’s dosage.
The mechanism of action of methaqualone has been described as sedative-hypnotic because of its connection with the GABA receptors in the brain. The drug activates GABA, resulting in the following effects that users normally feel in phases:
Abuse of Quaalude became a kind of an epidemic in the 1970s and early 1980s due to a mix of individual pharmacology, culture, and the failure of initial regulation.
By the mid-70s, Quaaludes had become a non-prescription sleep drug and a common recreational drug. The disinhibiting properties of the drug were adopted by the disco era, and it was given such names as disco biscuits and ludes. The recreational users treasured the drug as it made them feel relaxed and euphoric and also not as heavily sedated as barbiturates.
The Quaalude epidemic was facilitated by a number of social and regulatory factors. Factors that contributed to the same were the following:
The addiction to Quaalude evolved quickly among many people who took it because the drug has a euphoric effect, and they became addicted to Quaalude as a result of using the drug frequently. Identifying symptoms of addiction was crucial so that the condition could be addressed promptly.
The table below presents the physical and mental symptoms of addiction to Quaalude:
| Physical Signs | Psychological Signs |
| Increasing tolerance requires higher doses. | Obsession with taking and using the drug. |
| Sleepiness and lack of coordination. | Continued use despite negative effects on relationships or work. |
| Diffused speech and retarded reflexes. | Anxiety or irritability when unable to use. |
| Between doses, nausea and headaches. | Unsuccessful efforts to reduce or quit consumption. |
| Sleep disturbances without the drug. | Loss of interest in previously enjoyed activities. |
| Physical dependence requires the drug to feel normal. | Denial of the severity of use or its consequences. |
The withdrawal of Quaalude may be intense and even fatal, just like the withdrawal of other sedative-hypnotic drugs. The body had adapted to the chronic use of methaqualone, and therefore, when it was stopped at once, a rebound effect occurred as the nervous system was overcorrecting.

According to the National Institute on Drug Abuse (NIDA), withdrawal symptoms of sedative-hypnotic drugs may be unsafe and have to be monitored by a doctor during the detoxification process.
The withdrawal of Quaaludes is a condition that needs a meticulous approach to medical care since it is prone to serious complications. In general, the symptoms were usually the following:
Medical detoxification was usually performed through a gradual reduction of dose or replacement with longer-acting tranquilizers to avoid the high-risk withdrawal effects.
The ban on Quaaludes was brought about by widespread evidence of harm, coupled with the fact that other safer alternatives were available. By the early 80s, the extent of abuse on Quaalude was so extensive that the drug was practically ignored by the medical fraternity and replaced by benzodiazepines.
Some of the reasons that caused the ban were the reported deaths associated with the overdose; the drug was also linked with sexual assault; the drug was diverted to the illegal market in large numbers; and the availability of alternative drugs with safer profiles. Legal production and prescription in the United States were practically terminated when the schedule was reclassified in 1984 to Schedule I.
Although Quaaludes are no longer legal, the experience of the methaqualone epidemic is used in the current practice of treating addiction to depressant drugs. A lot of the principles that underlie the treatment of withdrawals after benzodiazepine or alcohol addiction also work in the case of a person who might still be facing the problem of dependency on sedatives.
Silicon Valley Recovery offers comprehensive treatment for substance use disorders, including addiction to sedative-hypnotic substances. To treat physical and psychological components of addiction, we use our evidence-based practice that involves medical detoxification, individual and group therapy, and long-term recovery planning.
If you or someone you love is struggling with addiction, help is available. Contact Silicon Valley Recovery today to learn about our treatment programs.
Yes, with the euphoric effects of methaqualone, psychological dependence could develop even after limited recreational use. It usually takes weeks of regular use, and the urge to repeat the experience might cause addictive patterns within a short time.
Quaalude and alcohol withdrawal share many symptoms because both substances affect the brain’s GABA system, such as anxiety, tremor, sweating, and seizure susceptibility. The time and the intensity may be different, although the two necessitated medical care because of their life-threatening complications.
Methaqualone was a strong euphoriant and a strong sedative, and thus more euphoric than most of the depressants. This combination of enjoyment and rest drove users to repeat more often, and this quickened the process of addiction.
Sedative-hypnotic abuse in chronic abuse may have long-term consequences on memory, cognition, and emotional regulation, although most people improve significantly with abstinence. There are a few long-term studies that are specific to methaqualone, though it can be expected that it has effects comparable to other members of the same kind.
The physical dependence is treated using medical detoxification using gradual tapering or substitution therapy, and the cravings are treated using behavioral therapies such as cognitive behavioral therapy, which prevent a relapse. Full-time intervention that is done for both perspectives has the best long-term results.
Searching for “heroin detox centers near me” is a crucial first step toward recovery. Heroin addiction is a serious medical condition that can affect your physical and mental health, personal and professional life, and future prospects. Heroin withdrawal is extremely challenging and dangerous to manage without professional support.
In this guide, we will help you understand the importance of finding a heroin detox center near you, the benefits of medical detox, the main factors to consider when choosing a rehab facility, and the advantages of ongoing addiction treatment. Overcoming heroin addiction may be difficult—but with the right help, recovery is possible.

Heroin detox is the process of removing all traces of the drug from your system and managing the resulting withdrawal symptoms. When you suddenly quit heroin after developing a dependency, your body reacts negatively, leading to a wide range of physical and psychological symptoms—from nausea and muscle pain to depression and insomnia.
The purpose of heroin detox is twofold. First, you need to go through withdrawal to start your recovery journey. Second, you need to establish the foundation for avoiding heroin in the future. Attempting to go through withdrawal without medical assistance is dangerous—you should rely on the expertise of addiction specialists to keep you safe and comfortable.
There are many benefits to enrolling in a professional detox program instead of trying to quit heroin on your own.
Safe environment. Detox centers offer a controlled setting where patients can go through withdrawal under the supervision of trained medical professionals.
Withdrawal management. Doctors can prescribe medication to alleviate withdrawal symptoms and help patients feel more comfortable throughout the process.
Medication-Assisted Treatment (MAT). Certain medications, such as Methadone and Buprenorphine, can be used to reduce cravings and prevent relapse.
Psychological support. In addition to treating the physical symptoms of withdrawal, patients can work with therapists and counselors to address the root causes of their addiction.
Here are a few factors you may want to consider when selecting a detox facility.
Location. Is the center close to your home? Is it easy to reach? Will your family be able to visit you while you are undergoing treatment?
Accreditation. Is the facility licensed to provide addiction treatment? Does the medical staff have the necessary credentials?
Treatment options. Does the center offer the program you need? Can you get medication-assisted treatment for heroin addiction?
Cost. Will your insurance provider cover the treatment? Can the facility offer you a payment plan?
In addition to joining a detox program, you can expand your support network by relying on local resources.
Support groups. Join a local chapter of Narcotics Anonymous (NA) to share your struggles and achievements with people who will understand you and support your recovery.
Therapy. Find a licensed therapist in your area and attend individual and family therapy sessions to address the mental health aspects of addiction.
Healthcare provider. Talk to your doctor about your substance use disorder—you may receive valuable tips on recovery and prescriptions for medication you may need.

Detox is only the first step on the path to long-term recovery. If you were enrolled in a short inpatient or outpatient detox program, you should continue your treatment after you are done with withdrawal.
Preventing relapse. Your chances of avoiding heroin in the future are much higher if you continue going to therapy and benefiting from medication-assisted treatment.
Addressing co-occurring disorders. If your addiction was preceded or caused by mental health issues such as anxiety or depression, you should work with a therapist to improve your mental health.
Building a support network. From joining local support groups to attending therapy with your family members—surround yourself with people who will help you remain sober.
Heroin detox is the process of ceasing drug intake and eliminating it from your body. It is usually accompanied by withdrawal symptoms—physical and psychological reactions of your body to the lack of heroin.
2. What are the symptoms of heroin withdrawal?
Heroin withdrawal symptoms may include nausea, vomiting, muscle aches, shaking, anxiety, agitation, depression, insomnia, high blood pressure, and increased heart rate.
3. Should I enroll in a heroin detox program?
It is recommended to undergo heroin withdrawal under the supervision of medical professionals. This way, you will have access to the medication you need and receive psychological support from therapists and counselors.
4. What are the benefits of medical detox for heroin addiction?
Medical detox allows you to quit heroin in a safe environment under medical supervision, manage withdrawal symptoms with the help of prescribed medications, and get psychological support from mental health professionals.
5. What should I do after completing a heroin detox program?
To increase your chances of recovery, you should continue your treatment after detox. Attend therapy sessions, rely on the support of your friends and family, and join a local support group to connect with people who will understand your struggles.
We hope this guide has helped you realize the importance of finding a heroin detox center near you and enrolling in a detox program to overcome your addiction. Detox allows you to quit substance use in a safe environment under medical supervision—give yourself the best chance of recovery.
Reach out to Silicon Valley Recovery to learn more about our heroin detox and treatment programs. Our team is here to provide you with the guidance and support you need to overcome addiction. You can conquer heroin addiction and return to a healthy and happy life.
Dissociation may seem disturbing, worrisome, and lonely. Most of the individuals also lament that they are not related to their bodies, their feelings, the world around them, or even their identity. Although you might always wonder how to come out of dissociation, it is interesting to note that dissociation is not an inability on the part of an individual, but it is a form of defense mechanism that the brain acquired as a way of coping with excessive stress or trauma.
Dissociation is a challenging condition that is also curable. The proper grounding strategies will allow returning to the present in the long run and take the feeling of control and safety with the help of mindfulness training, treatment choices, and coping strategies.
Dissociation is a psychological response that occurs when the mind isolates problematic thoughts, feelings, or emotions, or sensations. It is typically a defense mechanism during periods of extreme stress or trauma, or being overloaded with emotions.
As far as the issue of mental health is concerned, the dissociation is on a continuum. Mild cases of dissociation, such as daydreaming or zoning out, are normal. Worse ones may be a lack of actuality, time wasting, or even numbness.
Dissociation is generally related to:
One such step towards curing is the knowledge of the fact that dissociation is something that happens and not a fault of shame upon herself, and knowledge helps to alleviate fear and shame, and this constitutes a very important step towards healing.
Situations that bring to mind a past dangerous situation, even in the absence of a real danger, can usually cause dissociation episodes.
Common triggers include:
The recognition of triggers enhances self-awareness practices and enables early intervention, which uses grounding and stress management techniques.
Dissociation may occur in physical and emotional organs and levels, and sometimes it is hard to identify such in real-time.
Physical signs may include:
Emotional signs may include:
Grounding techniques are effective tools that help reconnect the mind and body to the present moment. They can be the best quick solution to the question of how to stop dissociating.
Before enumerating certain techniques, it should be noted what they aim to achieve: grounding is a technique that shifts gears towards external reality and helps forget internal distress.
Examples of effective grounding techniques are:
Although grounding techniques can be beneficial in the immediate, mindfulness activities can be used to support the process of awareness and emotional regulation in the long term.
Mindfulness does not mean pushing the thoughts out of mind, it is only about not judging the thoughts. In dissociative people, mindfulness develops an ability to tolerate the experience of the present gradually and in a controlled manner.
Some beneficial mindfulness exercises are:
Dissociation in many people is based on unresolved trauma, ongoing stress, or emotional difficulties. Although coping mechanisms are beneficial, treatment alternatives aim at the root of the problem.

Dissociation is a condition that is usually treated using evidence-based therapies that include:
The recovery of dissociation in the long term consists of enhancing emotional control, stress management, and self-connection. Such abilities make dependence on dissociation as a coping mechanism less needy.
Certainly, strategies are best described in advance, but it is worth stating that consistency is more significant than perfection.
Recent coping strategies that can be effective in the long term are:
These exercises assist the nervous system over time in making it feel secure and more robust.
Dissociation usually occurs with substance use, trauma, anxiety, and depression. At Silicon Valley Recovery, care is provided to the entire individual- not only to the symptoms.
Recovery does not mean forcing oneself out of it. It is all about coming to know how to be safe in your body.
Dissociation is not something that you must go through on your own, in case it is interfering with your everyday life or recovery.
Contact Silicon Valley Recovery today and receive compassionate, professional mental health support. Healing begins with support.

Trauma, stressful life, anxiety, or excessive emotional experiences tend to cause dissociation. It is formed as a self-defense reaction when the nervous system becomes insecure.
The techniques involving the senses, or, to be more precise, naming objects in the room or paying attention to physical sensations, are often the most efficient. Their effectiveness gets better with practice.
Mindfulness develops awareness of thoughts, emotions, and body sensations without the element of judgment. With time, it becomes more tolerant of present moment experience and decreases dissociative response.
The most common types of trauma-informed therapies include EMDR, DBT, and cognitive behavioral treatments. These treatments are focused on the symptoms and causes.
Dissociation should be treated with professional assistance in case it is common, traumatizing, and disruptive to everyday life. The symptoms and general life quality can be improved with the help of support.
When it comes to identifying heroin, many people wonder whether this illegal drug has a distinctive aroma. Noticing an unusual smell in your house or car can be an important first step in preventing heroin abuse and addiction. However, heroin comes in many forms, and some varieties of this drug are nearly odorless.
In our article, we will explain whether heroin has a smell, describe its scent, and list the main signs of heroin use you should be aware of. We will also discuss the dangers of heroin addiction and offer you a path toward a safe and quick recovery. Heroin use disorder is a serious mental health condition—make sure to reach out to Silicon Valley Recovery if you or your loved ones need professional help.
![]()
Yes, heroin does have a smell, though its aroma may not be too strong or easy to recognize, especially if you have never encountered this drug before. Typically, unrefined heroin, such as black tar heroin, has a noticeable acidic smell, while pure white heroin may be completely free of any scent.
It may be challenging to identify heroin solely by its smell—nonetheless, this drug has a unique aroma that may alert you to its presence. Pay attention to the unusual chemical smell in your residence or vehicle, and combined with other signs of heroin use, you may be able to determine that a friend or a family member is abusing this drug.
The scent of heroin depends on its type and purity. Here are the most common types of heroin and their smell:
While it may be tricky to figure out what heroin smells like if you have never felt its aroma before, there are a few methods you can try to recognize its scent:
The smell of heroin is only one of the signs that a person may be using this drug. Here are a few common symptoms of heroin abuse you may notice:
![]()
Heroin is an illegal, highly addictive substance—its use may lead to a myriad of physical and mental health problems. Here are a few reasons to be concerned about heroin addiction:
Heroin does have a smell, though its scent varies based on the type of heroin—while black tar heroin has a strong smell, white heroin may be odorless.
The smell of heroin is often described as vinegary or acidic—its aroma is similar to the smell of many cleaning chemicals.
You can recognize heroin by its pungent smell—if you feel an unusual acrid smell in your house and cannot explain its origin, consider this may be heroin.
In addition to the smell of heroin, you may notice a person is abusing the drug if they have drug paraphernalia in their possession and display physical and mental symptoms of drug use.
Heroin addiction may have devastating consequences for a person—this drug negatively affects both the body and the mind and increases the risk of premature death.
We hope that our guide was able to help you figure out the smell of heroin and recognize its presence in your home. While noticing the odor of heroin may alert you to the problem, it is crucial to pay attention to other symptoms of heroin abuse and get help for yourself or your loved one.
Reach out to Silicon Valley Recovery to get in touch with mental health professionals who will be able to assist you. Our experts will design a personalized treatment plan for you and support you during your recovery journey.
Suboxone is a prescription medication utilized in the treatment of opioid addiction and is an important step in the recovery journey for many individuals who struggle with substance use disorder. One of the main benefits of Suboxone is its ability to block the effects of opioids—but how long does Suboxone block opioids, and what are the exact advantages of this medication?
In our article, we will explain the duration of Suboxone effects, list the factors that may change how long Suboxone stays in a person’s system, and talk about the benefits of this medication in addiction treatment. We will also answer the most frequently asked questions on this topic and provide you with guidance on incorporating Suboxone into your recovery journey.
![]()
Suboxone is a medication used to treat opioid addiction. It combines buprenorphine (a partial opioid agonist that blocks the negative effects of opioid drugs) and naloxone (an opioid antagonist that prevents misuse of medication.) Suboxone helps people reduce opioid cravings and withdrawal symptoms and can be used during medically supervised detox as well as long-term maintenance treatment.
On average, Suboxone can block the effects of opioid drugs for 12-24 hours. The exact duration of Suboxone effects will depend on a few factors we have listed below—some people will stop experiencing the impact of Suboxone only 6 hours after taking the medication, while others will feel its effects for 2 full days. Your doctor will be able to prescribe you the proper dosage of Suboxone and adjust it to suit your needs.
Here are the main factors that play a role in how long Suboxone will remain in your system:
![]()
Proper Suboxone usage under the supervision of a qualified healthcare provider can be very advantageous for a person who suffers from opioid addiction:
Suboxone is usually taken sublingually (a person puts a Suboxone tablet or film under their tongue to let it dissolve). You will feel the effects of the medication 20-70 minutes after you take it.
There is no fixed duration for Suboxone therapy—some patients take it for a few days during detox to manage withdrawal, while others remain on Suboxone treatment for several years. Consult with your doctor to determine the best course of action for your recovery.
It is highly inadvisable to combine Suboxone and opioid drugs—this may lead to serious side effects (intense headaches, high blood pressure, and accelerated heart rate) and increase the risk of a drug overdose.
There may be adverse effects you experience after taking Suboxone: headaches, nausea, insomnia, pain in muscles and joints, fatigue, fever, and mood swings. If you suffer from these symptoms, reach out to your doctor—they may decide to lower your Suboxone dosage or discontinue this medication.
The main advantages of Suboxone include the prevention of withdrawal symptoms, a gradual reduction in drug cravings, and a lower probability of drug misuse in the future. This medication will help you restore normalcy in your life without the negative influence of substance abuse.
We hope that our guide was able to explain the purpose of Suboxone treatment and its benefits for a person who struggles with opioid addiction. This medication will block the effects of drugs on your brain, help you cope with withdrawal, and put you on the path to recovery.
In case you are looking for professionals to assist you with Suboxone therapy and build a personalized treatment plan for yourself or your loved one, get in touch with Silicon Valley Recovery. Our team will be happy to answer your questions about Suboxone and support you on your recovery journey.
Sleep disturbances rank among the most challenging aspects of opioid recovery. When you stop using opioids after prolonged use, your body undergoes significant adjustments that frequently disrupt normal sleep patterns. Opioid withdrawal insomnia affects countless individuals working toward recovery, creating exhaustion that compounds an already difficult process.
Understanding why insomnia occurs during withdrawal and knowing how to manage it can make a meaningful difference in your recovery journey. Poor sleep doesn’t just leave you tired. It affects judgment, increases stress and raises relapse risk. Addressing sleep problems proactively supports both short-term comfort and long-term success in overcoming opioid dependence.
![]()
Opioids target specific receptors in the brain, altering how the central nervous system functions. These drugs are commonly prescribed for moderate to severe pain management, but their euphoric effects contribute to high addiction potential. In 2020, approximately 2.7 million people in the United States were diagnosed with opioid use disorder, reflecting the widespread nature of this public health challenge.
When someone uses opioids regularly, their brain chemistry adapts to the presence of these substances. The body becomes accustomed to functioning with opioids influencing neurotransmitter activity, sleep-wake cycles and stress responses. Once opioid use stops, the body must readjust to operating without these drugs, a process that produces various withdrawal symptoms.
Sleep disturbances emerge as a common withdrawal symptom because opioids significantly affect the central nervous system’s regulation of sleep. While actively using opioids, many people experience increased drowsiness and sleep more than usual. During withdrawal, this pattern reverses dramatically. The brain’s sleep regulation systems, no longer suppressed by opioids, often overcorrect, producing insomnia, restlessness and difficulty achieving restful sleep.
Psychological symptoms accompanying withdrawal also contribute to sleep problems. Anxiety, agitation, depression and racing thoughts make relaxing into sleep difficult. Physical discomfort from other withdrawal symptoms, including muscle aches, sweating and restlessness, further interferes with the ability to fall and stay asleep.
The duration of withdrawal-related insomnia varies considerably between individuals. No fixed timeline applies to everyone, as multiple factors influence how long sleep disturbances persist. On average, acute insomnia lasts approximately one to two weeks after the last opioid dose. However, some individuals experience sleep difficulties lasting several months, particularly those recovering from long-term or high-dose opioid use.
Factors Affecting Insomnia Duration
| Factor | Impact on Sleep Recovery | Considerations |
|---|---|---|
| Type of opioid used | Short-acting opioids clear faster; long-acting opioids may cause prolonged symptoms | Heroin, codeine vs. methadone, extended-release formulations |
| Duration of use | Longer use periods typically mean longer adjustment times | Years of use requires more extensive brain readjustment |
| Dosage levels | Higher doses create greater physiological dependence | Tapering may reduce symptom severity |
| Previous sleep patterns | Pre-existing sleep issues may complicate recovery | Address underlying sleep disorders separately |
| Access to treatment | Professional support improves outcomes | Medications and therapy accelerate improvement |
| Overall health status | Better general health supports faster recovery | Nutrition, exercise and stress management matter |
Healthcare providers can assess individual circumstances and provide personalized recommendations for managing insomnia duration and severity. Working with professionals who understand both addiction medicine and sleep health produces the best outcomes.
Managing withdrawal insomnia requires a comprehensive approach addressing physical comfort, behavioral habits and professional support. These strategies can help improve sleep quality during this challenging period.
Consult with healthcare providers. Medical professionals offer invaluable guidance tailored to your specific situation. Doctors can prescribe appropriate medications to assist with sleep while ensuring these treatments don’t interfere with recovery goals. Both over-the-counter and prescription options may help, but professional guidance ensures safety and effectiveness. Don’t hesitate to reach out if insomnia persists beyond a few days.
Optimize your sleep environment. Creating conditions conducive to sleep supports your body’s natural rest mechanisms. Keep your bedroom cool, as lower temperatures promote better sleep. Invest in comfortable bedding that supports physical relaxation. Minimize light exposure, particularly blue light from electronic devices, in the hours before bedtime. Consider blackout curtains, white noise machines or other environmental modifications that promote restfulness.
Establish consistent sleep habits. Maintaining regular sleep and wake times helps regulate your body’s internal clock, even when sleep feels elusive. Go to bed and wake up at the same times daily, including weekends. This consistency trains your body to expect sleep at appropriate times.
Practice relaxation techniques. Calming activities before bed help transition your mind and body toward sleep. Consider deep breathing exercises, progressive muscle relaxation, gentle stretching, meditation, aromatherapy with lavender or chamomile, warm baths, journaling to process thoughts and emotions, or listening to calming music. Experiment with different approaches to discover what works best for you.
Limit stimulants and sleep disruptors. Avoid caffeine, nicotine and heavy meals in the hours before bedtime. While alcohol might seem to promote sleep initially, it actually disrupts sleep quality and should be avoided during recovery.
![]()
Sleep quality directly impacts recovery success in multiple ways. Understanding these connections emphasizes why addressing insomnia matters beyond simple comfort.
Impact of Sleep on Recovery Outcomes
| Sleep Status | Effects on Recovery | Long-Term Implications |
|---|---|---|
| Adequate sleep | Improved cognitive function, stable mood, sufficient energy for treatment participation | Better treatment adherence, stronger coping skills |
| Mild insomnia | Increased irritability, reduced concentration, moderate fatigue | May slow progress but manageable with intervention |
| Severe insomnia | Impaired judgment, heightened anxiety and depression, exhaustion | Significantly elevated relapse risk |
Research consistently demonstrates connections between sleep disturbances and opioid relapse. Patients struggling with insomnia during and after withdrawal show higher rates of returning to drug use. This relationship likely reflects multiple factors. Sleep deprivation impairs decision-making abilities, increases emotional reactivity, reduces stress tolerance and diminishes motivation for recovery activities.
When you’re well-rested, you’re better equipped to engage in treatment programs, practice coping skills and resist cravings. Cognitive performance improves, mood stabilizes and you have energy to invest in building a drug-free life. Prioritizing sleep isn’t self-indulgence during recovery. It’s an essential component of successful treatment.
A few sleepless nights during early withdrawal, while uncomfortable, typically don’t require immediate intervention. Short-term insomnia resolves for most people as acute withdrawal symptoms subside. However, certain situations warrant professional attention.
Seek help if insomnia persists beyond one to two weeks without improvement. Contact a healthcare provider if you experience signs of significant sleep deprivation including severe irritability, inability to concentrate, dizziness, confusion or emotional instability. Reach out immediately if sleep problems contribute to thoughts of using opioids again or if you’re struggling to participate in recovery activities due to exhaustion.
Healthcare providers can diagnose underlying causes of persistent insomnia and prescribe appropriate treatments. Mental health professionals offer additional support, teaching coping skills, relaxation techniques and lifestyle modifications that promote better sleep. Comprehensive treatment addresses both the physical and psychological aspects of withdrawal insomnia.
Opioid withdrawal insomnia presents real challenges, but you don’t have to face them alone. Professional support makes a meaningful difference in managing sleep disturbances and building a foundation for lasting recovery. Silicon Valley Recovery Center provides comprehensive addiction treatment programs that address the full spectrum of withdrawal symptoms, including sleep difficulties. Our experienced team understands the connection between quality sleep and successful recovery, offering evidence-based approaches to help you rest better and recover stronger. Contact Silicon Valley Recovery Center today to learn how our programs can support your journey toward an opioid-free life.
1. What are the common symptoms of opioid withdrawal?
Opioid withdrawal produces both physical and psychological symptoms. Physical symptoms include muscle aches, nausea, vomiting, diarrhea, sweating, hot and cold flashes, runny nose and increased heart rate. Psychological symptoms include anxiety, irritability, agitation, depression, difficulty concentrating and insomnia. Symptom severity varies based on the type of opioid used, duration of use and individual factors.
2. How long does opioid withdrawal insomnia typically last?
Opioid withdrawal insomnia duration varies considerably between individuals. On average, acute sleep disturbances last one to two weeks after stopping opioid use. However, some people experience sleep difficulties for several months, particularly those recovering from long-term or high-dose use. Factors influencing duration include the specific opioid used, length of use, dosage levels and access to professional treatment.
3. Can medications help treat insomnia during opioid withdrawal?
Yes, various medications can help manage withdrawal insomnia when prescribed by healthcare providers. Options may include sleep aids, anti-anxiety medications or other treatments tailored to individual needs. Medical supervision ensures these medications support rather than interfere with recovery goals. Never take sleep medications without consulting a doctor, as some substances may complicate opioid recovery.
4. Why is addressing insomnia important for opioid recovery success?
Sleep quality directly impacts recovery outcomes. Research shows that patients struggling with insomnia during withdrawal face higher relapse rates. Sleep deprivation impairs judgment, increases stress and anxiety, reduces coping capacity and diminishes energy for treatment participation. Addressing sleep problems supports cognitive function, emotional stability and overall treatment adherence, all factors contributing to successful long-term recovery.
5. What natural strategies help improve sleep during opioid withdrawal?
Natural sleep improvement strategies include maintaining consistent sleep and wake times, creating a cool and dark sleep environment, avoiding caffeine and screens before bed, practicing relaxation techniques like deep breathing or meditation, taking warm baths, engaging in gentle exercise during the day and limiting daytime napping. Combining multiple approaches often produces better results than relying on any single strategy.
Discontinuation of antidepressants is not as easy as some individuals would assume. Sometimes known as antidepressant discontinuation syndrome, cymbalta withdrawal symptoms may manifest when duloxetine is tapered off too slowly or abruptly. These symptoms do not indicate weakness and dependence – actually, it is a physiological response as the brain adapts to the shift in the levels of neurotransmitters.
Knowing what to expect, the length of the symptoms, and knowing how to cope safely with them can reduce the process a lot. Cymbalta withdrawal management with proper tapering and support can go through more easily and safely.
Cymbalta (duloxetine) is a serotonin-norepinephrine reuptake inhibitor (SNRI) that is regularly prescribed to manage depression, anxiety, chronic pain, fibromyalgia, and nerve pain. Its mechanism of action is that it raises the level of serotonin and norepinephrine in the brain-chemicals that aid in the control of mood and perception of pain.
Withdrawal is caused by the fact that the brain gets used to the existence of Cymbalta over time. With a decrease or discontinuation of the medication, neurotransmitter levels abruptly drop and cause duloxetine withdrawal effects. Patients stopping Cymbalta are more likely to experience withdrawal symptoms in case changes are introduced too fast because the half-life of the antidepressant is lower than that of certain other antidepressants.
The symptoms of cymbalta discontinuation may be of different intensity and different lengths. Some experience mild discomfort, while others have more severe effects that interfere with daily functioning.
The most typical stopping cymbalta side effects are:
These are not psychological symptoms but rather physical symptoms and indicators of the process of adjustment of the nervous system, and not the relapse of the initial disorder.
Cymbalta withdrawal is one that is not the same in everyone – however, there are usually symptoms that follow a general pattern depending on the dosage used, time taken, the rate of tapering, and the sensitivity of the nervous system of a person. There is a delay in rebalancing in the brain and body as duloxetine influences both serotonin and norepinephrine, and then there is a time frame, when the drug is decreased or stopped.

The onset of withdrawal symptoms can start in as few as days after changing the dose and increase or decrease, instead of improving straight down the line. Other individuals have noticed short-lived episodes of symptoms and lapses between symptoms, which is a normal aspect of an adaptation of the nervous system. The following table presents the most common stages of Cymbalta withdrawal duration and what one can expect at each stage.
| Withdrawal Phase | Typical Timeframe | Common Symptoms |
| Onset phase | 1 to 3 days after dose reduction | Lightheadedness, brain shocks, vomiting, nervousness, and flu-like symptoms. |
| Acute phase | 4 to 14 days | Maximum severity of symptoms, sleeping disorders, mood swings, and tiredness. |
| Adjustment phase | 2 to 6 weeks | Slow improvement of the symptoms, persistent dizziness, and emotional sensitivity. |
| Resolution phase | 6+ weeks (varies) | The symptoms persist to subside, and the brain chemistry normalizes. |
The withdrawal symptoms usually start between 1-3 days following dose reduction or quitting. The initial symptoms are the most severe ones.
Common symptoms in the early stages are:
The effects may be disturbing, but they are often temporary, provided that they are dealt with.
In certain cases, the Cymbalta withdrawal period exceeds a week. The symptoms can progressively disappear in 2-6 weeks, however, higher doses or prolonged use may extend this period, and a longer period may be possible.
Prolonged symptoms can be:
The improvement is likely to happen gradually, but the constant or deteriorating symptoms must always be communicated to a healthcare provider.
Gradually reducing the dose under medical supervision is the safest way to manage cymbalta tapering symptoms. And the gradual reduction in taper is not a standardized tapering schedule, but it gives time to the nervous system to adapt.
General principles of tapering are:
There are those who demand extremely slow tapers, especially following prolonged use. Patience during this process can significantly reduce withdrawal severity.
Cymbalta withdrawal relief management involves managing symptoms, supporting the nervous system, and reducing stress. Withdrawal symptoms cannot always be eliminated, but in many cases, discomfort may be lessened.
Helpful strategies include:
Healthcare providers in certain situations might have to vary the rate of the tapering or temporarily increase the dosage and continue with a gradual downward adjustment.
Though most individuals cope with withdrawal with an outpatient helping hand, others have serious symptoms that disrupt normal life. It is more prevalent in patients with co-occurring mental disorders or substance abuse histories.
Signs that additional support may be needed include:
Monitoring, alleviation of symptoms, and emotional support can be offered to a person during this vulnerable period with the help of professional care.
Clinicians at Silicon Valley Recovery realize that antidepressant withdrawal may be physically and emotionally troublesome. The personalized, compassionate support is based on evidence-based care. Withdrawal, whether in isolation or with the use of substances, would be very much safer and more comfortable with the assistance of a professional.
You need not experience the effects of Cymbalta withdrawal in solitude, provided that it is affecting your quality of life.
Contact Silicon Valley Recovery for caring help and professional counseling during withdrawal and recovery. Support makes a difference.

The most frequent ones are dizziness, brain zaps, nausea, anxiety, and sleeping problems. These are caused by the process of the brain adapting to the changes in the levels of serotonin and norepinephrine.
The majority of the symptoms are better in 2-6 weeks – however, depending on the dosage, the rate of tapering, and the sensitivity of the particular person. Other individuals have less severe and extended symptoms.
The most effective method is the reduction of the dose gradually under the care of a physician. Tapers are slow, which lowers the degree of withdrawal and enhances comfort.
Quitting Cymbalta would not be advisable because of the aspect of severe withdrawal symptoms. It is always safer with a taper overseeing it.
Symptoms can be relieved with the help of hydration, rest, gradual tapering, the reduction of stress, and medical guidance. The availability of professional support is particularly beneficial in cases of the severity of symptoms.
When one spends the night out, a lot of individuals will find themselves seeking ways to make themselves sober within a short time in the hope that there is a solution within a bottle that will cure the effects of alcohol. It may be to feel better or to think clearly or to have a feeling of control again, the need to be as quick as possible to sobriety is understandable, although it is misconceived.
The fact is, alcohol has an influence on the body that cannot be turned immediately back. Although there are measures that you can undertake to take the edge off and make yourself more comfortable and supportive of the body in the process of handling the alcohol, there are indeed no shortcuts to sobriety. The point to start is to understand the way alcohol functions in the body and make safer choices for long-term health.
Contrary to common knowledge, there is no sure way to get quickly sober. Alcohol has to be processed by the liver, and this is time-consuming irrespective of the nature of the remedies administered.
The quick sobriety tips tend to emphasize the concealment of the symptoms instead of decreasing the level of actual intoxication. Some of the strategies can make you feel more focused or less nauseated, but they do not make much reduction in blood alcohol content (BAC).
This difference will be vital, particularly where there are safety or legal implications involved, e.g., driving.
The metabolism of alcohol is a biological process that cannot be hurried. When alcohol is taken into the body, it is absorbed through the stomach and small intestine into the bloodstream, and then it is processed by the liver, which is the main place of processing. This has a gradual process, whether it is the so-called sobering tricks that are proposed frequently.
The average metabolism rate of an average person is approximately one standard drink per hour, but this may be fluctuated by certain factors. The concept of what affects the metabolism of alcohol can be used to explain the reason why sobriety is a gradual process and why the results vary among individuals. The following table indicates the major determinants that influence the rate at which alcohol is broken down in the body.
| Factor | How It Affects Alcohol Metabolism |
| Body size | Higher body mass might dilute alcohol to some extent, but the rate of metabolism is still low. |
| Biological sex | The variation in enzymes and body structure may influence the processing speed. |
| Liver health | When the liver is healthy, it is more effective in the metabolism of alcohol. |
| Genetics | The enzyme changes have an impact on the breakdown of alcohol. |
| Amount consumed | Larger amounts take longer to process. |
| Drinking speed | The quick intake leads to intoxication that is followed by rapid metabolism lagging behind. |
There are numerous individuals who seek a means by which to get out of intoxication, however, it is not that fast that the liver can handle this. Nothing can suppress this process, any supplement, beverage, or activity.

Coffee, exercise, cold showers, and similar methods may make one feel more alert, but they do not eliminate alcohol in the blood. That is why one should not use quick sobriety tips.
Sober-up remedies have numerous myths that surround them. It is equally important to know what does not work as it is to know what works.
Common myths include:
Although such measures can alter your mood, they do not significantly affect BAC.
Though you cannot sober up immediately, there are realistic measures that can make you feel better as your body is processing alcohol. It is necessary to keep in mind that time is the most important factor in alcohol detox before enumerating these steps.
Other useful activities when waiting to sober up include:
Such measures facilitate comfort and security but cannot be confused with immediate sobriety.
Alcohol is also dehydrating, and it may interfere with blood sugar levels, which also causes fatigue, nausea, and headaches. Even when alcoholic recovery is not accelerating, hydration and nutrition help alleviate the symptoms of suffering, even though they do not accelerate the metabolic rate.
It is a good idea to have a grasp of what they are achieving prior to noting the strategies, they are not aiming at the reduction of intoxication but rather the relief of symptoms.
To hydrate and nourish, they are:
It is not unusual to wonder how to sober up after drinking. Nevertheless, the constant necessity of finding fast sobriety solutions can be a sign of a more serious problem with alcohol consumption.
Red flags that can be used include:
With time, excessive drinking may limit the working capacity of the liver, tolerance, and physical or psychological reliance may develop.
When alcohol consumption has become hard to manage or recovery seems too daunting, professional assistance can be of significance. Care at Silicon Valley Recovery is caring, confidential, and individualized. It is not just a matter of willpower to recover, but rather it is a matter of having the right instruments and support.
When you have to go on a regular hunt to find out how to sober up fast, maybe it is time to take a look at some healthier and sustainable options.
Contact Silicon Valley Recovery to find out how professional assistance can be used to get yourself under control and get on the path towards long-term recovery.

The average body is capable of processing one standard drink an hour. The level of sobriety is dependent on the quantity of alcohol taken and personal metabolic influences.
Coffee does not boost alcohol metabolism. It will not change your BAC but may make you more alert.
Taking cold showers does not reduce the intoxication of alcohol in the blood, but it will make a person more alert. They can also be dangerous in case of dizziness.
Toast, fruit, and soup are light foods that can be used to normalize sugar levels and overcome nausea. Eating does not eliminate alcohol from the blood system, but it can make one feel better.
In cases where daily commitments are affected by frequent intoxication or need frequent recovery measures, it can be an indicator of alcohol dependency. Professional assistance may stop the long-term injuries.
When facing the challenge of overcoming opioid addiction, many people wonder whether certain medications can alleviate their withdrawal symptoms. One of the drugs that is often mentioned in this context is gabapentin. Does gabapentin help with opioid withdrawal, and should you include it in your recovery journey?
In our article, we will explore the benefits of using gabapentin for opioid withdrawal and examine the effectiveness of this medication. We will also look into the side effects of gabapentin and offer alternative solutions to address opioid withdrawal symptoms.
![]()
Gabapentin is a medication primarily designed to treat epilepsy and manage seizures. The drug can also be prescribed to address chronic pain and relieve the symptoms of restless legs syndrome. Gabapentin is an anticonvulsant—it affects the nerves and chemicals in the human body responsible for seizures and pain.
In recent years, the off-label use of gabapentin has expanded to include anxiety reduction and insomnia treatment. Thanks to the drug’s ability to decrease agitation and promote calmness, gabapentin has become a useful tool in assisting patients undergoing various addiction treatments, including alcohol dependency and marijuana addiction.
Opioids are powerful painkillers that target the brain’s opioid receptors and increase the production of endorphins—chemicals responsible for alleviating pain and enhancing pleasure. Unfortunately, while effective, opioids are highly addictive—even a short prescription from your healthcare provider can lead to dependency.
Once a person becomes addicted to opioids, they may experience a myriad of unpleasant symptoms when they attempt to cut down on their drug consumption or quit taking opioids altogether. These symptoms are both physical (muscle pain, headaches, sweating, nausea) and psychological (anxiety, irritability, insomnia, depression).
There are several benefits to using gabapentin during opioid withdrawal:
Gabapentin can be of great help during opioid withdrawal. Several studies have confirmed the efficacy of this medication—patients who were given gabapentin during their recovery reported that it helped them cope with the withdrawal symptoms and reduced their pain.
Like any medication, gabapentin may have side effects:
Before you start taking gabapentin for opioid withdrawal, you should be aware of the side effects associated with this drug. While gabapentin is usually well-tolerated by patients, some individuals may have an adverse reaction to the medication—in this case, the doctor may adjust the dosage or suggest you stop taking gabapentin.
![]()
If you are looking for medications similar to gabapentin or want to have several options to choose from before you start your recovery, consider these alternatives to gabapentin for opioid withdrawal:
While gabapentin is a viable option for opioid withdrawal, you may want to consider other medications that can help you cope with the symptoms of this challenge. Make sure to talk to your physician—a trained medical professional will be able to diagnose your issue and prescribe the best medication for your unique circumstances.
Gabapentin is a drug intended to prevent and treat seizures—it was first approved for medical use in 1993 for epilepsy treatment.
Opioid withdrawal may lead to various physical and mental health issues—patients struggle with muscle aches, anxiety, headaches, insomnia, nausea, and depression.
Gabapentin is capable of reducing the symptoms of opioid withdrawal—this medication lowers anxiety, improves sleep, and manages pain.
The most common side effects of gabapentin are dizziness, drowsiness, and fatigue. In rare cases, patients may suffer from breathing difficulties and suicidal thoughts.
There are several drugs similar to gabapentin you may want to use for opioid withdrawal—ask your doctor about methadone, buprenorphine, clonidine, and naloxone.
Incorporating gabapentin into your treatment plan can be a smart choice—this medication has been proven to be effective when it comes to addressing opioid withdrawal. Gabapentin will reduce the symptoms of withdrawal and make your recovery journey easier.
If you are looking for a personalized approach to opioid addiction treatment, reach out to Silicon Valley Recovery. Our team will support you every step of the way—we will help you select the best medication for your unique case and provide you with the tools you need to conquer your addiction. Contact us today to find out how we can assist you.
When you or a loved one is treated by a healthcare provider, you are likely to receive a prescription for one or several medications. It is important to remember that all drugs have a specific shelf life and will eventually expire. Consuming expired pills can be dangerous to your health.
If you are wondering how long prescription medicine lasts, our blog will be able to help you. Below you will find the definition of the shelf life of prescription drugs, a few factors that affect the longevity of medications, and useful tips on the proper storage of your medicine.
![]()
Prescription medication shelf life can be defined as the period of time calculated from the date the medicine was manufactured during which the drug is safe to consume, and it remains effective to treat the symptoms it was prescribed for. After this time passes, the medication is considered expired—it may lose its potency and, in some cases, become dangerous for the patient.
There is no universal shelf life for prescription drugs—on average, medications are safe to use for up to two or three years. You should check the packaging of the medicine to see its expiration date and pay attention to the storage instructions, especially if you are planning to keep the drug at home for a long time.
The formulation of the medicine plays a huge role when it comes to the duration of its shelf life. Here are a few types of medicine and their average shelf life:
Several elements may influence the shelf life of prescription drugs:
![]()
Follow these tips to make sure your prescription drugs remain safe and effective:
It is advised to avoid taking medicine that has expired. While in many cases the drug will not harm you, it may not have the desired effect—the medicine loses its potency after its shelf life is over. This may be crucial for your treatment and recovery—for instance, if you fail to take effective pain medication after the surgery, your healing process may be delayed.
In rare cases, expired medicine will negatively affect your health. If you or your family member has taken drugs that have passed their expiration date, and you have noticed unusual side effects—dizziness, nausea, or abdominal pain—reach out to your doctor.
On average, prescription medicines last for two or three years. The shelf life of the drug will depend on its formulation and storage conditions.
Several factors affect the longevity of the medicine—its type (tablets, capsules, liquid, injectables, etc.) and storage (temperature, light exposure, humidity of the room, and type of container).
You should not consume drugs that have expired—they may be ineffective for your treatment and, in some cases, harmful to your health.
Check the packaging of the drug to learn its expiration date—manufacturers usually calculate the shelf life of the medicine and list the date on the label.
To increase the longevity of your medicine, store it in a dry, dark, and cool place. There may be special storage instructions on the label of the drug—follow them to preserve the medicine.
Understanding how long prescription drugs last and when it is time to dispose of expired medicine is crucial for your health. Different types of medicines have varying shelf lives—if you are unsure whether a particular drug is safe to consume, it is best to consult with a healthcare professional.
Our team is here to help you—get in touch with Silicon Valley Recovery to receive personalized advice regarding prescription medications and make sure you never put your health at risk.
Adderall is a widely recognized medication primarily prescribed for Attention Deficit Hyperactivity Disorder (ADHD) and narcolepsy. It is a central nervous system stimulant that can help increase attention, focus, and impulse control for those diagnosed with ADHD. However, understanding the strongest Adderall prescription, its potential side effects, and the proper way to use it is crucial for patients and caregivers.
In this guide, we will delve into the uses of Adderall, the available dosage options, potential risks associated with its consumption, and alternative treatments for ADHD. If you or your loved one is considering starting Adderall, consult your healthcare provider to determine if this medication suits your needs.
![]()
Adderall is a prescription medication consisting of four amphetamine salts: amphetamine aspartate, amphetamine sulfate, dextroamphetamine saccharate, and dextroamphetamine sulfate. This combination of ingredients makes Adderall a potent stimulant designed to affect brain chemicals and neurotransmitters.
Adderall is approved by the Food and Drug Administration (FDA) to treat the following conditions:
In some cases, Adderall is also used off-label to treat depression and help patients struggling with major depressive disorder (MDD) achieve better results when combined with antidepressants. Nonetheless, the efficacy of Adderall for depression remains unproven.
Adderall comes in two formulations: instant release (IR) and extended release (XR). Patients can choose to take Adderall orally in the form of tablets or capsules. Your healthcare provider will help you select the optimal Adderall dosage based on your age, weight, medical history, and personal needs.
Adderall IR Dosages
Adderall IR tablets are available in the following strengths:
Adderall IR is usually taken two to three times a day, with the first dose administered in the morning. You can expect Adderall IR to kick in within an hour and last four to six hours.
Adderall XR Dosages
Adderall XR capsules are available in the following strengths:
Adderall XR is designed to be taken once a day since this formulation lasts between 12 and 24 hours. While Adderall XR takes longer to start working (from 30 minutes to 2 hours), its prolonged benefits make it a popular choice among patients.
![]()
Like any medication, Adderall may cause certain side effects, from mild to severe. Make sure you are aware of the potential consequences of taking Adderall before you start your treatment.
Common Side Effects of Adderall
Here are a few of the most common side effects of Adderall:
These side effects are typically minor and go away on their own after a few days of treatment. If these side effects persist or cause you significant discomfort, talk to your doctor about adjusting your dosage or switching to a different medication.
Severe Side Effects of Adderall
In rare cases, taking Adderall can lead to more serious side effects, such as:
If you experience any of these side effects after taking Adderall, seek medical help immediately.
Adderall is primarily prescribed to children and adults with ADHD or narcolepsy. There is no single age group that can benefit from taking Adderall—anyone from a six-year-old child to a senior can be prescribed this medication.
However, Adderall is not suitable for people with certain pre-existing conditions. Make sure you do not fall under the following categories before you take Adderall:
If Adderall is not a good fit for you, there are plenty of alternative medications you can try to manage ADHD.
Medication
Here are a few ADHD medications you can try instead of Adderall:
Therapy
In addition to medication, consider enrolling in therapy to address ADHD. Working with a licensed therapist can help you understand the root of the problem and develop healthy coping mechanisms to reduce the symptoms of ADHD without drugs.
1. What is the strongest Adderall prescription available?
The highest FDA-approved dosage of Adderall is 30 mg for both immediate-release (IR) and extended-release (XR) formulations. However, higher doses increase the risk of dependency, misuse, and adverse side effects, especially when taken without close medical supervision.
2. Can Adderall be addictive?
Yes. Adderall is a stimulant and a Schedule II controlled substance, meaning it carries a high potential for misuse and addiction. Taking higher doses than prescribed or using Adderall without a prescription significantly increases the risk of substance use disorder.
3. What are signs of Adderall misuse or dependence?
Common signs include needing higher doses to feel the same effect, taking Adderall for reasons other than prescribed, insomnia, anxiety, irritability, appetite loss, and difficulty functioning without the drug. In severe cases, misuse can lead to paranoia, psychosis, or cardiovascular issues.
4. Is it safe to stop taking Adderall suddenly?
Stopping Adderall abruptly—especially after long-term or high-dose use—can cause withdrawal symptoms such as fatigue, depression, mood swings, and intense cravings. It’s important to seek medical guidance before discontinuing use.
5. What are alternatives to Adderall for ADHD or stimulant misuse recovery?
Treatment options may include non-stimulant ADHD medications, behavioral therapy, cognitive behavioral therapy (CBT), lifestyle changes, and structured addiction treatment programs that address both mental health and substance use concerns.
If Adderall use has become difficult to control or is affecting your mental health, relationships, or daily life, help is available. The experienced team at Silicon Valley Recovery Center provides comprehensive, evidence-based treatment for stimulant misuse, co-occurring mental health conditions, and substance use disorders. Reach out today to schedule a confidential assessment and take the first step toward recovery, stability, and long-term wellness.
Adderall is a readily available stimulant medication, as well, which is used to treat attention-deficit hyperactivity disorder (ADHD) and, less commonly, narcolepsy. Despite not being a bad drug when used as prescribed, the majority of people will pose such questions as how long does Adderall stay in your system, especially in terms of drug screening, health-related or the fear of abuse.
The pharmacokinetics of Adderall take more than one number. Depending on the dosage, use frequency, metabolism, and the type of drug test, detection time may be different. This guide disaggregates the mechanisms of Adderall, the duration it can be detected, and the significance of this information beyond employment.
Adderall is a combination of amphetamine salts, which are central nervous system stimulants. It works by increasing levels of dopamine and norepinephrine in the brain, which is employed in increasing concentration, attention, and impulse control.
Once ingested, Adderall is absorbed through the gastrointestinal system and processed by the liver, the majority of the time. The blood then transports it all through and is disposed of mostly through urine.
There are two major formulations:
The formulation is very crucial in the duration of action and binding of Adderall in the body.
The half-life of a particular drug is the period in which half of the drug is eliminated from the body. According to research on clinical pharmacology, Adderall has an average half-life of 9 -14 hours, depending on individual factors and formulation. It is documented in studies conducted in Clinical Pharmacokinetics that, on average of about 5 half-lives is needed to get the drug virtually eliminated.
No standard detection window of Adderall exists. The time of detection may vary across many factors, depending on the individual and the usage.
The most important things that determine the duration for Adderall to remain in your body include:
Chronic/high-dose administration can result in a delay in detection as compared to infrequent therapeutic use.

A urine test is the most typical method of determining Adderall and other amphetamines. The urine drug tests, which are generic, are not designed to detect specifically Adderall but amphetamines.
According to the research done by the Substance Abuse and Mental Health Services Administration (SAMHSA), Adderall is likely to be detected in urine 2 to 4 days after use.
It is worth comparing the detection windows before analyzing other test types.
| Test Type | Typical Detection Time |
| Urine test | 2 to 4 days |
| Blood test | 12 to 24 hours |
| Saliva test | 1 to 2 days |
| Hair test | Up to 90 days |
A blood test will identify Adderall significantly sooner since amphetamines are eliminated from the bloodstream comparatively fast. The majority of the studies reveal that it can be detected within 12 to 24 hours of the final dose.
A saliva test also has a slightly wider detection window, with an average of 24 to 48 hours for Adderall. Less prevalent, saliva testing can be applied in road localized examination or brief observation.
These are usually more effective in detecting recent use and not previous exposure.
A hair test is not like a urine test, a blood test, or a saliva test. It does not detect the presence of active drugs, but finds the drug metabolites that become entrenched in the hair shaft as the hair grows.
Based on research, Adderall can be detected in hair for up to 90 days. Hair tests, however, are less popular in routine screening, and they are expensive.
It is also worth mentioning that hair tests cannot identify the recent use or impairment, but only the prior exposure.
Although drug testing is commonly linked with jobs, the outcomes may have wider consequences. Legal, or recovery-related, in the field of healthcare, test results can play a role in the choices to be made in the course of treatment, compliance mandates, or safety strategies.
To those who are recovering, either prescribed or abused stimulants can make mental health, sleeping habits, and emotional control difficult. A timeline of detection can help people make informed choices and prevent unintended consequences.
Addiction medicine studies indicate that stimulant abuse has the potential to augment addiction vulnerability, stress, high blood pressure, and sleep disturbance, particularly when the substance is used beyond the scheduled prescriptions.
How long does Adderall stay in your system? is the question that can come up, as well as more serious reasons, which involve misuse, addiction, or even a lack of knowledge of using the medication. Support at Silicon Valley Recovery is more than the test results. At either the prescriptive or unregulated stage of Adderall use, the assistance of a professional could potentially allow safeguarding of the physical health and long-term well-being.
In case of fears of using Adderall, taking a drug test, or being addicted to the stimulants, you can get help.
Contact Silicon Valley Recovery today to get confidential help and professional advice.

The average time that Adderall is visible in urine is 2 to 4 days after administration. Cases of frequent use, higher dosage, or slow metabolism may require a long time to be detected.
Adderall has an average half-life of between 9 -14 hours, depending on the formulation and the metabolism of a particular person. This implies that the drug may take a few days before eliminated completely.
Yes, it is possible to test Adderall in a hair follicle test up to 90 days after usage. Hair testing is not as popular, and it is normally applied in cases of long-term or former exposure, not in cases of use.
The detectability of the drug depends on the dose, frequency, metabolic rate, hydration, and urine pH. The rate at which the body is able to process amphetamines may also be affected by liver functioning and general well-being.
The adderall typically stays in the blood between 12 and 24 hours after the final administration. Blood tests are most useful in detecting very recent use as opposed to a past exposure.
Meloxicam is a popular nonsteroidal anti-inflammatory drug (NSAID) that is commonly prescribed to patients diagnosed with rheumatoid arthritis and osteoarthritis – it helps reduce the pain and inflammation caused by these conditions which significantly improves the quality of the patient’s life. It is also useful for individuals who suffer from stiffness and swelling in their joints.
You should be prepared to experience meloxicam withdrawal symptoms if you developed a dependence on this medication or were taking high doses of this drug especially if you misused meloxicam against the instructions of your healthcare provider. The pain and inflammation return once you stop using meloxicam, and patients often inform their healthcare providers about the psychological dependence they developed on meloxicam – they become mentally reliant on this drug to manage their pain and feel stressed because they worry their symptoms may return or worsen.
Even though meloxicam withdrawal is not as severe as some would expect considering the effectiveness of this medication, it will still be difficult to cope with physical symptoms which include tachycardia, gastrointestinal issues, back pain, shortness of breath, and flu-like symptoms. When you quit meloxicam abruptly, you may experience diarrhea and even harm your kidneys or liver which is why people with chronic health problems need to be mindful of potential withdrawal.
There may be complications that affect your mental health – many patients become restless, agitated, and even depressed once meloxicam is no longer in their systems. When you are taking other prescription drugs alongside meloxicam, they may affect your body differently now that this anti-inflammatory medication is not in the picture.
While meloxicam is quite similar to alternative prescription medications – the mechanism of action, the therapeutic use, and the adverse effects are largely the same – there is a difference between how the body of the patient reacts to meloxicam withdrawal in comparison to the withdrawal from other addictive substances such as opioids or alcohol:
| Key Difference | Description |
| Lack of Psychoactive Effects | Meloxicam will not alter your brain chemistry because it does not penetrate the blood-brain barrier – there are no typical withdrawal symptoms that occur where there is a different type of addiction. |
| Severity of Symptoms | In general, the symptoms are rather mild – individuals who discontinue meloxicam complain about digestive issues, physical fatigue, and headaches. |
| Rebound Effect | Instead of experiencing physical discomfort, an individual will struggle with inflammation and pain that meloxicam was helping them with. |
| Lack of Physical Dependence | Since meloxicam is not an addictive substance that induces euphoria and causes rapid tolerance, the gradual tapering off goes relatively smoothly. |
The timeline of meloxicam withdrawal contains three phases:

Here are a few tips for someone who stops using meloxicam:
It can be hard to predict the impact of meloxicam on the person’s health as well as the duration of withdrawal – there are several contributing factors at play here. Your age, kidney function, liver function, metabolic rate, the presence of physical conditions, the simultaneous use of other medications, the use of alcohol, and the long-term use of meloxicam will inevitably change the way your body reacts to the absence of this substance. On average, the withdrawal of meloxicam lasts for about ten to fourteen days – up to one month in the most severe cases.
You can cope with the most acute symptoms of meloxicam withdrawal by relying on the following therapeutic approaches:
| Advice | Description |
| Taper off Meloxicam | You should only do so under the supervision of a detox specialist – they will tell you how to calculate the right dose and cleanse your body of the traces of meloxicam step-by-step. |
| Ask Your Loved Ones for Help | Find out which family member or friend you can trust with your problems and ask them to keep you accountable as you are staying away from meloxicam – this is particularly important during the first few days of withdrawal. |
| Attend Counseling Sessions | Talk to a therapist about the reasons for your meloxicam addiction, come up with a recovery plan you will stick to under their guidance, and master coping mechanisms that will distract you when withdrawal manifestations get too severe. |
| Explore Alternative Therapies | There are numerous holistic interventions you can try to see what resonates with you, reduces your anxiety, and helps you combat cravings – meditation, yoga, breathing exercises, and art therapy are among the most common mindfulness practices you can incorporate into your daily routine. |
| Prioritize Your Physical Wellness | Even if your symptoms are more of an emotional nature, you should not disregard your physical well-being during the withdrawal and detox – light exercise will boost your energy levels while proper nutrition will give you strength to keep up with a tapering schedule or a comprehensive detox program. |
Whether you have been dealing with side effects of meloxicam that have been detrimental to your psyche, tried to quit this drug on your own, or worry about the complicated process of withdrawal, undergoing detox under the supervision of medical professionals can be the solution you are looking for. Our team is ready to help individuals who want to combat the symptoms of meloxicam withdrawal and prevent health complications in the long run.
Reach out to Silicon Valley Recovery now – start the journey of physical and mental transformation and secure a healthy future for yourself.

Physical and emotional fatigue, mood fluctuations, digestive issues, and the return of pain and inflammation the patient was coping with using meloxicam are the most common signs of withdrawal.
The symptoms will bother you during the first days after meloxicam discontinuation, peak after a week, and subside over the next week completely – in most instances, without any lasting damage to your body and mind.
Since meloxicam will be fully eliminated from your system in three to five days, the withdrawal symptoms should not last much longer especially if you are supervised by a doctor and take care of your overall health at that time.
Low energy, depression, and stomach issues are arguably the most difficult things to manage but they will not interfere with your day-to-day activities for too long.
Seek medical assistance if the pain and inflammation are too difficult to bear without additional medication or the symptoms such as diarrhea or sore throat do not subside within a couple of weeks.
Eszopiclone (the brand name of the medication is Lunesta) refers to a nonbenzodiazepine drug prescribed to patients who suffer from insomnia. It is not a secret that sleep is vital for your overall health – it helps with physical repair, emotional regulation, and cognitive function, so when you struggle to fall asleep or stay asleep to get the restorative rest you need, it will affect you on a daily basis. Lunesta will slow down your brain activity and fix the chemical imbalance that forces you to stay awake for a long time.
Medications like Lunesta can certainly be very beneficial to a patient but they have their risks – it is very easy to abuse a drug of this kind and become dependent on it. Patients may build up a tolerance to the effects of Lunesta and take larger doses of it to fall asleep without scheduling a consultation with their doctors. Still, simply quitting Lunesta is not an easy solution either – the withdrawal that comes after will impair your functioning.
Sedative-hypnotic medications – usually referred to as “sedatives” – are among the most commonly prescribed drugs. Sleep disorders such as insomnia affect both children and adults which is why medication management is often necessary to help people who are unable to fall asleep on their own. Lunesta can be quite effective when it comes to the treatment of insomnia – you fall asleep at a faster rate, sleep enough to rest and restore your strength, and prevent random middle-of-the-night awakenings that interfere with your daily routine.
As soon as you stop taking Lunesta, you may experience anxiety and feel unable to calm down before you go to bed – this kind of emotional dysregulation results in insomnia, which means the withdrawal of Lunesta is fueled by your poor emotional state on top of physical dependence on the drug. Mental and physical fatigue are also among the first symptoms, considering it will be hard to get a full night of sleep once you no longer take a sedative.
The most common Lunesta withdrawal symptoms are restlessness, nervousness, fatigue, nausea, vomiting, and anxiety. In the most severe cases, the person will exhibit uncharacteristic aggression and suffer from seizures – the latter symptom definitely warrants medical intervention.

Lunesta withdrawal will take a toll on your body and mind simultaneously – let us look at the key differences between psychological and physical signs of withdrawal:
| Feature | Physical | Psychological |
| Symptoms | Gastrointestinal issues, excessive sweating, and physical exhaustion. | Anxiety, restlessness, agitation, aggressiveness, and emotional fatigue. |
| Duration | Peak at the end of the first week without Lunesta and subside by the end of the first month. | May affect the individual for months especially if the problem is disregarded. |
| Treatment Options | Medically supervised detox is the best option for people with acute symptoms. | Cognitive and behavioral therapy modalities and support groups will help you overcome psychological dependence on Lunesta. |
While the process of withdrawal looks different for everyone, there are usually three phases:
It is hard to predict how long withdrawal of Lunesta will last in every particular case – it depends on the physical well-being of every person who has been using this medication and, in some instances, the longevity of their addiction to the drug. However, most individuals are able to cope with the symptoms within two or three weeks. If your addiction is severe, the symptoms will not fade away for a few months but you can minimize the adverse effects by undergoing detoxification and following the guidelines of medical providers.
Even though Lunesta withdrawal is not as severe as the withdrawal many patients go through after they stop using more powerful drugs and mind-altering substances, it is still difficult to quit this medication – things will inevitably change, especially if your sleep routine has not yet been restored. Nevertheless, there are therapeutic approaches that individuals with sleep disturbances can resonate with to overcome their insomnia and combat sedative dependence.

| Strategy | Description |
| Sign up for a Detoxification Program | Undergoing detox with the assistance of medical professionals who will tell you how to minimize the risks of Lunesta withdrawal on your health is arguably the most effective option for most individuals. |
| Attend Counseling Sessions | Whether you resolve your sleep problems in individual therapy or meet with like-minded patients in group therapy when the same issue triggers sleep disturbances for all of you, therapy can be a source of validation and support. |
| Work on Your Physical Wellness | Sleep issues can be very detrimental for your body which is why optimizing your nutritional intake, exercising, playing sports, and avoiding alcohol and caffeine will do wonders for your health. |
| Find Solace in Mindfulness | Unconventional methods you can practice on your own such as meditation therapy, journaling, yoga, or breathing exercises will be an outlet for emotions related to complicated withdrawal. |
Whether you have tried to taper off Lunesta on your own and could not or you want to undergo a supervised detox from this prescription sedative, talking to a specialist who knows how to cope with the symptoms of withdrawal safely is the best solution. Our clinic welcomes all individuals in need of guidance and support when they try to discontinue prescription medication like Lunesta.
Reach out to Silicon Valley Recovery today – together, we can handle all the physical and psychological challenges you have to face during the Lunesta withdrawal.
Lunesta withdrawal will affect you psychologically and physically – you will experience the symptoms of an anxiety disorder, feel emotionally fatigued, suffer from digestive issues, suffer from excessive perspiration, and feel unable to fall asleep when you need to rest.
The timeline of the withdrawal varies from person to person but usually the symptoms start during the first one or two days, get worse by the end of the week, and slowly disappear over the course of two weeks – in rare cases, over the course of the month.
The duration of Lunesta withdrawal does not exceed seven or ten days – only if your physical health is hampered by additional conditions or you are taking prescription medications that have adverse effects on your body and mind, will it take you up to a month to overcome the symptoms.
At the very minimum, it will be difficult to fall asleep without any medication at first. This will cause you to feel restless and anxious, result in fatigue, and lead to headaches and digestive problems especially if your health is not at its best right now.
If you have mental and physical health conditions whose symptoms get worse because of your insomnia, do not hesitate to see a doctor. Additionally, if Lunesta withdrawal causes seizures or vomiting you cannot control for a day or two, make sure you get adequate medical help.
Hydromorphone (the brand name of this drug is Dilaudid) is a popular opioid that is typically prescribed to patients who struggle with severe pain. It alleviates the symptoms of the person when similar painkillers are futile – there are capsules and tablets that relieve the pain when opioid treatment is the only reasonable solution.
Despite its effectiveness, Dilaudid is an addictive substance – when someone uses it for a long time, they may build up a tolerance to the effects of this drug and depend on it both physically and psychologically. The dependence becomes a problem when the person misuses Dilaudid or stops using it abruptly without talking to their healthcare provider first – this may happen if you do not have access to the medication, and the symptoms of the withdrawal may seriously undermine your wellness.
Only a medical professional can confirm that the symptoms you are currently dealing with are a direct consequence of Dilaudid discontinuation. Still, it is important that you know you are going through a withdrawal and it is not a side effect of a different medication you were prescribed. Besides, certain discomfort is normal – the withdrawal rarely goes smoothly even if you are physically strong. Only when the symptoms become overwhelming and interfere with your day-to-day obligations, should you seek medical intervention or mental health guidance.
Dilaudid cessation takes a toll on your body – typically, it starts within the first twenty-four hours after the last dose is taken. The cravings begin right away – they are worsened by excessive perspiration, rapid breathing, muscle pain, an inability to fall asleep, and yawning that quickly becomes a major nuisance. The physical discomfort makes it hard to concentrate and make decisions – your physical and cognitive wellness are closely connected which is why working or socializing during the first days of withdrawal of Dilaudid becomes quite a challenge.
Sometimes, Dilaudid affects your emotional state more than it harms your physical health. Patients who discontinue this medication confirm that they feel restless and nervous, there is a sense of fear and dread they cannot attribute to any other factors, and their mood fluctuates – one moment they are agitated, and the next they go through a depressive episode.
It only takes a few hours for a person to feel how complicated the process of Dilaudid withdrawal can be. While your brain and body are readjusting to the absence of this drug in your system, it is easy to develop depression, anxiety, and insomnia as well as feel the rebound pain that is no longer controlled by the medication. Many people have flu-like symptoms such as fever, suffer from random muscle spasms, and lose their appetite which may lead to a temporary weight loss.
| Phase | Description |
| Early Signs | After the dose of Dilaudid is reduced or you stop using it completely, you will feel the first symptoms – restlessness, muscle pain, and stomach cramps. |
| Peak Signs | The manifestations of withdrawal are at their peak one to three days after the last dose – some people report gastrointestinal issues, irritability, and dilated pupils especially if their health has been undermined by other problems. |
| Late-Stage Signs | By the end of the first week, the symptoms are supposed to subside – talk to a doctor if you experience severe symptoms that impair your daily functioning for more than ten days. |
There are certain factors that change the way the withdrawal of Dilaudid occurs – the age of the patient, their metabolic rate, the frequency of Dilaudid use, and the dose of the medication their body has been accustomed to will play a role here. Nevertheless, Dilaudid withdrawal should not affect your physical or psychological health for more than a week.

No matter how complicated the adverse effects of Dilaudid withdrawal may be, it is possible to overcome them and prevent serious health risks as long as you are willing to work with physical and mental health professionals who specialize in detox procedures and can come up with a customized plan for treatment in your case.
Let us take a look at the most common methods to handle the signs and symptoms of Dilaudid withdrawal:
| Therapeutic Approach | Description |
| Medication-Assisted Treatment | There are different drugs that will help with the most acute symptoms of withdrawal – most healthcare providers prescribe Suboxone or methadone after examining the physical health of the individual. |
| Cognitive Behavioral Therapy (CBT) | A patient gets to challenge their negative thoughts and change their mindset opting for healthier coping mechanisms during a difficult time. |
| Holistic Techniques | You can enhance the effectiveness of conventional methods of treatment with practices that have also been tested by time – try meditation, yoga, acupuncture, aromatherapy, and breathing exercises. |
| Focus on Nutrition | Nutrition and hydration are often underestimated by individuals going through a withdrawal but a balanced diet will allow you to improve liver and kidney function so that the toxins are flushed out quicker. |
Whether you have been struggling with Dilaudid dependence for a while or you suspect you might be addicted to this opioid and worry about your physical and mental well-being, do not hesitate to schedule a consultation with a mental health specialist. Our facility can help you take a step towards a healthier life where you can feel in control – your future does not have to be defined by a prescription medication that causes you harm.
Get in touch with Silicon Valley Recovery today – together, we will figure out how to tackle Dilaudid withdrawal and detoxification with minimal harm to your body and mind.

Anxiety, agitation, an inability to fall asleep, intense cravings, sweating, and mood shifts indicate that the person’s body is trying to adjust when the Dilaudid is missing from their system.
Even though Dilaudid withdrawal can be rather challenging, it will not affect you for more than a week. The symptoms begin within hours after the last dose, peak after three days, and subside step-by-step after about seven days.
The duration of Dilaudid withdrawal does not exceed a week – if there are depressive episodes, cognitive issues, or digestive problems more than ten days after you stopped using this medication, go to a doctor without delay.
While physical symptoms such as teary eyes or joint pain are hard to handle, psychological problems are arguably the worst – you will experience cravings, struggle to concentrate on important tasks, and feel anxious and irritated for no valid reason.
In rare cases, Dilaudid withdrawal may cause auditory and visual hallucinations, crippling anxiety, and insomnia that does not let go for days on end – it is better to be safe than sorry and schedule a consultation with your healthcare provider when that happens.
Dependency on benzodiazepines may be a lonely experience, yet diazepam withdrawal is something that can be comprehended and dealt with. Diazepam, which is also referred to as Valium, is a drug that interferes with the nervous system by calming the brain, and therefore quitting it can be as overwhelming after long-term use.
Individuals undergoing diazepam withdrawal symptoms usually fear that something has happened to them when, in the real sense, what happens is that the brain is reacting after being long-term chemically suppressed. Through the support given and medical advice, recovery can be safe and achievable.
Long-term use alters the brain receptor reaction to stress and relaxation. The more time one is on diazepam, the more they get used to it. Once the drug is stopped, the nervous system becomes unable to self-regulate, and this leads to the signs of diazepam withdrawal that most individuals face. This explains why medical tapering is safer than abrupt cessation.
Depending on the duration and amount of drug use, the signs of diazepam withdrawal may start in hours or days after the last dose. These are the signs of the body’s alarm system that has been turned off for too long.
The initial symptoms are most often restlessness, thoughts of restlessness, nausea, sweating, and mood swings. The withdrawal can lead to the worsening of the symptoms, especially in cases where the medication was suddenly discontinued.
To obtain better and medically investigated information about the benzodiazepine withdrawal symptoms and schedules, you may resort to such resources as Healthline. These sources describe the process of withdrawal and what to expect during the process as your body adapts.
These diazepam withdrawal symptoms can be mild or severe, depending on dosage, timing, and overall health.

| Phase | What Happens |
| 6-24 hours | Restlessness, anxiety, weak tremors, and insomnia. |
| Days 2-7 | Maximum symptoms such as panic, nausea, and muscle pain. |
| Weeks 2-4 | Physical symptoms are relieved; emotional symptoms persist. |
| 1-6 months | The potential of persistent anxiety, fatigue, and mood swings. |
The diazepam withdrawal schedule is slower than that of short-acting benzodiazepines since diazepam remains longer in the body. But it also implies that the symptoms may be extended in case they are not treated in a corresponding way.
The most frequent one is, How long does diazepam withdrawal last, as people have to be assured that they will not experience the pain long-term. The acute withdrawal lasts between two and four weeks, though some of the symptoms may occur even after the acute withdrawal. Others might have anxiety, depressed mood, or sleep disorders, which can take months before they are resolved.
The duration of withdrawal of diazepam is affected by several factors. They are the dosage, length of use, abrupt cessation of use, age, liver functioning, and mental health history. A taper monitored by a physician may greatly reduce and ease the withdrawal symptoms.
Others experience post-acute withdrawal syndrome, or PAWS. It means that the lingering effects of diazepam withdrawal, such as fatigue, anxiety, and mental fog, could last weeks or months. The National Institutes of Health (NIH) states that PAWS is a temporary neurochemical imbalance and improves as the brain mends.
Treatment of diazepam withdrawal side effects requires medical and emotional assistance. Physicians are able to develop a taper program, which can help to reduce the dosage gradually so as to give the nervous system time to adapt. There are situations when supportive drugs can be prescribed to control blood pressure, sleep, or nausea.
The healing process is facilitated by therapy, hydration, nutrition, and sleep hygiene. Peer-reviewed research published in addiction medicine journals indicates that the outcomes of long-term recovery and reduction of complications are better with supervised detox. Substance Abuse and Mental Health Services Administration (SAMHSA) recommends that benzodiazepine detox cannot be performed alone, as it may cause seizures and is extremely unpleasant psychologically.
In the case of diazepam withdrawal in you or a loved one, expert attention may be the difference. Silicon Valley Recovery Center is an evidence-based and medically regulated detox and treatment center for physical and emotional health protection. Their clinical employees are familiar with how to address signs of diazepam withdrawal safely, compassionately, and professionally. You do not have to bear this alone.
Agitation, insomnia, tremors, nausea, and mood swings are the most common symptoms of diazepam withdrawal. These are expressed as the nervous system becomes hypersensitive after stopping the drug.
The diazepam withdrawal normally occurs during the initial week, beginning within the first 24 hours. After stabilization of the brain, the symptoms slowly disappear in a few weeks.
Most acute diazepam withdrawal is two to four weeks. Some emotional symptoms are likely to continue as a result of post-acute withdrawal.
The adverse effects of diazepam withdrawal are bad since they include seizures, excessive confusion, and abnormally high blood pressure, which is quite dangerous. These instances require urgent attention.
Extreme panic, hallucinations, seizures, or uncontrolled shaking can be bad symptoms of diazepam withdrawal. These effects indicate that there should be urgent professional detoxification.
Lorazepam withdrawal can be discouraging and even frightening, especially for individuals who were prescribed this medication to manage anxiety, insomnia, or panic attacks. Ativan is a medication commonly known as lorazepam, which is a drug substance belonging to a group of drugs referred to as benzodiazepines. These drugs work well in calming down the central nervous system, but after a prolonged period, the body gets addicted to the drugs.
The withdrawal process may commence with the reduction or maintenance of the drug; some of the severe withdrawal symptoms are physical and emotional. Being aware of what happens during lorazepam withdrawal will allow a person to be ready and find the right assistance. Mentorship makes the process less dangerous and far easier.
Lorazepam increases the activities of gamma-aminobutyric acid (GABA), which is a neurotransmitter that decelerates the activities of the brain. This is the reason why it works as an anxiety, muscle tension, and sleep medication. Nevertheless, the brain gets used to the constant generation of GABA and becomes dependent on the medication, since it is used regularly. This causes physical dependence.
According to MedlinePlus, benzodiazepines like lorazepam alter brain chemistry in a way that makes stopping the medication abruptly unsafe. During withdrawal, the nervous system becomes overstimulated, leading to some of the most unpleasant and sometimes severe effects of lorazepam withdrawal.
Early signs of lorazepam withdrawal will allow for preventing complications and allow for the more timely receipt of medical help.
In the beginning, withdrawal may feel mild. It is confused with stress or sickness for many people. The early symptoms of the lorazepam withdrawal include restlessness, headache, anxiety, difficulty sleeping, and mood change. A heightened or reduced appetite may also be observed, and even sensitivity to light or sound.
The symptoms are even more severe as the nervous system is having difficulties stabilizing the balance. This can result in panic attacks, tremors, confusion, sore muscles, and a beating heart. More serious ones are hallucinations or seizures, and individuals are advised to address the medical treatment as quickly as possible. These risks have led to caution that benzodiazepine withdrawal should never be addressed alone because of them.

The following are some of the most typical lorazepam withdrawal symptoms that people complain of:
These are some side effects of lorazepam withdrawal, as the brain is adapting to work without the drug. The extent of the condition relies on drug dosage, duration of use, and abrupt drug cessation or a gradual withdrawal.
The lorazepam withdrawal timeline differs depending on the individual; however, in most cases, it has a rough schedule. Lorazepam is a short-acting benzodiazepine, and, therefore, the withdrawal symptoms may begin rapidly, and in many cases, within 6 to 12 hours of the last administration.
The symptoms are common during the period of days 2 to 7. It is the time of the strongest discomfort for people. Symptoms can gradually improve after the first week, but with enduring effects that can take weeks or months.
Peer-reviewed research papers demonstrate that structured tapering and medical assistance help greatly in the alleviation of symptoms and their duration.
| Phase | What Happens | Duration |
| Acute Withdrawal | Anxiety, tremors, insomnia, nausea, panic, and irritability | 1 to 2 weeks |
| Protracted Withdrawal | Lingering anxiety, sleep issues, mood changes, and brain fog | Several weeks to months |
This table explains the significance of professional support. The majority of people feel better after the acute phase, but they still need instructions because of the symptoms that remain.
The question people tend to ask themselves is, How long does lorazepam withdrawal last? The severest symptoms are overcome in two weeks by the majority of people. However, the withdrawal effects of lorazepam that are mild in nature, including anxiety, fatigue, or sleeping disorders, can last quite a long time.
However, the National Library of Medicine has shown that those who taper gradually under medical attention will recuperate sooner and with less trouble than those who suddenly quit. Long withdrawal seems more prevalent among individuals who were taking lorazepam for months or years.
Although the process of lorazepam withdrawal is a scary one, it is a sign that the nervous system is growing. The other item that is critical at this stage is hydration, nutrition, and emotional support.
The facts supported by evidence, such as the National Helpline offered by SAMHSA, are capable of offering information that individuals can apply to overcome benzodiazepine withdrawal. These sources assist patients and families in making sense of what is occurring and what recovery would appear like.
Research papers and peer-reviewed materials also indicate that counseling, cognitive behavioral therapy, and supervised detox are very effective in enhancing the long-term prognosis of individuals experiencing withdrawal of lorazepam.
The lorazepam withdrawal process is not only risky, but also unnecessary to undergo. Silicon Valley Recovery offers tapering, mental health, and a customized treatment regimen under medical supervision that ensures that the physical and emotional health of individuals is preserved.
Their clinical personnel are aware of the science of benzodiazepine dependence and treat patients with respect and humane treatment. At Silicon Valley Recovery, we are capable of assisting you or the loved one you have in initiating a safer and more supportive process of recovery.
Lorazepam withdrawal symptoms are typical and are typified by anxiety, insomnia, tremors, nausea, irritability, headache, and panic attacks. In more difficult situations, hallucinations or seizures may occur.
Typically, the lorazepam withdrawal schedule takes effect upon completion of approximately 12 hours of the last dosage, then reaches its peak within the first week, and the improvement goes on in the following weeks. Medical advice on clinical grounds provided by NIH or SAMHSA indicates that individuals who taper gradually with medical care tend to have shorter and much easier recoveries.
The most common sufferers experience symptoms that take one to two weeks, although mild effects may persist for a number of months. That is why the question is so popular among people: how long does lorazepam withdrawal last, and why is medical tapering so significant?
Yes. Some of the side effects of withdrawal of lorazepam include seizures, severe confusion, and problems with heart rhythms. They can be life-threatening without being medically supervised.
Go to the doctor immediately in the case of seizures, hallucinations, excessive agitation, high fever, or irregular heartbeat. These are the signs of lorazepam withdrawal that point to a healthcare crisis.
Are you struggling to help a friend or a loved one who is misusing alcohol? We know how hard and stressful it can be to watch someone you care about be harmed by drinking too much. Our guide will teach you how to accurately spot the symptoms of alcohol use disorder and have a productive and compassionate conversation about this issue.
It is not easy to support someone on their journey to sobriety – but your care and guidance can make a huge difference in their life. Use our tips to find the right words and the right time to talk to your friend or your family member about cutting alcohol out of their life.
![]()
Before you talk to your friend or family member about their drinking problem, it is crucial to comprehend the scope of the issue, both for the person struggling with addiction and the people around them. While moderate alcohol consumption is generally not considered harmful, becoming dependent on alcohol will lead to negative consequences both for the physical health of the individual and their lifestyle.
Alcohol abuse may lead to numerous health complications – high blood pressure, liver disease, stroke, digestive problems, and cancer, to name a few. In addition, a person who suffers from alcohol addiction may struggle to maintain their normal lifestyle – they can have problems at work or in school, get into fights with their friends, and be isolated from their peer group, and face legal troubles due to their erratic behavior.
There is no one single symptom of alcohol addiction; however, there are several red flags you can pay attention to, especially if your friend has been acting strangely lately. Here are a few common behavioral and physical signs of alcohol use disorder (AUD):
● High tolerance. If your friend has been drinking more than usual and they do not seem to be intoxicated after consuming large quantities of alcohol, they may have developed a high tolerance for alcohol – this is one of the main signs of addiction.
● Mood swings. Has your loved one seemed irritable, anxious, or aggressive lately? Their bizarre behavior may be linked to alcohol addiction, especially if they are showing symptoms of depression.
● Withdrawal symptoms. When a person feels unwell after they stop drinking alcohol, it may be a sign of withdrawal. Pay attention to symptoms such as headaches, nausea, sweating, and shaky hands – your friend may require medical assistance to safely detox from alcohol.
![]()
Choose the right time to sit down with your friend and have a private conversation with them. You should speak to them when they are sober, and no one is around to interrupt your discussion. It is recommended to talk to your friend in a familiar, comfortable environment – for instance, you may come over to their place and speak to them at home.
There is no “right” thing to say to a person with an alcohol problem – every conversation will be unique. However, you should aim to express your concerns without accusing your friend or making them feel guilty. Let them know you have noticed the changes in their behavior, explain the dangers of alcohol addiction, and offer your help – it may be a good idea to reduce alcohol consumption or quit drinking altogether.
Your job is not done after you talk to your loved one one time – whether your friend listened to your concerns and decided to keep drinking or they agreed to embrace sobriety, be there for them in the future. A short, friendly message or a quick visit to check up on your friend will be appreciated.
If your loved one decided to give up alcohol, remind them of their achievement if they start backtracking in their decision – for instance, if they feel left out when your friend group goes to the bar, invite them to join you in alcohol-free activities you can enjoy together. In case the behavior of your friend does not change for the better, you may talk to their family and reach out to mental health professionals together.
You do not have to handle this challenge on your own – nowadays, there are many organizations and individuals specializing in addiction treatment that will be able to assist you and your friend. Below you can find a few resources that may be useful to you and your loved one:
● Substance Abuse and Mental Health Services Administration (SAMHSA). Contact SAMHSA at 1-800-662-4357 to get free, confidential guidance 24/7 – their representatives will be able to refer you to the nearest treatment facility.
● Alcoholics Anonymous (AA). Join the support group in your area to meet other people who struggle with alcoholism and attend meetings together with your friend – you may find a local chapter of AA on their official website.
● Silicon Valley Recovery (SVR). Get in touch with our team of professionals who have experience in dealing with alcohol addiction and recovery – we will design a personalized treatment plan for your friend and help them start their journey to sobriety.
Common signs of alcohol addiction include high tolerance to alcohol, withdrawal symptoms such as nausea and headaches, and mood swings.
Alcohol misuse may lead to serious health problems – for instance, a person may suffer from heart disease or cancer. Moreover, alcohol addiction will negatively impact a person’s life – their productivity will go down, they may get into fights with friends, and their behavior may lead to legal troubles.
When you talk to your friend about their alcohol problem, tell them you are worried about their well-being and list the symptoms you have noticed – make sure they know you are not blaming them and are willing to support them on their recovery journey.
There are several ways to assist a loved one with this challenge – talk to them to express your concern, be there for them in the future, even if they decide to keep drinking, and reach out to mental health professionals who specialize in addiction recovery.
Alcohol Use Disorder (AUD) can be defined as a person’s inability to control their drinking despite the negative consequences of this behavior. If your friend suffers from AUD, you should talk to them and persuade them to give up alcohol for their own well-being.
Talking to a friend or a family member about their drinking habits may feel daunting, yet it is necessary to prevent long-term addiction and the negative consequences associated with alcohol misuse. From recognizing the symptoms of alcoholism to enlisting the help of a professional therapist, you can do a lot to help your loved one.
Our team at Silicon Valley Recovery is here to assist you and your friend—do not hesitate to get in touch with us, share your concerns, and find the best treatment for your loved one. Reach out to us today.
The process of morphine withdrawal may be overwhelming, frightening, and very uncomfortable, particularly to those individuals who use this harsh opioid to treat pain or overcome emotional distress. Dependence on morphine in the body and then abruptly quitting it does not only cause discomfort. It has a compound effect of physical and psychological responses, which may be severe and uncontrollable. Knowledge of the process that occurs during withdrawal of morphine assists individuals to plan, be safe, and take the initial step towards recovery without feeling fear.
All health organizations, including the National Institute on Drug Abuse, focus on the idea that opioid withdrawal is a disease, not a personal failure. It is a symptom of the morphine altering the brain chemistry over time, and not a weakness. In the presence of the appropriate support, individuals will be able to get through this stage and restore a sense of stability.
Morphine is an opioid that is administered for moderate to severe pain, usually postoperative, injury, or cancer treatment. It functions by stimulating opioid receptors in the brain and the spinal cord, which alleviates pain and at the same time produces a sense of relaxation and relief. With time, the repeated exposure causes the brain to become dependent on morphine to be able to perform the normal functions.
It is this biological adaptation that makes people addicted. As the morphine concentration decreases, the nervous system overreacts and produces the misery that is characterized by morphine withdrawal. MedlinePlus claims that opioids inhibit the body’s ability to control pain along with the dopamine signal, and this is why it leads to physical and emotional instability when quitting.
The long-term use leads to tolerance, i.e., it requires higher doses in order to get the same effect. It is a cycle that increases the chances of dependence and worsens morphine withdrawal symptoms in case of reduction and/or discontinuation of the drug.
The symptoms of morphine withdrawal usually start a few hours after the final dose. In the case of short-acting morphine, some of the early symptoms can begin as early as 8 to 12 hours after administration. Delaying symptoms may be achieved with long-acting versions.

The initial signs of morphine withdrawal seem to be a severe case of the flu with anxiety. Sweating, yawning, restlessness, watery eyes, and aches may be observed. Sleeping becomes complicated, and a very strong temptation to use morphine once again may engulf you. The body experiences these cravings, which alter the brain’s reward system, rather than weakness.
These initial phases may be easy to cope with, but they tend to escalate pretty fast; hence, medical intervention is highly encouraged.
The morphine withdrawal symptoms are both physical and mental. Physically, the body cannot control pain, temperature, digestion, or the control of the muscles. People can be afraid, panic, be sad, or be very irritable emotionally.
Morphine withdrawal is also known to have common side effects such as nausea, vomiting, diarrhea, chills, tremors, headaches, and rapid heartbeat. There are also sleep problems and tiredness. Depression, anxiety, and emotional numbness tend to come together with physical distress on the emotional front.
The first few days are normally characterized by worsening. Because morphine is excreted in the body, the nervous system is under stress, which it releases. The result of this is sweating, excessive thoughts, and high pain sensitivity. Journals such as the American Journal of Psychiatry have published peer-reviewed articles confirming that opioid withdrawal is at its peak levels when the brain is most unable to re-equilibrate.
Emotional distress and physical pain boost one another. Anxiety increases when the body is aching. Pain is more intense when there is an increase in fear. This cycle is the reason why morphine withdrawal cravings are so strong. It is also the reason why professional detox care enhances results.
The time frame of morphine withdrawal depends on the amount of morphine used, the duration of morphine use, and the type of morphine used, i.e., short- or long-acting. Overall, the symptoms are predictable. Let’s discuss in the table below.
| Phase | What Happens |
| 6 to 12 hours | Early anxiety, sweating, muscle aches, yawning |
| 1 to 3 days | Peak nausea, vomiting, cramps, agitation |
| 4 to 7 days | Symptoms slowly decrease; sleep remains poor |
| 2 to 3 weeks | Mood changes, fatigue, lingering cravings |
The patterns reflected in this table are the ones defined by SAMHSA. Emotional symptoms can be more enduring, whereas discomfort disappears.
The most severe period typically takes place on the first three days. The majority of physical symptoms improve at the end of the first week. Depression or anxiety can also be experienced, but becomes easier to manage.
The question that many are asking is How long does morphine withdrawal last? In the majority of people, the acute symptoms take between five and ten days. Nevertheless, persistent fatigue, sleepiness, withdrawal symptoms, and mood swings may continue for weeks. This extended phase is commonly referred to as post-acute withdrawal.
The duration is dependent on the duration that morphine was taken, the dose, and general well-being. Individuals who administered greater dosages or abused morphine with other drugs usually take a considerable amount of time to recuperate.

Treatment of side effects of morphine withdrawal is safe only with medical assistance and emotional support. SAMHSA prescribes medically monitored detox, as medications are able to relieve nausea, pain, and cravings, as well as test vital signs.
The following are useful tactics in the withdrawal:
Morphine withdrawal does not have to be done alone. Professional care can be the difference between experiencing pain and going through it without problems. Silicon Valley Recovery is a supportive setting that provides medically supervised detox, therapy, and long-term addiction treatment. With a team that understands both the physical and emotional sides of dependence, patients receive care that is safe, structured, and compassionate. This kind of support not only eases withdrawal symptoms but also helps build a strong foundation for long-term recovery.
Contact Silicon Valley Recovery to get help today!
The earliest morphine withdrawal symptoms include anxiety, sweating, yawning, and muscle aches. These usually begin within 8 to 12 hours after the last dose.
The morphine withdrawal timeline typically lasts 7 to 14 days for the acute phase. Some emotional and sleep-related symptoms may continue for several weeks.
Most people feel the worst symptoms for about 5 to 10 days. Milder effects like fatigue and mood changes can linger longer.
Common side effects of morphine withdrawal include nausea, diarrhea, chills, and anxiety. Sleep problems and cravings are also very common.
Severe dehydration, chest pain, confusion, or uncontrolled vomiting are dangerous signs of morphine withdrawal. Suicidal thoughts or medical distress need emergency care right away.
Alcoholism, a severe form of alcohol use disorder, is a chronic disease characterized by an inability to control or stop drinking despite adverse consequences. Excessive alcohol consumption leads to numerous physical and mental health issues, impacting personal and professional life and reducing life expectancy. Understanding the dangers of alcohol addiction and how long it takes to die from alcoholism is crucial for timely intervention and prevention.
Several factors determine how fast a person may die from alcohol poisoning or related health conditions, from the average amount of alcohol consumed daily to co-occurring disorders and lifestyle. In this guide, we will explore the life expectancy of people diagnosed with an alcohol use disorder (AUD), the main factors affecting the prognosis, and the benefits of quitting alcohol.
![]()
On average, people addicted to alcohol die 24-28 years earlier than individuals who do not drink. One study found that the mean age of death for men diagnosed with alcoholism was 47-53 years, depending on the study group. For women, the average age of death was 50-58 years.
For comparison, according to the CDC Centers for Disease Control and Prevention, the average life expectancy in the United States for the general population is 76.4 years, 73.5 years for men, and 79.3 years for women. Excessive alcohol consumption significantly reduces a person’s lifespan, especially if left untreated.
The life expectancy of an individual suffering from alcohol addiction depends on numerous factors, including:
There are many ways in which alcohol kills a person, from acute alcohol poisoning to chronic conditions caused by long-term alcohol consumption:
![]()
The best thing you can do for your health is to give up alcohol, return to a healthy lifestyle, and add a few more years to your life. Here are a few benefits of alcohol cessation:
On average, alcohol addiction reduces a person’s lifespan by 25 years—compared to non-drinkers, individuals diagnosed with AUD die much younger.
The leading cause of death among people who struggle with alcoholism is cardiovascular disease—excessive drinking is known to contribute to high blood pressure, arrhythmia, heart attacks, and strokes.
Research shows that one in ten adults between 20 and 64 years old dies prematurely because of alcohol consumption. In the group of people aged 20-49 years, one in eight deaths is attributed to drinking.
In some cases, alcohol detox may be fatal – symptoms like seizures and delirium tremens pose a serious danger to the person’s life. This is why it is important to undergo alcohol withdrawal under medical supervision.
Yes, it is possible to overcome alcoholism with the help of healthcare professionals and the support of your loved ones. Talk to a doctor you trust to come up with a treatment plan that suits your needs.
Alcoholism drastically shortens a person’s life; from chronic health issues to premature death, there are many dangers associated with alcohol addiction. Fortunately, this is a problem you can solve—as soon as you quit drinking, you will be able to reap the benefits of sobriety and prolong your lifespan.
Whether you are struggling with alcohol addiction or worried about a loved one who drinks, our team is here to help you. Silicon Valley Recovery offers personalized treatment plans for patients with AUD—reach out to us today to start your recovery journey.
Experiencing hot flashes after enjoying a drink or two can be an uncomfortable surprise. While hot flashes are often associated with menopause and hormonal changes, alcohol consumption is also a known trigger for this phenomenon. In most cases, hot flashes after drinking are mild and should not be a cause for concern.
If you would like to learn how to get rid of hot flashes after drinking alcohol as well as prevent this reaction in the future, there are several simple steps you can take. In our guide, we explore the connection between hot flashes and alcohol and provide effective solutions to this problem.
![]()
Before you can treat hot flashes after alcohol consumption, it is important to understand why this reaction occurs in the first place. Several factors may contribute to hot flashes triggered by drinking.
The main reason why alcohol may cause hot flashes is the effect of drinking on your cardiovascular system. Alcohol is known to increase your heart rate and raise your body temperature. As blood vessels in your skin dilate, you may experience a sensation of warmth and observe skin redness.
If you are going through menopause, hormonal changes caused by this process, combined with the vasodilating properties of alcohol, may lead to hot flashes. Women who drink during menopause are also more likely to suffer from night sweats after consuming alcohol in the evening.
There are several methods you can try to get relief from hot flashes after drinking alcohol.
Drink Cold Water
One of the easiest ways to lower your body temperature and hydrate yourself is to drink a glass of cold water after you get a hot flash. If you are at a party or in a bar, remember to ask for water with your drinks.
Put Ice Packs on Your Skin
Applying something cold to your skin, such as an ice pack or a wet washcloth, can help you cool down and feel better. Focus on such areas as your neck, forehead, and wrists for the best results.
Practice Deep Breathing
When you start feeling unwell, take a few minutes to step outside, get some fresh air, and practice deep breathing. This will help you calm down, reduce stress, and accelerate your recovery.
While hot flashes after alcohol intake are usually harmless, it is best to avoid this unpleasant experience in the future. Here is what you can do to prevent hot flashes:
Identify Drinks That Cause Hot Flashes
Some types of alcohol may be more likely to give you hot flashes. For example, beverages with a high alcohol percentage, such as vodka or whiskey, are a common trigger for this reaction. Pay attention to how your body reacts to different drinks so you can avoid those that do not suit you in the future.
Wear Light Clothes
Your outfit can have a huge impact on your comfort when you drink. Choose loose clothes made of breathable fabrics—this way, if you do get a hot flash, you will not feel restricted by what you are wearing.
Reduce Your Alcohol Consumption
Perhaps the best way to prevent hot flashes is to cut down on drinking or quit alcohol altogether. There are many benefits to giving up alcohol, from improved physical health to better sleep and mental clarity.
![]()
In most cases, hot flashes should not alarm you—this is a short-term issue you can resolve within minutes. Nonetheless, sometimes hot flashes are a symptom of a more serious problem that requires a visit to a healthcare provider.
If your hot flashes persist for a long time and you struggle to get rid of them, you feel dizzy and nauseous after drinking, or you have chest pain and difficulties breathing after consuming alcohol, you should see a doctor. A medical professional will examine you and create a personalized treatment plan suited to
your needs.
You can feel a hot flash coming if you suddenly feel warm or even hot in particular areas of your body—usually the face, neck, and chest. Hot flashes are often
accompanied by excessive sweating and skin redness.
Yes, alcohol can give you hot flashes. This may happen due to the dilatation of blood vessels, increased heart rate, and higher body temperature after you drink
alcohol.
Women who go through menopause are sometimes advised to give up alcohol; hormonal changes combined with the negative effects of alcohol on the endocrine
The system may exacerbate the symptoms of menopause, including hot flashes.
Fortunately, the duration of a hot flash is usually short—on average, it lasts for three to four minutes. In rare cases, hot flashes persist for ten minutes or
longer.
You can deal with a hot flash after drinking by rehydrating your body, pouring cold water on your skin, breathing deeply, and stepping away from a hot or
stressful environment.
Hot flashes are certainly unpleasant, but with the help of our tips and tricks, you will be able to manage and prevent them! Pay attention to the signals your body
sends you—if drinking alcohol leads to discomfort, it may be better to reduce or quit consumption.
Are you struggling with hot flashes and looking for assistance with alcohol withdrawal? Reach out to Silicon Valley Recovery! Our team will be happy to support you in designing a unique treatment plan and help you on your recovery journey.
“`
Oxycodone withdrawal is a difficult and often daunting process, particularly for those who have developed a physical addiction to this powerful opioid drug. Whether oxycodone was initially prescribed to manage pain or misused, the body can easily get used to its use.
Withdrawal symptoms occur when the use is reduced or stopped as the nervous system strives to restore the balance. This guide explains the science of opioid dependence, oxycodone withdrawal symptoms, the complete withdrawal schedule of oxycodone, and how the side effects and suffering can be reduced with treatment that is medically administered.
Oxycodone functions by attaching to the opioid receptors located in the brain and the spinal cord that inhibit the transmission of pain and create an effect of relaxation or feelings of euphoria.
Repeated exposure to the drug causes the brain to slow down its natural secretion of endorphins and rely on the drug to function normally. When oxycodone use stops, the brain and nervous system are left without proper regulation of chemicals, and withdrawal occurs.
Neurologically, opioid dependence is not a vice – it is a biological reaction that can be expected. A study carried out by the National Institute on Drug Abuse (NIDA) also found that the long-term use of opioids alters the dopamine signaling and stress-responsive brain mechanisms. Such changes lead to tolerance (needing more and more to achieve the same effect) and dependence (needing the drug to feel comfortable).
When oxycodone use ceases, the body responds by becoming withdrawn as it tries to restore normalcy. This is why oxycodone withdrawal symptoms become so severe, and why the help of a medical worker is frequently needed.

Early symptoms of oxycodone withdrawal may appear within hours of the intake of short-acting formulations. Most people report experiencing uneasiness, anxiety, or restlessness. Poor sleep patterns are common, and so are yawning, sweating, and muscle pains.
Common Symptoms of Oxycodone Withdrawal
The oxycodone withdrawal symptoms are different in terms of severity, and this is based on the dosage, the period of use, and other health reasons that are unique to every individual. Symptoms are both physical and mental.
These are rather disturbing oxycodone withdrawal side effects that do not pose life-threatening conditions when placed under the care of a doctor. However, dehydration, electrolyte imbalance, and comorbid mental health issues can pose serious risks.
The oxycodone withdrawal timeline is quite predictable, but it may vary for individuals:
| Timeframe | What to Expect |
| 6–12 hours | Early withdrawal begins with anxiety, restlessness, and sweating. |
| 24–48 hours | Peak symptoms – nausea, vomiting, muscle pain, insomnia |
| Days 3–5 | Symptoms remain intense but begin to stabilize. |
| Days 7–10 | Physical symptoms gradually subside. |
| Weeks to months | Psychological symptoms and cravings may persist. |
This timeline explains the importance of professional detox. Medications and supportive care can significantly reduce the intensity of the symptoms and prevent complications during the time of maximum withdrawal.
A common question is: how long does oxycodone withdrawal last? It is a common question, the answer to which varies depending on a number of factors. The period of acute withdrawal is usually 7–10 days, the most severe effects of which are experienced during the first 72 hours. But there are those who have lingering symptoms of fatigue, sleep problems, or even depression, which is commonly termed as post-acute withdrawal syndrome (PAWS).
The duration of withdrawal of oxycodone depends on the history of dosage, the length of use, whether the drug was an extended-release or immediate-release, as well as metabolic well-being, along with the presence of co-occurring substance use or mental health issues.
SAMHSA states that individuals who detox under medical care have a higher chance of safely going through withdrawal and entering into continuous therapy, thereby minimizing chances of relapse.
Treatment of the side effects of oxycodone withdrawal without medical intervention may be very challenging and may even lead to fatalities. Recovery efforts can easily be stalled by dehydration, extreme vomiting, and emotional instability. Symptom-relief medications, hydration, and constant monitoring are provided by medically supervised detox.
Buprenorphine or clonidine are examples of evidence-based medications that can be used to decrease the cravings and stabilize the vital signs. Behavioral support is also very instrumental, since anxiety and depression tend to be at their highest point during withdrawal.
Educational materials by the National Institute of Drug Abuse stress that detox is not a treatment but the initial step to long-lasting recovery, when detox is followed by therapy and professional care.
The process of oxycodone withdrawal does not require self-administration. At Silicon Valley Recovery, treatment programs are designed primarily to help individuals feel physically more stable and recover successfully in the long term, with the support of caring professionals through medically guided detox and treatment programs.
With 24/7 healthcare and a patient-centered approach, individuals can withdraw safely and prepare to heal in a sustainable manner. Silicon Valley Recovery is the place to begin your path toward permanent recovery, especially when you or someone you love is experiencing Oxycodone withdrawal.

The early symptoms are anxiety, restlessness, perspiration, yawning, and insomnia. These symptoms may appear 6-12 hours after the last dose
Oxycodone withdrawal timeline starts within a period of less than one day and peaks within two to three days. A period of one to two weeks is enough to see the body symptoms improve, though the cravings may not go away.
Acute oxycodone withdrawal typically lasts 7-10 days. In the next few weeks, other individuals will experience lingering emotional symptoms that will not require further treatment.
The most difficult are usually reported to be muscle pain, nausea, insomnia, anxiety, and intense cravings. Oxycodone withdrawal has these side effects that may be overwhelming unless the person gets medical assistance.
This requires urgent care in the case of severe dehydration, vomiting that cannot be controlled, chest pain, or suicidal thoughts. Such medical or mental health risks may be severe because of these oxycodone withdrawal symptoms.
Alcohol withdrawal is a challenging and often uncomfortable process that occurs when someone who has been drinking heavily for a long time suddenly stops or significantly reduces their alcohol intake. Understanding the timeline of alcohol withdrawal symptoms and the best ways to manage them is crucial for a safe and successful recovery. Whether you are concerned about your drinking habits or want to help a loved one who wants to quit drinking, it is important to know what to expect during alcohol withdrawal.
How long does it take for alcohol withdrawal to go away? The symptoms of alcohol withdrawal usually begin within a few hours after the last drink and may last for several weeks, depending on the severity of alcohol use disorder. In some cases, people develop a potentially life-threatening condition known as delirium tremens and require professional medical assistance to deal with alcohol withdrawal. In this blog, we will explain the main symptoms of alcohol withdrawal, the typical duration of withdrawal from alcohol, and effective methods to relieve the symptoms.
![]()
Alcohol withdrawal happens when a person who is dependent on alcohol decides to quit alcohol or reduce the consumption of alcohol. Chronic alcohol use affects the chemicals in your brain—in particular, it reduces the production of gamma-aminobutyric acid (GABA), which is responsible for having a calming effect on your brain. It also increases the production of excitatory neurotransmitters such as norepinephrine.
When you stop drinking alcohol, your brain may become overexcited, and you may experience a variety of unpleasant symptoms from mild anxiety to severe agitation. It is never a good idea to go through alcohol withdrawal on your own—reach out to friends and family and ask for help from medical professionals to ensure your safety.
Here is a list of physical and mental symptoms you may suffer from when you stop drinking:
While most people only have to deal with mild symptoms that go away on their own within a few days, in rare cases alcohol withdrawal leads to a condition called delirium tremens (DTs). If you or the person you are caring for starts shaking and sweating profusely, becomes disoriented and confused, and has visual hallucinations, bring them to the hospital as soon as possible.
![]()
On average the alcohol withdrawal timeline spans a week. However the symptoms may persist for weeks and even months
Here is what the timeline looks like:
The length of alcohol withdrawal depends on several factors—it is unique to every individual.
People who have been drinking for years and have consumed large quantities of alcohol regularly whereas are more likely to struggle with withdrawal. If a person has tried to quit drinking before and gone through withdrawal in the past, the symptoms may be more severe the next time they stop consuming alcohol. Younger individuals have a better chance of coping, with withdrawal; for an older person, it may be more difficult to quit alcohol. Pre-existing mental health conditions, such as depression and anxiety, may exacerbate the symptoms of withdrawal. It is crucial to have a solid support system made up of friends, family, and medical providers who can offer their assistance and guidance.
There are several methods you can implement to treat alcohol withdrawal.
It is advised to talk to a therapist or a doctor before you quit drinking, especially if you have an alcohol addiction—a healthcare provider will be able to design a treatment plan suitable for your needs. Let your friends and family know you are planning to give up alcohol—their encouragement and emotional support will be invaluable for your recovery. Even if you cannot enter a rehab facility, you should be under the supervision of a doctor who can prescribe certain medications to deal with withdrawal. Drugs like lorazepam and diazepam can be used to reduce anxiety and prevent seizures.
Make sure you adhere to a healthy lifestyle. Eat nutritious meals, stick to the sleeping schedule you are comfortable with, and drink plenty of water to stay hydrated. You have to avoid situations that trigger you to drink, but it does not mean you should withdraw from social events.
Alcohol withdrawal is a set of physical and psychological symptoms that start when a person who suffers from alcohol dependence stops drinking.
The symptoms of alcohol withdrawal are numerous—a person may have headaches, nausea, and agitation, and in severe cases, hallucinations and seizures.
In most cases, the withdrawal symptoms begin 6 hours after the last drink—a person may feel anxious, have a headache, and struggle to fall asleep.
Typically, it takes 3-7 days to get through alcohol withdrawal—the symptoms will peak on the fourth day after you stop drinking.
Yes, it is recommended to reach out to a healthcare provider and ask for their assistance with alcohol withdrawal—they will be able to prescribe you medications to manage the symptoms.
We hope that our guide was able to answer your question—how long does it take for alcohol withdrawal to go away?—and that you learned the basics of alcohol withdrawal and its treatment. Remember that you do not have to go through this challenge on your own—rely on your close ones and bring in professionals to help you!
Silicon Valley Recovery specializes in alcohol addiction treatment—our team will be glad to assist you! Reach out to us to discuss your unique circumstances, and we will design a personalized plan to fit your needs.
Cessation or abandonment of drugs related to opioids might not be an easy task, particularly in cases where a person begins becoming physiologically dependent on the drug. Buprenorphine withdrawal is a medically recognized condition that occurs when the medication is abruptly stopped or gradually tapered after habitual or prolonged use, often leading to physical and psychological symptoms.
Despite the success of buprenorphine as a treatment for opioid use disorder, withdrawal from it may result in undesirable and even protracted withdrawal symptoms. The information about buprenorphine withdrawal, its symptoms, and seeking medical assistance can facilitate the process of recovery.
Buprenorphine is a partial opioid agonist found in medications such as Suboxone and Subutex. It acts by binding with the opioid receptors in the brain, reducing cravings and withdrawal symptoms without producing the full effects of full opioid agonists that produce intense euphoria. Because of this distinctive action, buprenorphine is an important component of medication-assisted treatment (MAT) of opioid use disorder.
However, over time, the body can develop dependence on buprenorphine despite it being used in the appropriate dose. Dependence occurs when the brain adjusts the production of natural opioids and the responsiveness of these receptors. When the drug is reduced or withdrawn, the nervous system reacts to it, and buprenorphine withdrawal symptoms occur.
Buprenorphine has a long half-life, and therefore, the withdrawal symptoms may take a long time to show, unlike other short-acting opioids, which do not show instantaneously. The early withdrawal symptoms are usually mixed with a flu-like sickness or emotional burnout.
The Substance Abuse and Mental Health Services Administration (SAMHSA) indicates that guided tapering and expert monitoring are the most relevant factors that help minimize withdrawal symptoms and the potential for relapse.
Buprenorphine withdrawal has both physical and psychological symptoms. Physical symptoms do not pose a life-threatening risk of the condition, although they may be unpleasant, whereas psychological ones may be the hardest to get through on the road to recovery.
On the physical level, one may experience gastrointestinal upsets, headaches, fatigue, muscle cramps, and appetite changes. Such symptoms are caused by the fact that the absence of stimulation of the opioid receptors does not enable the nervous system to maintain balance.
Concurrently, it could also have psychological connotations where the feelings of anxiety, depression, irritability, and intense cravings are factored in, particularly in persons with comorbid mental health disorders.

Daily tasks may become difficult during withdrawal. Focus can become impaired, sleep disorders may increase fatigue, and emotional instability may put relationships or job performance under pressure. Many people report feeling overwhelmed by burnout and stress, and it may make them more willing to get back to opioids just to have some relief.
Although the majority of buprenorphine withdrawal symptoms can be resolved with the right support, medical assistance is highly advised when the symptoms do not subside within the time frame or lead to severe depression or attempts to end life.
The buprenorphine withdrawal schedule is different for each patient based on the dosage, time of use, metabolism, and health condition. The withdrawal may be delayed because of the long half-life of buprenorphine as opposed to other opioids.
| Stage | Timeframe | Typical Experience |
| Early onset | 24–72 hours | Anxiety, restlessness, mild aches |
| Peak phase | Days 3–10 | Strong physical symptoms, cravings |
| Subacute phase | Weeks 2–4 | Fatigue, mood swings, insomnia |
| Post-acute | Weeks to months | Emotional sensitivity, low energy |
This is the reason why professional guidance is so crucial due to this long schedule. Studies published in peer-reviewed journals and cited by the National Institute on Drug Abuse (NIDA) indicate that a progressive tapering program decreases the severity of symptoms, as well as the duration of symptoms.
One of the questions is how long does buprenorphine withdrawal last? The acute withdrawal symptoms usually disappear within two to four weeks, but the long-term consequences or effects may still be experienced even after a few weeks (now termed as post-acute withdrawal syndrome or PAWS). These may be low motivation, disturbed sleep, and emotional instability.
The process of withdrawal tends to take much time, depending on whether the drug was discontinued or was decreased gradually. Those who are being tapered under the supervision of a medical practitioner usually have fewer and relatively mild withdrawal periods.
The side effects of buprenorphine withdrawal could be unbearable, yet with the support network, one can get through it. The treatment is geared towards stabilization of physical pain and emotional distress, and reducing the chances of relapse.
Among the interventions that may be implemented by high-quality withdrawal management are hydration, nutritional support, sleep regulation, and medications to mitigate some of the typical symptoms of nausea, anxiety, or insomnia. In practice, practitioners can utilize Buprenorphine withdrawal in a clinical setting to modify taper regimens or to incorporate supportive interventions to ensure that the procedure is comfortable and safe.
The process of buprenorphine withdrawal does not necessarily have to be done alone. Professional care provides a guideline, security, and compassionate care throughout all recovery processes. Silicon Valley Recovery also provides evidence-based approaches, which focus on an individual, to help people overcome the symptoms of withdrawal as they build a durable platform that helps them be sober in the long term. If you or a loved one is struggling with buprenorphine withdrawal, contact Silicon Valley Recovery today to start your journey toward lasting recovery.

The typical buprenorphine withdrawal symptoms are anxiety, insomnia, muscle aches, sweating, nausea, and drug cravings. Irritability and low mood are also very common emotional changes reported.
The withdrawal schedule of buprenorphine usually starts 24-72 hours following the final dose, peaks during the first 1-2 weeks, and slowly subsides thereafter. Some people can experience lingering symptoms that can take several weeks.
The answer to the question is that most individuals have an acute period of two to four weeks during which they experience withdrawal symptoms of buprenorphine. The psychological effects could be mild and thus long-term without adequate support.
Other possible withdrawal symptoms of buprenorphine include fatigue, sleeping problems, stomach problems, mood swings, and insomnia. The degree of the problem lies in the dose, duration of use, and the tapering mode.
The main symptoms of buprenorphine withdrawal that involve the use of professional assistance are severe anxiety, continuous insomnia, strong cravings, or an inability to operate. Medical care may minimize the risks and enhance the outcomes of recovery.
Struggling with alcohol addiction can be a daunting experience, affecting every aspect of a person’s life, from personal relationships to work performance and the state of a physical body and mental well-being. There are many ways to address this problem, from therapy and support groups to inpatient and outpatient treatment, as well as simple and effective home remedies to stop drinking alcohol.
In our guide, we will explore the benefits of quitting alcohol, remedies you can try on your own, and the advantages of implementing these solutions. Lowering your alcohol consumption or cutting it out of your life completely will lead to a happier and healthier future.
![]()
It is crucial to be aware of the negative consequences of alcohol addiction, whether you are struggling with this issue yourself or worried about the drinking habits of a person you care about. While on the surface, alcohol may seem like a harmless way to relax and have fun, when drinking becomes excessive and chronic, it leads to numerous problems.
From minor symptoms such as headaches and nausea to the increased risk of heart disease, stroke, and liver damage, the adverse effects of alcohol on a person’s physical health are well-documented. Besides, alcohol abuse is often linked to mental health disorders—many people rely on alcohol to cope with stress and anxiety.
One of the best natural remedies to give up alcohol is to modify your diet. The food you consume may either help you deal with withdrawal symptoms or exacerbate the problem.
Here are a few dietary tips to stop drinking:
There are many vitamins and herbs to stop drinking alcohol that you can add to your diet to speed up your recovery. Below you can see the list of supplements that will assist you in the process:
To successfully give up alcohol, you should make changes in your daily routine and surroundings. Implement the following suggestions to lower your alcohol consumption:
![]()
While home remedies can certainly be helpful, it is important to reach out to a healthcare provider when the situation gets out of control. A doctor will be able to diagnose the issue, prescribe medication, and come up with a personalized treatment plan that suits the patient and their unique circumstances.
In addition, you may want to contact a mental health counselor or a therapist and explore the reasons behind the addiction with a professional. Very often, alcohol abuse has underlying psychological causes that should be addressed during therapy.
Answer: Some of the initial steps to quit drinking include recognizing the problem, setting a goal, reaching out for support, and avoiding triggers.
Answer: Giving up alcohol will improve your physical and mental health, boost your energy levels, enhance your appearance, and help you build better relationships with those around you.
Answer: You should supplement your diet with vitamins B, C, and E – these nutrients will alleviate the symptoms of withdrawal and protect your organism.
Answer: It is possible to stop drinking on your own, especially if you only drank socially in the past; however, if you were a heavy drinker, it is recommended to see a doctor.
Answer: Yes, if you or someone you care about is struggling with alcohol addiction, do not hesitate to reach out to a healthcare provider and ask for help.
There are numerous home remedies to stop drinking alcohol that you can try—from dietary adjustments to lifestyle changes. If you or your loved one is struggling with alcohol addiction, remember that you can always rely on Silicon Valley Recovery to help you in your journey to sobriety. Our team is here to support you—get in touch with us to learn more about our services
Rubbing alcohol may seem like a harmless household item, but it is incredibly dangerous to drink. It is very different from alcohol that you drink at parties or at home with friends. There is a huge difference between sipping a glass of wine and ingesting rubbing alcohol.
This blog was created to help you understand the dangers of drinking rubbing alcohol. Can you die from drinking rubbing alcohol? What should you do if someone you love drank rubbing alcohol by mistake? How can a professional team help you deal with the consequences of ingesting isopropyl alcohol?
![]()
Rubbing alcohol, also known as isopropyl alcohol, is a common household item used for cleaning and disinfection. It is present in many health and cleaning products, and it is widely used by medical professionals and ordinary people at home.
While rubbing alcohol is only meant for topical application, some people may decide to drink it. This is a terrible idea—isopropyl alcohol is not meant for human consumption, and it is dangerous to ingest it.
Yes, it is possible to die from drinking rubbing alcohol. The fatal dosage depends on a variety of factors—your age, weight, health condition, allergies, and much more. Even if you do not die from ingesting isopropyl alcohol, you may seriously harm your body by drinking it.
There is a huge difference between safe-to-drink ethanol and dangerous isopropyl alcohol. If you are worried about someone you love accidentally drinking rubbing alcohol stored in a mislabeled bottle, you should learn about the symptoms of rubbing alcohol poisoning to react fast in case of an emergency.
Here are the most common signs of rubbing alcohol poisoning you should look out for:
In some cases, a person who drank rubbing alcohol may go into a coma. Pay attention to their symptoms and make sure to get medical assistance as soon as possible.
![]()
Whether you consumed isopropyl alcohol yourself or you are worried about a friend or a family member who drank rubbing alcohol, there are a few things you can do to improve the situation.
First of all, do not panic—a clear head will help you figure out the next steps. If a person who drank rubbing alcohol is only exhibiting mild symptoms—such as an upset stomach and a minor headache—you may decide to let them stay at home and treat them there without calling an ambulance.
Nonetheless, it is recommended to get a professional medical provider to examine the person who ingested isopropyl alcohol. A doctor or a nurse will be able to properly diagnose the symptoms of rubbing alcohol poisoning and prescribe adequate treatment.
Here are a few tips you can follow to make sure no one drinks rubbing alcohol by mistake:
If you believe a person in your household drank rubbing alcohol – whether it was accidental or they consumed it on purpose – reach out to mental health professionals from Silicon Valley Recovery to get the help you need.
Our team will be able to advise you—we have a lot of experience when it comes to alcohol and drug abuse prevention and treatment. Let our experts support you and your family during this challenging time.
Rubbing alcohol is primarily composed of isopropyl alcohol and water. It is meant for external use only.
No, you should never drink rubbing alcohol—it is dangerous to ingest it.
Fatalities from rubbing alcohol are rare—it is estimated that around 150 people die from isopropyl alcohol poisoning in the US every year.
The most common signs of rubbing alcohol poisoning are stomach pain, nausea, vomiting, dizziness, and confusion.
To make sure no one in your family drinks rubbing alcohol by mistake, you should keep it out of the reach of children and always label it properly.
Accidentally or intentionally drinking rubbing alcohol can have serious consequences for a person’s health. From mild symptoms such as nausea to coma and death, isopropyl alcohol should never be consumed.
If you or your loved one drank rubbing alcohol by mistake, get in touch with Silicon Valley.
Recovery Silicon Valley Recovery to talk to our professionals. We will be able to advise you and guide you and come up with a personalized treatment plan to suit your needs.
The withdrawal effects of the benzodiazepines are one of the most difficult things to endure, and they can be experienced by either a physically or psychologically addicted person towards benzodiazepines. These medications are referred to as alprazolam (Xanax), diazepam (Valium), and lorazepam (Ativan), and they are typically utilized in the treatment of anxiety, insomnia, panic disorders, and muscle spasms.
Tolerance means that you have to take larger and larger doses of the drug to feel the same. Physical dependence is a sign that your body is accustomed to the drug, and you will suffer a withdrawal effect when you quit the drug.
In this blog, some facts relating to benzodiazepine withdrawal, its withdrawal schedule, signs, and anticipations are shared.
The benzodiazepine withdrawal phase does not always have a serious onset. There are symptoms that range from mild to more severe.
The physical symptoms may present themselves as:
These are some of the first indications that your body is adapting to drug withdrawal, and you are used to it.
The benzodiazepine disrupts brain chemistry; therefore, psychological symptoms will show themselves in the early stages:
These are all signs of your body adjusting – it is the natural rebalancing of your body. Recognizing these signs is one way to help you seek assistance during the initial stages of withdrawal.
The benzodiazepine withdrawal symptoms can be extremely diverse and will vary depending on the dose, the number of times used, and the sensitivity of the individual. These symptoms may range from minor symptoms to severe discomfort and may be classified as physical or mental.
Here is a snapshot:
According to the Substance Abuse and Mental Health Services Administration (SAMHSA), withdrawal is not only psychological, but it also has actual physiological effects.
Recovery is not immediate – it occurs in phases. Although everyone’s experience is different, most people follow a similar pattern, as shown in the table below:
| Phase | Timeframe | Common Experiences |
| Early Onset | 6–24 hours after last dose | Initial anxiety, restlessness, insomnia |
| Peak Symptoms | 24–72 hours | Heightened anxiety, tremors, nausea |
| Acute Withdrawal | 3–10 days | Strong psychological symptoms, sleep disruption |
| Protracted Phase | Weeks to months | Gradual reduction of symptoms (anxiety, sleep issues) |
It is just a general timeline of benzodiazepine withdrawal that can be used as a guide, but should not replace personal medical counseling.
The question that people normally ask themselves is, “How long does withdrawal of benzodiazepines take? Its quick response usually takes between 7 days and 3 months. The acute symptoms are generally overcome in the first 10 -14 days, but there may be a small residual effect, including some anxiety and sleep problems, and this effect may take months to vanish.
There are a number of significant variables that determine the duration of withdrawal:
The National Library of Medicine research argues that prolonged withdrawal symptoms may take months to disappear in some cases, despite detox under medical care. This has been the main reason why a detailed care plan is essential.
Withdrawal is not just about feeling uncomfortable – it also has side effects that are of medical concern. Key side effects include:
The psychological after-effects often persist the longest and put a strain on the ability to function every day.
Withdrawing from benzodiazepines may feel like a powerless experience – but you are not alone in the process. We at Silicon Valley Recovery are focused on non-hazardous, medically-monitored detox and rehabilitative care. We are aware of the intricacy of benzodiazepine dependence and offer personal care that is comprehensive, in terms of both physical and emotional needs.
If you worry about the symptoms of benzodiazepine withdrawal or would like a medically assisted detox that is as risk-free as possible, we are there to help you throughout it.
Contact Silicon Valley Recovery today and receive expert and compassionate help.

The symptoms include mostly anxiety, insomnia, tremors, irritability, and nausea. In severe cases, one can experience seizures and severe panic. The experience of each person is different.
The symptoms tend to develop within the first day of quitting and peak on days two to three before disappearing. People may experience psychological symptoms, which may require weeks or months.
Although the acute symptoms will probably subside within 10–14 days, in the vast majority of cases, for several weeks to months, in particular, anxiety and sleeping problems.
The most severe side effects may be seizures, excessive panic attacks, and cardiovascular strain. The risks are increased by the sudden withdrawal or absence of medical care.
Medical detox provides 24/7 attention, drug support, and takes an active step in case of complications. It will reduce the intensity of risk and make the withdrawal process more comfortable.
Understanding the alcohol withdrawal seizure timeline is crucial for anyone considering reducing their alcohol consumption or supporting a loved one struggling with addiction. While drinking is an accepted social activity in many cultures worldwide, heavy alcohol use is known to cause a wide range of health problems and increase the risk of accidental injuries. It is important to be aware of the symptoms of alcohol withdrawal and the dangers of quitting alcohol abruptly without medical supervision.
This article will explain what alcohol withdrawal seizures are, list the main symptoms to watch out for, describe the typical timeline of the withdrawal process, and offer treatment and management tips. We will also answer the most frequently asked questions on this topic to provide our readers with the information they need to protect their health and make safe choices.
![]()
Alcohol withdrawal seizures are a serious complication that may occur when a heavy drinker suddenly stops consuming alcohol. In most cases, seizures are preceded by mild and moderate withdrawal symptoms, such as nausea, headaches, anxiety, and tremors. People experiencing seizures may lose consciousness, shake uncontrollably, and fall to the ground, which puts them at risk of getting injured.
According to research, approximately 2 to 5 percent of patients going through alcohol withdrawal develop seizures within 2 or 3 days after quitting alcohol. The likelihood of getting a seizure depends on a variety of factors, including a history of epilepsy, previous withdrawal attempts, and concurrent health disorders. It is advised to seek medical help as soon as the initial symptoms of alcohol withdrawal appear to prevent seizures.
Mild and moderate symptoms of alcohol withdrawal usually show up within 6 hours of the last drink. Below are the most common symptoms to look out for
Alcohol withdrawal seizures are considered a severe symptom of withdrawal. Here are the warning signs of a pending seizure to be aware of
If someone you know is having a seizure, move them away from dangerous locations (for example, a busy road), put a soft object under their head, turn them on their side, and call emergency services for assistance.
While the alcohol withdrawal timeline may differ from person to person, in most cases the duration of the withdrawal fits into a 7-day timeframe.
Here is what you can expect when you stop drinking alcohol.
6 to 12 Hours
The first symptoms of alcohol withdrawal may appear as soon as 6 hours after your last drinking session. Minor symptoms you may experience during this time include
12 to 48 Hours
More symptoms may develop within 12 to 48 hours of abstaining from alcohol. It is not unusual to have
This is the period when you are most likely to get a seizure, especially if you have a history of seizures and were a heavy drinker. Make sure you are supervised by a medical professional during the first two days of your withdrawal.
48 to 72 Hours
After 2 days, more serious symptoms of alcohol withdrawal may kick in. You may go through the following
On top of that, between 48 and 72 hours, you may have an episode of delirium tremens, a severe symptom of alcohol withdrawal that requires hospitalization.
4 to 7 Days
The majority of people who go through alcohol withdrawal feel better by the end of the first week. Nonetheless, some symptoms may persist for 7 days or longer, especially if you were addicted to alcohol for a long time. It is not uncommon for psychological symptoms such as anxiety and insomnia to last for several weeks.
Remember that the alcohol withdrawal timeline depends on many factors: your drinking habits, medical history, and personal circumstances. Reach out to a doctor to come up with a personalized withdrawal plan that works for you.
There are several factors that can influence the development of seizures during alcohol withdrawal
![]()
1. How common are alcohol withdrawal seizures?
Alcohol withdrawal seizures occur in approximately 2–5% of people who suddenly stop drinking after heavy or prolonged alcohol use. While not extremely common, they are serious and can escalate quickly without proper care. Individuals with a history of seizures or multiple withdrawal attempts are at higher risk.
2. Can alcohol withdrawal seizures happen without other symptoms first?
Although most people experience early symptoms—such as tremors, anxiety, and nausea—before a seizure occurs, it is possible for seizures to appear suddenly without clear warning. This is especially true for people with severe alcohol dependence. Because symptoms can be unpredictable, medical supervision is always recommended.
3. How long after quitting alcohol can seizures occur?
Seizures most commonly occur between 12 and 48 hours after the last drink, though some cases develop as early as 6 hours or as late as 72 hours into withdrawal. The exact timing depends on individual health factors and drinking patterns. Continuous monitoring during the first two days is especially important.
4. Are alcohol withdrawal seizures life-threatening?
Yes, withdrawal seizures can be dangerous and may lead to complications such as falls, injuries, or progression to delirium tremens (DTs). Without prompt treatment, DTs can become life-threatening. Immediate medical attention significantly reduces the risk of severe outcomes.
5. How can alcohol withdrawal seizures be prevented?
The best way to prevent seizures is to undergo medically supervised detox, where healthcare providers can offer medications to stabilize the nervous system. Benzodiazepines are commonly used to reduce seizure risk and manage symptoms. Attempting to quit “cold turkey” at home increases the likelihood of complications and should be avoided.
Methamphetamine, commonly known as meth, is a powerful and addictive stimulant that affects the central nervous system. This drug has a significant impact on a person’s behavior, appearance, and mental health. Recognizing the signs of meth use can be crucial for providing timely help and support to those in need. In this guide, we will explore the behavioral and psychological symptoms of meth abuse and offer advice on addressing this issue.
Whether you suspect that your loved one may be struggling with meth addiction or want to learn more about the effects of this drug, our comprehensive resource will equip you with the necessary knowledge. From short-term agitation to long-term cognitive deficits, meth use can manifest in various ways and harm a person’s life in many aspects. Continue reading to understand how meth affects users and what you can do to assist them.
![]()
Methamphetamine is a highly addictive stimulant that affects chemicals in the brain responsible for pleasure, focus, energy levels, and more. Initially developed as a medication for narcolepsy and obesity, meth is primarily used as an illegal recreational drug nowadays.
This substance looks like a white crystalline powder with no smell and a bitter taste. People ingest meth in a variety of ways—by snorting the powder, injecting it into their veins, inhaling it through a pipe, or ingesting it in pill form. The method of administration affects the onset and duration of meth effects.
The initial effects of meth use are temporary—you may notice these symptoms for a few hours or days after the person ingests the drug. Here are the most common short-term signs of meth use you should be aware of:
● Changes in Physical Appearance
Even a brief meth use may negatively affect the way the person looks. You may see their skin is pale and sweaty, they have acne or other skin conditions, their jaw is clenched, and their lips are dry and cracked.
Meth is a psychoactive drug, which means it has a powerful effect on a person’s behavior. The user may appear more energetic and talkative than usual—while euphoria and alertness are not necessarily negative symptoms, they should raise concern when there is no apparent reason for such a mood change.
In addition to affecting a person’s looks and mannerisms, meth has an impact on their mental health. The drug may make the user anxious and confused—in certain cases, meth leads to aggressive behavior and hallucinations.
![]()
If a person continues to take meth, their addiction will lead to severe and sometimes irreversible consequences for their behavior. Chronic meth use harms a person’s life in many ways:
While it is possible to get addicted to meth after one or two intakes, when the drug use is not stopped, the person may develop a substance use disorder that will persist for a long time. Meth targets the brain chemistry of the user—their body starts to depend on the drug to function normally.
Meth is known for its negative effect on a person’s cognition. Long-term drug use is associated with memory loss, poor concentration, inability to make decisions, lack of verbal skills, and reduced motor speed.
Meth addiction will inevitably affect a person’s life. The individual may abandon their professional responsibilities and give up on their personal hobbies to focus on drug use; in many cases strained relationships with friends and family members are observed.
Methamphetamine significantly affects a person’s brain function and behavior. Here are the mental symptoms you may notice after short- and long-term meth use:
It is common for meth users to feel uneasy and agitated after they take the drug. Meth messes with the neurotransmitters in the person’s brain—once the effect of the drug wears off, the individual may feel hopeless and depressed.
In some cases meth use leads to psychosis—the person may struggle to distinguish between reality and hallucinations. If you have noticed someone is being delusional and paranoid, talk to them and reach out to a medical professional for help.
Agitation caused by meth may result in aggressive outbursts. Typically calm and composed individuals may start raising their voices and even resort to physical violence when they are confronted or provoked.
Whether the meth use of your loved one was short-lived or they have been struggling with addiction for a long time, your support and compassion combined with assistance from a mental health professional will help them to overcome this challenge. Here is what you can do to help a meth user:
It is important to speak to the individual you are worried about and share your concerns with them. Choose a quiet, private spot for a conversation; approach the person without judgment and offer your support—you may be able to convince them to give up meth and seek therapy.
● Reach out to a professional.
Get in touch with a doctor or therapist that specializes in drug addiction and ask them for advice. A mental health provider will be able to diagnose the patient and come up with a personalized treatment plan that suits the needs of the meth user.
There are numerous organizations in the country that specialize in helping meth addicts and their loved ones. You can find a local peer support group to join—being surrounded by people that can relate to your struggles will be beneficial both for the drug user and their family.
Meth use may temporarily affect a person’s appearance (pale skin, dry lips) and behavior (euphoria, increased energy levels). In most cases these symptoms disappear within a few days.
Prolonged meth use may lead to addiction and cognitive deficits (such as memory loss and poor concentration) as well as mental health issues like anxiety and depression.
Quitting sleep medication is never easy, especially at this point, since you may already be used to it. Ambien withdrawal is a real concern. It tends to be quite painful and may happen as a result of diminishing or discontinuing zolpidem (Ambien), particularly when it is used either in large doses or over a long period of time.
The anxiety can be alleviated by knowing what to look forward to, as well as helping you plan safely, not to mention that you are not alone. We are going to describe the causes of withdrawal, including why it happens, how to recognize it, the overall progression of the withdrawal, and how to manage the symptoms in a caring and humane way, as discussed below.
Ambien (zolpidem) is a prescription sedative hypnotic that is typically used to treat insomnia. Although it works well when used short-term to manage sleep problems, frequent use causes the brain to adjust itself to its existence. The nervous system may not be able to restore balance when the Ambien is abruptly stopped or tapered too quickly; therefore, Ambien withdrawal symptoms may occur.
Ambien amplifies the action of a neurotransmitter in the brain, the gamma-amino butyric acid (GABA), which calms brain activity. Over time, the brain compensates by reducing its natural calming responses.
This imbalance can cause symptoms of Ambien withdrawal, which include sleep problems and mood changes, among others, when the medication is stopped.
Timely detection of the signs of Ambien withdrawal will avoid the complicated consequences and allow you to find the necessary assistance. Changes may be observed within the first day or two after quitting, but experiences differ greatly.
Among the factors are dosage, duration of use, individual metabolism, and the use of other substances. Notably, withdrawal is not a failure of character, but rather a physiological reaction that requires medical care guided by a physician and compassion.
The most common symptoms of Ambien withdrawal are as follows:
The side effects of Ambien withdrawal are not very serious in the majority of cases; however, there are people who may experience prolonged or severe side effects, particularly after using it over a long period of time.

The Ambien withdrawal timeline will eliminate confusion and enable you to plan. The general pattern of the symptoms can be observed, but the experiences of a person vary.
| Phase | Timeframe | Typical Experiences |
| Early Onset | 6–24 hours | Return of insomnia, anxiety, restlessness |
| Peak | 2–5 days | Heightened symptoms, mood changes, sleep disruption |
| Subacute | 1–2 weeks | Gradual easing of symptoms, lingering sleep issues |
| Recovery | Weeks to months | Stabilization of sleep and mood with support |
One of the questions that comes up is, How long does Ambien withdrawal last? In most cases, acute symptoms resolve within one to two weeks. Nonetheless, sleep disorders or anxiety may be more persistent, particularly when there is no systematic taper or care.
The personal health history and the presence of coping measures, such as sleep hygiene, stress management, and counselling, determine the withdrawal of Ambien. It has been observed in peer-reviewed journals (PubMed) that medical dosage reduction, which is gradual, is more effective in enhancing comfort and results.
The side effects of Ambien withdrawal are managed by emphasizing long-term sleep health, comfort, and safety. Symptom management and changes to taper schedules may be observed through medical supervision.
The evidence-based resources, i.e., the sleep education materials of the National Library of Medicine and the guidance on sedative dependence, are helpful as background information. Behavioral strategies, such as cognitive behavioral therapy for insomnia (CBT-I), are frequently suggested and endorsed by the research as effective drug-free interventions to achieve restful sleep.
It is also the right moment to deal with some underlying factors causing insomnia, which include stress, anxiety, or unusual sleep habits. A lot of recovery centers promote whole care, a combination of medical supervision with therapy, meditation skills, and lifestyle changes.
You do not have to face Ambien withdrawal alone. Support is available for you or your loved one during this process. Silicon Valley Recovery offers personalized treatment plans that are medically supervised with the main goal of safety and comfort. Their kind staff knows the ins and outs of sedative addiction and provides care personalized to your specific needs.
Contact us today to get on the path to recovery.

Rebound insomnia, anxiety, restlessness, and irritability are the common symptoms of Ambien withdrawal. The symptoms may start in 6–24 hours of medication withdrawal.
The Ambien withdrawal timeline tends to peak in the initial days and get better after 1–2 weeks. Certain sleeping disorders or anxiety can occur without the necessary support.
The typical Ambien withdrawal symptoms are a lack of sleep, anxiety, headaches, nausea, and mood swings. The degree of the symptoms is based on the dosage, the length of time taken, and those that depend on health.
The withdrawal side effects of Ambien may be severe in certain instances, and they become particularly severe after prolonged use. The use of medical supervision minimizes the risks, and the complications are managed safely.
The withdrawal of Ambien is highly advised to be under medical supervision to be safe and comfortable. Professionals will be able to instruct tapering and deal with symptoms before they become serious.
Supporting someone going through alcohol withdrawal can be a challenging yet incredibly important task. Withdrawal symptoms can be intense, and managing them requires patience, knowledge, and understanding. Whether you are a family member, a close friend, or a colleague of a person struggling with alcohol addiction, you may want to learn how to help them during this difficult time.
In our guide, we will walk you through the basics of alcohol withdrawal, explain the symptoms of this condition, and teach you how to assist your loved one on their journey to recovery. From creating a safe environment for them to knowing when to reach out to medical professionals, there are many ways you can make a difference and be there for the person you care about.
![]()
Alcohol withdrawal is a range of physical and mental symptoms a person may experience after they abruptly stop drinking alcohol or significantly reduce their alcohol consumption after being dependent on alcohol for a long time. This condition may last for several weeks—in most cases, symptoms resolve within five days, but psychological effects may persist.
Withdrawal happens when the brain has to adjust to the absence of alcohol—this substance affects the brain chemistry, so its sudden removal leads to a brain dysfunction. On average, symptoms of alcohol withdrawal start within eight hours after the last drink and peak within three days.
Here are a few ideas you may find useful when helping your loved one manage alcohol withdrawal:
Do you wonder whether alcohol withdrawal can be treated at home or the person you care about needs to be hospitalized? A doctor will be able to evaluate the severity of the withdrawal and prescribe a suitable course of treatment based on the symptoms of the patient.
In case the alcohol dependence of the individual is mild, it may be possible to manage the withdrawal with medication at home. Nonetheless, it is recommended to consult a healthcare provider who can prescribe drugs that will alleviate the symptoms of withdrawal—for instance, benzodiazepines are known for their efficacy when it comes to alcohol withdrawal treatment.
![]()
Therapy After Alcohol Withdrawal. Once the acute symptoms of withdrawal have been resolved, it is still important to address the addiction—a therapist will help the patient understand the reasons why they started drinking in the first place and come up with a treatment plan that suits the individual and prevents relapse.
Build a Support Network for the Person Struggling With Addiction. Let your friend know they can rely on you—if you cannot be there for them all the time, make sure they are surrounded by people who care about their well-being. You can also suggest they join a support group in your area—sharing their struggles with people who go through the same thing may be beneficial.
Focus on the Lifestyle of Your Loved One. There are many habits the person can implement to reinforce their recovery—sticking to a healthy diet, exercising, picking up new hobbies, and avoiding people and places that trigger their addiction are some of the things that will help them move on.
Whether you are able to convince your loved one to handle their withdrawal at home or the person requires inpatient treatment in the hospital, the support of addiction recovery professionals will be invaluable. Reach out to Silicon Valley Recovery to learn from the experts!
Our team will be able to guide you and your friend or family member struggling with alcohol addiction—we will develop a personalized treatment plan for our patient and equip them with the skills they need to overcome their dependency and lead a happy, fulfilling life.
Symptoms of alcohol withdrawal range from mild (headaches, nausea, sweating) to severe (hallucinations, seizures, agitation). On average, the symptoms persist for 3-5 days.
The duration of alcohol withdrawal depends on several factors—in most cases, it lasts for less than a week, but some symptoms may persist for a few weeks.
You can assist the person struggling with alcohol addiction by educating them about the dangers of withdrawal, being there to support their efforts, and bringing them to a doctor.
It is possible to treat alcohol withdrawal at home; however, in some cases, this condition may be life-threatening. It is advised to show the patient to a healthcare provider who can prescribe them the necessary medication.
Yes, you should at least consult a medical professional about the condition of your loved one—a doctor will be able to diagnose the patient and either let you treat them at home or admit them to the hospital.
Now that you know how to help someone with alcohol withdrawal, you can be there for your loved one during this challenging time and provide them with the support they need. From recognizing the symptoms of withdrawal to coming up with a long-term recovery plan together with a therapist, your care and encouragement may make all the difference.
At Silicon Valley Recovery, we are prepared to assist you and your loved one on this journey. Do not hesitate to contact us—our experienced professionals will be able to advise you, respond to your concerns, and treat your friend or family member either at home or in the hospital.
“`
Recognizing the signs that someone might be taking methadone can be a crucial step in offering them the support and care they might need. Methadone is a medication often prescribed to help with opioid addiction, but like any drug, it can have side effects and consequences for a person’s health and behavior. If you suspect a friend or a loved one is struggling with methadone use, our guide will help you understand the symptoms of methadone consumption and its impact.
Our comprehensive guide on how to tell if someone is on methadone will assist you in spotting the physical symptoms of methadone use as well as the changes in a person’s behavior and lifestyle this medication may cause. We will also explain the purpose of methadone prescriptions and give you advice on supporting someone who is on methadone—from having a compassionate private conversation to involving medical professionals in their treatment.
![]()
Methadone is a medication that is used to treat individuals who struggle with addiction to opioids—it changes the way the brain and nervous system respond to pain, which makes it similar to drugs such as heroin or morphine. In addition, methadone may be prescribed to a patient who suffers from severe chronic pain, especially if other medications have failed to help them.
Developed in the last century, methadone is on the World Health Organization’s List of Essential Medications and remains one of the most popular drugs to manage opioid dependence. This medication reduces drug cravings and eases withdrawal symptoms, making it easier for the patient to stick to their recovery journey.
There are two main reasons to prescribe methadone to the patient: pain relief and opioid addiction treatment. This synthetic analgesic drug can be given to the person who is struggling with post-surgical pain or chronic pain that disrupts their daily life as well as the individual that requires assistance with substance abuse treatment.
While methadone can be efficient to address opioid dependence, it is important to remember that this medication should only be taken under the supervision of a healthcare provider. The administration of methadone comes with certain risks—for instance, a patient may develop a dependence on this drug, especially if they were taking it to treat their addiction to heroin or oxycodone.
Here are the most common physical signs of methadone consumption you may notice:
● Drowsiness. Similar to other sedatives, methadone may make the person feel sleepy—they can have trouble staying awake and alert during the day and appear lethargic.
● Nausea. Your loved one looks pale and complains about feeling unwell—it is possible they are taking methadone or another drug they are allergic to.
● Slow Breathing. If you can tell the person’s breathing is unusually slow and their movements are uncoordinated, they may be experiencing a methadone overdose, which means they will require immediate medical assistance.
Methadone use may affect the behavior of the individual—below you can see the changes to watch out for:
● Confusion. Is your friend having trouble focusing on a simple task? Are they struggling to remember things that happened recently? Methadone consumption may lead to cognitive impairment.
● Poor Concentration. Someone on methadone may not be able to pay attention to what is going on around them—this can be especially dangerous if they are driving a car or operating machinery.
● Mood Swings. Methadone impacts the brain function of the person—this can mean elevated or depressed mood, agitation, irritation, and euphoria.
![]()
Whether your family member or a friend was prescribed methadone by their doctor or started taking it without a prescription, they will benefit from the support of their loved ones. Pay attention to the symptoms listed above, talk to the person you are worried about, and advise them to see a doctor to adjust or discontinue their methadone treatment.
If you believe methadone use negatively affected the physical and mental health of the person you care about, you can reach out to a mental health professional or an addiction specialist and ask your friend to join you in a therapy session. A qualified therapist will be able to diagnose the issue and come up with a personalized treatment plan for the patient.
Methadone is a medication used to treat chronic pain and assist patients who suffer from opioid dependence—it minimizes withdrawal symptoms and has a calming effect on the person.
The most common adverse effects of methadone are dizziness, drowsiness, nausea, vomiting, and muscle pain. In case the methadone overdose is suspected—for example, the person has trouble breathing and passes out—you should call the emergency services.
It is possible to recognize the signs of methadone use upon close observation—from the changes in the person’s behavior, such as confusion and agitation, to the physical symptoms, like sleepiness and lack of coordination.
When it is taken as prescribed by the doctor, methadone can be good for the patient; nevertheless, you should be aware of its side effects and make sure the person stops taking it if it harms their health.
If a person close to you is taking methadone, whether they have a prescription or not, you can be there for them to talk. Talk to them about your concerns and bring them to a healthcare provider who will be able to help them.
We hope that our guide was useful and you learned how to tell if someone is on methadone—both the physical symptoms and behavioral changes associated with this drug may mean your loved one is in trouble. While methadone can be beneficial for the treatment of opioid addiction, its use should be carefully monitored.
Are you looking for advice and support for someone on methadone? Reach out to Silicon Valley Recovery! Our team is a phone call away—we will be able to guide you, listen to your concerns, and come up with a treatment plan tailored to the needs of your friend or family member. Do not hesitate to contact us!
Heroin chic is a phrase, popularized in the early 1990s, that has recently experienced a revival in the fashion industry. It was an objectionable style that gained popularity on the runways and in fashion magazines, featuring waif-like models of the period, a trend that has been revived today. Although it is controversially associated with unhealthy body ideals, the revival of heroin chic is more multifaceted, with 90s fashion reinterpreted in a new context. This article discusses the brilliance of this edgy style, how it has evolved, and how it is shaping current trends, while speculating on its effects on body image and mental health.
Heroin chic, with its pale complexion, thin models, and grunge-inspired style, reappeared in the past decade. This renaissance is not purely a fashion phenomenon; it reflects the cyclical nature of modern culture, where old trends are revisited in new forms. While the look is associated with the dark appeal of the 90s, its recent revival has sparked discussions about the evolving notion of beauty.
Heroin chic was embodied by 90s supermodels such as Kate Moss and Naomi Campbell. They were small and frail, and this became the standard for high fashion. These models featured the grunge fashion movement, which was disheveled in hair, makeup, and clothing which was intentionally torn. Their appearance on the runway and on the adverts had an unforgettable impact on the fashion industry and heroin chic became a big aesthetic. The designers are going back to these styles today to aim at a feeling of nostalgia but at the same time, reinventing the aesthetic to align with current preferences.
The waif appearance is one of the hallmark characteristics of heroin chic. This look referred to models who were extremely thin, to the point of being emaciated, with a delicate and ethereal air. Heroin chic was closely linked to the waif look in the 90s, and despite ongoing body image controversies, the look continues to influence the current fashion industry.
The thin models with their prominent cheekbones and sallow skin tones became the inspiration for new fashion designers seeking to create an edgy, raw style. The waif look challenged the conventional beauty standards, which placed voluptuous or muscular bodies, and instead underlined vulnerability and a non-traditional form of beauty. This thin androgynous ideal is still present in modern fashion promotions, although fashion is becoming increasingly more diverse and accepting of bodies. The 90s thin models contributed to the creation of a new kind of beauty that continues to captivate both designers and audiences.
The 90s were also about thinness but it also adopted an androgynous approach that was not strict on either masculine or feminine. This trend in fashion put gender-neutral clothing into focus, as opposed to the gendered fashion of the past decades.

The 90s heroin chic was closely tied to grunge fashion, which was a rebellion against societal norms. Oversized flannel shirts, leather jackets, and combat boots, which could be worn by any person, not necessarily of any particular gender, were the androgynous style that was usually related to grunge. The trend denounced the old ideas of gender roles and paved the way to a more accepting, and loose way of dressing. The influence of the 90s grunge fashion is also seen today in the grunge-style wear in the streets and in the gender-neutral collections.
Minimalist fashion was a defining element of the 90s aesthetic, focusing on simplicity and functionality. Below is a table that highlights the key characteristics, cultural impact, and ongoing influence of this iconic fashion trend:
| Feature | 90s Minimalist Fashion |
| Key Characteristics | Simple, clean lines, neutral colors, understated designs |
| Cultural Impact | Reflects a shift towards simplicity and functionality, rejecting excess |
| Influential Designers | Calvin Klein, Jil Sander, Helmut Lang |
| Iconic Trends | Slip dresses, tailored suits, basic tees, black and white palette |
| Contrasts with the Previous Decade | A departure from the extravagant, bold fashion of the 80s |
| Current Influence | Inspires modern minimalist styles in both streetwear and high fashion |
The minimalist, waif-like style gave rise to pale skin, which was an attribute of heroin chic. Along with the fact that pale skin was viewed as a symbol of vulnerability, it was also an intentional contrast with the tan, muscular body images of the preceding decades. This style of appearance was taken up by models like Kate Moss in the 90s, and this aspect contributed a lot to the cool minimalistic spirit of the 90s. Nowadays, a pale color of the skin is a characteristic of some fashion subcultures like goth and minimalist fashion.
The influence of heroin chic is still visible in today’s fashion collections, which embrace the simplicity and rawness of the 90s. Designers are returning to past trends but putting a modern twist on them that aligns with current values. Nonetheless, these trends are reemerging, and in this case, the focus has changed to a more inclusive approach towards the body type, where numerous brands prefer to use models of all sizes. This new form of heroin chic is more inclusive and a little less controversial and is a compromise between nostalgia and beauty standards.
Mental health and body image can be greatly impacted by fashion and trends, especially by such an idea as heroin chic. We know that societal pressure and beauty ideals can influence self-esteem and psychological health at Silicon Valley Recovery. However, in case you or a person close to you has problems with body image or are addicted to fashion trends, help is available.
Contact Silicon Valley Recovery to get help today.

Supermodels of the 90s, such as Kate Moss and Naomi Campbell, made the trend of grunge fashion popular with their thin, androgynous look. Their influence created a shift toward a more natural and minimalistic appearance.
The waif appearance is also a thin delicate one with or without a pale complexion. Such a look was coupled with the little makeup, which contributed to the coolness of the era.
The 90s androgynous style furthered the trend of gender-neutral fashion by adopting clothes that were not strictly masculine or feminine, promoting equality in fashion.
Minimalist fashion in the 90s focused on understated designs, neutral colors, and clean lines. It avoided excessive embellishments, in contrast to the bold styles of previous decades.
Some of the heroin chic style highlighted the use of pale skin, which represented vulnerability and simplicity. This beauty was unlike the tanned and fit body images of the past decades.
Meloxicam is one of the most common medicines that can be prescribed and can be classified as NSAIDS. To better understand its classification, usage, and important information, a table is presented below:
| Feature | Meloxicam |
| Drug Class | Nonsteroidal Anti-inflammatory Drug (NSAID) |
| Primary Use | Pain relief, inflammation reduction, arthritis treatment |
| Mechanism of Action | Inhibits cyclooxygenase (COX) enzymes, reducing prostaglandin production |
| Common Side Effects | Stomach upset, dizziness, headache, nausea |
| Risk Factors | May increase risk of heart attack or stroke with long-term use |
| Typical Dosage | 7.5 mg to 15 mg once daily |
| Duration of Use | Short-term for acute pain; long-term for chronic conditions like arthritis |
Meloxicam is not an opioid. Meloxicam does not excite the brain and the central nervous system, as opposed to opioids, which prevent the occurrence of inflammation in the body. It operates by inhibiting pain-inducing enzymes, which causes inflammation and pain – so, it is a non-opioid analog that can be used in the treatment of pain. Opioids used to treat more severe pain include oxycodone or morphine, and are used to treat moderate pain, which happens during arthritis, and include meloxicam.
Meloxicam is an anti-inflammatory that is also a nonsteroidal anti-inflammatory drug (NSAID) and an anti-inflammatory drug that prevents the body from producing inflammatory and painful chemicals of production by blocking body enzymes known as cyclooxygenase (COX). Its lack of any direct or indirect impact on the central nervous system, unlike opioids, makes it an addictive drug, and it cannot be dependent.
There are non-steroidal anti-inflammatory drugs such as meloxicam which is renowned in the management of mild and moderate pains. They have been used as pain relievers to curb inflammation that has the potential to alleviate the pain of conditions like arthritis and muscle tension, among other inflammatory diseases.
The mechanism of action of NSAIDs is to block the activity of the COX enzymes (COX-1 and COX-2) that cause the production of the prostaglandins, pain-causing chemicals. NSAIDs inhibit the ability of these enzymes to reduce swelling, stiffness and pain. That is why the prescription of meloxicam and other NSAIDs will be a routine procedure in the case of arthritis, including rheumatoid arthritis or osteoarthritis, where the inflammation can be regarded as a major issue.
Opioids were the initial choice of medication and they are the ones that are administered when treating acute pain. Nonetheless, due to the increasing number of opioid-related addictions and overdoses, medical workers are thinking about effective opioid alternatives in order to treat pain.
Non-opioid prescription drugs, in particular, the use of meloxicam, offer a safer alternative to opioids in controlling pain. Since opioids have the effect of directly altering brain activity and inhibiting the transmission of pain, NSAIDs, e.g., meloxicam, inhibit the inflammatory process, and the organism should be expected to heal on its own.
Instead, the opioids are more efficient and may be utilized in extreme pain states, but they are more likely to be abused and addicted. To a large number of individuals, NSAIDS like meloxicam may make a good pain reliever and could be administered without the danger of taking opioids.
Arthritis is an illness that is associated with inflammation of the joints, which may lead to pain, swelling, and joint stiffness. Meloxicam has been primarily applied in the treatment of arthritis, because it has the potential of reducing inflammation and pain. Although NSAIDs such as meloxicam have proven effective in the management of symptoms of arthritis, some of the dangers may be achieved after long-term administration of the medication, and they include:
The purpose of this is to ensure that the safety and efficacy of meloxicam achieve their goals in the long term with the help of a medical practitioner. Regular check-ups may be recommended, especially for individuals with multiple underlying health conditions.
Even though NSAIDs like meloxicam are effective, they are not risk-free. When used or abused to excess, it can lead to some kind of complication, and more so in individuals who already suffer some sort of health complication, such as heart disease or kidney complications.
NSAIDs also have specific potential side effects:
New NSAID therapies may be developed in the future to minimize such side effects. Currently, research is focused on specialized delivery systems that would make NSAIDs more effective, besides causing fewer gastrointestinal complications. Innovative approaches to pain management are the direction to provide safer alternatives to individuals who need to take pain relief over the long term without the risks of opioids.
At Silicon Valley Recovery, we help people manage the pain and minimize the risks of addiction. We offer personalized care to individuals who desire to treat their pain with meloxicam in a non-opioid way. If you need guidance on managing pain or other treatment options, you can always contact Silicon Valley Recovery for assistance.

NSAIDs provide effective pain relief and reduce inflammation without causing physical dependence or addiction, unlike opioids; they also carry a lower risk of respiratory depression and overdose, making them safer for long-term use in appropriate patients.
NSAIDs inhibit COX enzymes to decrease prostaglandin production, thereby reducing joint inflammation, swelling, and pain in arthritis; this anti-inflammatory action improves mobility and function while addressing the underlying inflammatory process rather than just masking symptoms.
Yes, non-opioid options include antidepressants like duloxetine for neuropathic pain, anticonvulsants such as gabapentin or pregabalin for nerve-related pain, and muscle relaxants like cyclobenzaprine, all of which can effectively manage chronic pain without the risks of opioid dependence.
Long-term NSAID use can cause gastrointestinal ulcers, bleeding, kidney damage, and increased cardiovascular risks; regular monitoring, use of proton pump inhibitors, and selecting COX-2 selective agents when appropriate can help mitigate these risks.
NSAIDs serve as a cornerstone for inflammatory pain within a multimodal plan that combines physical therapy, acetaminophen, topical treatments, and non-pharmacological interventions like exercise and cognitive-behavioral therapy to optimize pain control while minimizing reliance on any single agent.
The frotteuristic disorder is one type of paraphilic disorder where the individual finds sexual gratification by rubbing themselves against strangers most of the time in open areas. This is usually carried out without the consent of the victim, which may make their spirits feel violated. Individuals who have this disorder are capable of unwanted intimacy, and the intimacy itself is also harmful to both partners. Frotteurism, its nature, and its effects on its victims need to be understood so that they can be helped and provided with sufficient support.
The paper will touch on the problem of frotteurism, including the key characteristics of frotteurism, the occurrence of non-consensual touching, its connection with other paraphilic disorders, the situational conditions under which sexual arousal occurs, and how Silicon Valley Recovery will be beneficial. We will also include frequently asked questions, which will help you develop a deeper understanding of this disorder and its effects.
Frotteuristic Disorder is a medical condition that can be challenging to comprehend due to its unique aspects and characteristics. The frotteuristic disorder is characterized by a tendency of non-consensuality, so that a person receives sexual gratification when rubbing against strangers in public places. This act is classified as a paraphilic disorder, that is, sexual arousal to unusual objects or activities.
Frotteurism can be practiced in busy or public places where the person can rub themselves against unsuspecting victims. The victim may not be aware that the behavior is occurring immediately, or may be confused, embarrassed, or both. Frotteurism is an unethical and illegal practice because of the absence of consent and disregard for personal boundaries. The essential features of the frotteuristic disorder are:

Patients suffering from frotteuristic disorder are likely to be affected by the repetitive nature of the behavior, which may be troublesome unless dealt with. In case of treating this disorder, there is a need to detect the behaviors that are associated with this disorder so that I can step in and provide the necessary support.
Non-consensual touching is a significant aspect of frotteuristic disorder. Being in unwanted contact may be very traumatizing to the victim. In many cases, victims of frotteuristic behavior are attacked in social places. In such settings, the victim may be unable to respond immediately or take any action to stop the attack.
Some of the experiences are as follows:
This can be attributed to the fact that, by valuing the impacts of non-consensual touching, the emotional and psychological cost of such touching to the victims will be easier to deal with. The support of both the victims and those with the disorder must be done comprehensively.
Frotteuristic disorder is classified as a subcategory within the paraphilic disorders, or abnormal sexual desires or behaviors that are not accepted in society. Paraphilias commonly result in activities that can result in injuries to other people, whether physically or emotionally, in an attempt to achieve sexual fulfillment.
The following table brings out the relation between frotteurism and other paraphilias:
| Paraphilia | Connection to Frotteurism |
| Exhibitionism | Both involve non-consensual sexual behavior in public. |
| Voyeurism | Both seek sexual arousal from non-consensual interactions. |
| Sexual Masochism | Both involve behaviors that cross social boundaries. |
| Sexual Sadism | Both involve violating personal boundaries for arousal. |
| Pedophilia | Both involve illegal and harmful sexual behavior. |
| Urophilia | Both are categorized as non-normative sexual arousals. |
The second impact of situational contexts on sexual arousal is the interaction between the situation and sex drive that can be positive or negative. Frotteuristic acts are typically precipitated within a congested or social setting, where the perpetrator can blend in with others. The frotteurism can provide the individual with frotteurism with a sexual stimulus due to the frictional action with strangers in a crowded space.
Frotteuristic behavior can occur in public transportation, at concerts, or in shopping malls, where large crowds of people are present. The victim may also be left in a confusing or uncomfortable state, as the person may be able to do so without the victim’s knowledge.
This is also against the law and not just a breach of personal space. The anonymity that promotes such acts is provided in public places. Frotteuristic disorder can make individuals fail to contain their impulses, and the behavior can even increase without treatment.
Frotteuristic disorder cannot be treated without a multidimensional strategy, which involves therapy, support, and continuous treatment. Silicon Valley Recovery provides expert services to individuals with frotteuristic and other paraphilic disorders. When the proper intervention is administered, affected individuals can be taught how to manage their impulses in healthier ways and minimize the potential for engaging in harmful behavior.
Silicon Valley Recovery provides full assistance using specific programs:
In case you or someone you know has frotteuristic disorder, contact Silicon Valley Recovery and receive professional help and advice. They are committed to providing the necessary tools for a successful recovery.

Frotteurism is the sexual arousal received through rubbing against strangers in a location without their consent. This is non-consensual behavior that is intrusive.
A typical sexual desires are known as a paraphilic disorder, such as frotteurism. These conditions tend to result in destructive habits that cross boundaries of people to gratify themselves.
Frotteuristic disorder provokes sexual arousal in people and, as a result, inappropriate and unwanted contact in social places.
Frotteuristic behavior is prevalent in congested areas, including buses or concerts, where the affected person can rub against strangers without their noticing to give them sexual arousal.
Frotteurism is harmful to the victims and has an effect of emotional trauma and distress. Its treatment can be done by using therapy, counseling, and support to overcome the psychological problems that are present.
In the case of Negative Affectivity, what needs to be addressed are the shadows that prevent recurrence and adverse effects, which may impair the establishment of good relationships with other individuals. Negative affectivity is a broad trait that significantly impacts a person’s emotional status. It is often manifested in a habit of feeling bad habitually, such as anxiety, irritability, ups and downs in mood, and pessimism.
Highly negative affective people have more problems in coping with emotional instability, stress, and even depression, which is a mental condition. This paper examines the correlation between negative affectivity and its impact on mental health, as well as strategies for managing negative affectivity. Silicon Valley Recovery is a place where you can receive support for coping with these problems and become more emotionally stable, leading to a better mental state.
Negative affectivity (NA) refers to the tendency to both express and experience a range of diverse negative feelings. These emotions may be the pressure, the anxiety, the depression, and the annoyance. People who are said to have large doses of NA are more likely to experience emotional distress and respond to daily situations in such a manner that they tend to have negative impressions. This is a fatal emotional condition to mental health since it affects the way an individual perceives inter-relationship, work-related stress, and adversities in life.
Emotional instability is closely related to negative affectivity. Active mood changes and higher levels of emotions may become a problem for maintaining a stable mental condition. These issues of mental health, such as anxiety, depression, and stress, may be due to such instability. Indicatively, living with feelings of worry or pessimism every day can prevent a person from appreciating the small things in life. This emotional suffering can have a lasting impact on one’s ability to function in life, whether at work or in personal life.
The Impact of Stress on Emotional Well-being
Stress is one of the vital dimensions of negative affectivity and an essential manifestation of emotional health. It is hard to control the feelings in the state of extreme stress, and it is hard to keep the balance. The chain of negative consequences that might be triggered by constant stress includes irritability, anxiety, and mood swings.
The stress may be chronic and therefore manifest in different ways. This may be physically manifested, with the person experiencing headaches, fatigue, and muscle tension, or emotionally, with the person being overly worried, irritated, and overwhelmed. The symptoms at such a young age will assist people in making the required actions that they have to undertake to overcome stress and handle emotional instability.

Anxiety and depression are two of the most common mental illnesses associated with negative affectivity. Individuals with elevated negative emotional rates are more susceptible to cultivating it, and they often have co-morbid conditions. Depression can intensify pessimism, and endless worry and anxiety may be caused by the depression.
Anxiety and depression are similar, which is one of the main characteristics of negative affectivity. The similarity between the conditions lies in their shared symptoms, including irritability, emotional instability, and excessive worry. The individuals who experience high rates of negative affectivity and are subject to such mental illnesses may be more vulnerable to stress due to negative affectivity. The sense of helplessness can be confirmed by this type of anxiety and depression cycle, but it is more challenging to interrupt the chain of emotional anguish.
Mood swings and irritability are characteristic of negative affectivity. These emotional shifts can significantly impact a person’s daily routine, affecting relationships, work performance, and overall well-being. Low and high mood individuals may often lack consistency in their reaction to life stressors. At one point, they are fine, and at another, they may either be engulfed or furious.
Among people with negative affectivity, some of the reasons in which individuals may experience mood swings and irritation include:
Through the assistance of triggers, it is possible to discover the techniques of emotional responses and improve one’s well-being.
Here’s a more concise version of the table under the Overcoming Pessimism and Worry heading:
| Strategy | Impact on Emotional Health |
| Mindfulness Meditation | Reduces worry, promotes calmness. |
| Cognitive-Behavioral Therapy (CBT) | Replaces negative thoughts with positive ones. |
| Gratitude Journaling | Shifts focus to positive thoughts, improves mood. |
| Positive Affirmations | Challenges negative self-talk, boosts confidence. |
| Physical Exercise | Reduces stress, boosts mood. |
| Breathing Exercises | Relaxes the nervous system and reduces worry. |
| Social Support | Provides emotional reassurance and reduces isolation. |
At Silicon Valley Recovery, individuals with negative affectivity will receive the required assistance in regaining emotional stability. The firm offers tailored treatment interventions that can assist them to cope with stress, anxiety, and other mental health challenges they experience regarding negative affectivity.
Silicon Valley Recovery strives to offer a holistic approach, which combines therapy, support groups, and lifestyle changes as a solution to maintaining a healthy lifestyle and a healthy mind. In case you or a friend is experiencing emotional instability or any other mental health-related problems, then contact Silicon Valley Recovery and get help today.

The result of the emotional instability can be increased difficulty in coping with stress and triggers, resulting in anxiety, which causes depression in the end. Depression and elevation are not stable, which means that a person is prone to mental diseases.
Sleep deprivation, stress, and unresolved conflicts are some of the examples of triggers. They may lead to relationship disruptions, impact work performance, and affect emotional well-being.
Pessimism is a mindset akin to it, and as such, it augments emotional instability. It is a cause of gloom and discouragement, which can have a highly influential impact on psychological well-being.
Worry can be managed through three effective methods: mindfulness, cognitive-behavioral therapy, and journaling. Such methods help channel negative thoughts into positive ones.
Anxiety and stress are both causes of emotional instability and swings. The stress is constant and therefore enhances the amount of anxiety that subsequently results in the emotional ups and downs and poor management of moods.
Ganser syndrome is a rare and complicated mental disorder that usually leaves victims and medical professionals with puzzling symptoms that imitate other forms of mental illnesses, and this makes it extremely hard to diagnose and treat. Although it is not quite prevalent, the information regarding the Ganser syndrome should be vital to individuals in mental facilities, especially those handling diseases that are characterized by loss of conscience and unconscious motivation.
This paper will discuss the intricacies of Ganser syndrome and compare it with related disorders, including factitious disorder and malingering. We will also explore the world of altered consciousness and unconscious motives in this context, and provide a summary of diagnosis and treatment. At Silicon Valley Recovery, we understand the unique challenges associated with such disorders and are committed to helping people through individualized mental health care.
Ganser syndrome is a type of dissociative disorder, in which one presents symptoms of other psychiatric conditions, which are schizophrenia, yet lacks the underlying causes of such conditions. It is characterized by a phenomenon referred to as vorbeireden, wherein patients tend to provide rough or wrong responses to questions, yet they seem to comprehend the same. Although the disease has been regarded as a rare one, its symptoms are not well understood or diagnosed very well.
Dissociative disorders such as Ganser syndrome develop when the identity of an individual is disassociated with his thoughts, memories, and identity. Such disorders may occur in various forms and be caused by a variety of factors.
The most frequent symptoms of dissociative disorders are:
| Symptom | Challenges |
| Fatigue | Can be caused by many conditions like anemia or depression. |
| Chest Pain | May indicate heart, gastrointestinal, or muscle issues. |
| Shortness of Breath | Can result from heart, lung, or anxiety problems. |
| Headaches | Caused by migraines, tension, or neurological issues. |
| Joint Pain | Often linked to arthritis, infections, or autoimmune diseases. |
| Abdominal Pain | Can be related to digestive or other organ problems. |
| Nausea/Vomiting | May be caused by infections, gastrointestinal issues, or toxins. |
| Fever | Typically due to infections, autoimmune disorders, or cancer. |
| Dizziness | Can result from heart, neurological, or ear problems. |
| Cough | May indicate respiratory issues or heart problems. |
Both factitious disorder and malingering are connected with the intentional generation of symptoms, although they are different in the underlying motives.
Knowledge of these disorders is essential in differentiating them from Ganser syndrome, in which people might seem to generate symptoms without necessarily being aware of them as part of a defense mechanism against stress or trauma in an unconscious way.

Disturbed states of consciousness are the major feature of Ganser syndrome and most dissociative conditions. Individuals with this condition are likely to have behaviors that are most likely to imply confusion or a complete lack of attachment to reality.
The connection between distorted consciousness and unconscious intentions is crucial in understanding the behavior of individuals with Ganser syndrome and distinguishing it from other conditions, such as factitious disorder or malingering.
Ganser syndrome is diagnosed by means of a thorough psychiatric examination. This includes:

Cognitive behavioral therapy (CBT) can also be used to help individuals overcome distorted thoughts and emotional triggers. In some cases, prescription of medication can be taken to assist in the symptoms such as anxiety, depression, or psychosis, depending on its severity.
In Silicon Valley Recovery, we are the center of treatment for people with such complicated mental illnesses as the Ganser syndrome and other dissociative disorders. Our professionals offer individual care with the emphasis on:
Silicon Valley Recovery provides care to individuals with Ganser syndrome or in need of Ganser syndrome-related care by offering compassionate care to meet your needs. Contact Silicon Valley Recovery now and find out more about our assistance.
Factitious disorder is a deliberate generation of symptoms to receive emotional gratification, whereas malingering is motivated by extrinsic factors, such as evading work or being caught by the law.
Distracted consciousness can be characterized by confusion, lapses in memory, or the state of detachment when people cannot perceive reality or the world around them.
The unconscious motives apply to Ganser syndrome and factitious disorder when patients inadvertently generate the symptoms to solve emotional trauma or stress.
A mental assessment is used to exclude other conditions, leading to accurate diagnosis and treatment, particularly for complex disorders like Ganser syndrome.
The treatment consists of psychotherapy, medication for underlying symptoms, and long-term support to overcome emotional triggers and enhance overall mental health.
Depressive Personality Disorder (DPD) is a complex mental issue that involves the manner in which one thinks or feels and behaves. It is also wrongly diagnosed as it has mild symptoms, which are difficult to distinguish from other mood disorders. Depressive Personality Disorder is a critical area of expertise that one needs to provide help and treatment to the victims. In this paper, the authors examine different implications of DPD, such as its effects on emotional health, relationships, and everyday operations.
Depressive Personality Disorder is a disorder characterized by sadness, hopelessness, and a bad attitude towards life. DPD is also more established and is more consistent like a person when compared to clinical, which is episodic. It remains to be emotionally unstable, and this can lead to other mental disorders such as anxiety and depression.

Some of the common characteristics of individuals with depressive personality disorder are constant depression, negative thoughts, and low self-esteem. These symptoms can make them fail to lead an active life and form any meaningful relationships with other people.
The long depression and disappointment of emotions can be described in the form of powerlessness, lack of interest in everyday life, and emptiness. Patients undergo mood fluctuations, irritability, and emotional numbness. These emotional problems are quite debilitating to their physical and psychological well-being, hence the failure to live normal lives.
The effect on self-esteem is also another key effect of Depressive Personality Disorder. This long-term sadness destroys the self-esteem of an individual, resulting in a worthless and skeptical person.
It is emotional distress that generally causes low self-esteem. When one is always in a depressive state, they might feel unworthy of loving or being able to achieve anything. This may manifest in various aspects of life, such as:
This is a vicious cycle that may cause severe loneliness, which may not be overcome by individuals who are in a depressive condition.
One of the common characteristics of the Depressive Personality Disorder is Pessimism. DPD patients are therefore interested in the bad things in life and hardly perceive the good things. This kind of attitude may also complicate their pursuit of happiness or pleasure.
It may either increase or decrease motivation depending on the way the individual is influenced. Negative thought patterns contribute to feelings of helplessness and lack of motivation. For example:
These patterns affect many areas of life, such as work and relationships, and can lead to a sense of hopelessness.
The other character trait of depression that defines depressive personality disorder is social withdrawal. DPD individuals are not inclined to identify themselves with other people, and this can contribute to the loneliness and depression that they experience even more.
Emotional vulnerability can interfere with healthy relationships for individuals with DPD. These individuals may:
Such problems in relationships can lead to difficulty for people in forming a strong bond and in maintaining a satisfactory relationship with family, friends, and colleagues.
These are some of the best methods that can be used to help people cope with depressive personality disorder and enhance their emotional status:
| Strategy | Description |
| Cognitive Behavioral Therapy | A therapeutic approach that helps individuals identify and change negative thinking patterns. |
| Medication | Antidepressants or mood stabilizers can be prescribed to help manage emotional fluctuations. |
| Mindfulness and Meditation | Techniques that promote mental clarity and emotional regulation by focusing on the present moment. |
| Exercise | Regular physical activity boosts mood and reduces stress. |
| Social Support | Building a support network through family, friends, or support groups to aid in emotional recovery. |
| Lifestyle Changes | Healthy eating, sleep routines, and stress management practices to improve overall well-being. |
At Silicon Valley Recovery, we specialize in treating Depressive Personality Disorder. We have a team of mental health professionals who are passionate about the development of individualized treatment plans that address the needs of every individual. It could be therapy, medication, a support group, whatever it is, we are here to help you in your mental health process.
We are here to listen and support you if you or someone you know is struggling with Depressive Personality Disorder.
Contact Silicon Valley Recovery for the support you need to achieve long-term emotional health.

Unrelenting sadness destroys the self-esteem of a person and makes him or her feel unworthy to love or to succeed. It is difficult to build and sustain healthy relationships because they think they do not deserve positive relationships based on such a negative mindset.
Managers will have the opportunity to deal with negative thinking and raise their self-esteem with the introduction of cognitive-behavioral therapy (CBT) and the mindfulness mechanisms. Such practices can support the action of breaking the vicious cycle of thinking about pessimism and supporting a more moderate perception of life.
This leads to a person not performing his or her personal responsibilities because even the most basic of tasks appears to be daunting due to a lack of motivation. It also causes social withdrawal that kills relationships and halts personal and professional development.
Emotional sensitivity will cause overreaction towards conflict, and negative thinking will cause distrust and insecurity. Such patterns put issues in healthy relationship maintenance, where partners are likely to feel unheard or not connected.
Social withdrawal occurs in the form of withdrawal, avoidance of social engagements, and a lack of feeling. To cope with this, therapy and good support systems can assist the individuals to regain their confidence as well as re-enter social life.
Elimination disorders can be problematic for both parents and the children. They cite the issues of urinary and defecation control, which could result in frustration and humiliation. The children are the ones who are likely to suffer from the conditions, and most especially in the process of potty training. The caregivers must be aware of the forms of elimination disorders to be able to cope with such issues. This paper will discuss common elimination disorders, their causes, and how to manage them. These disorders may include bedwetting (nocturnal enuresis) or encopresis, but the right approach can lead to successful outcomes. In the case of Silicon Valley Recovery, we provide professional support to the families that are forced to address such problems.
Children primarily experience elimination disorders related to difficulties with bowel control or urination. It has two common disorders such as nocturnal enuresis (bedwetting) and encopresis (soiling). The disorders are also misunderstood and can be a source of emotional stress to the child and his/her parents. While it’s common for children to struggle with using the bathroom, chronic issues may indicate an underlying cause. In order to empty themselves, there could be a cause behind such chronic problems. The key to treating the condition is understanding the causes, monitoring symptoms early, and knowing how to manage them.
Nocturnal enuresis refers to unconscious urine discharge at night, also known as bedwetting. It is one of the problems that usually happens in children who have not mastered the control of their bladder during the night. On the other hand, the involuntary bowel movement leading to the production of the stools is referred to as encopresis and is usually brought about by persistent constipation or even failure to control the bowel movements. The children are the ones who are likely to suffer from the conditions, and most especially in the process of potty training. The caregivers must be aware of the forms of elimination disorders to be able to cope with such issues.
Nocturnal enuresis has to be treated successfully; to achieve this, we need to identify the causes of this enuresis. This condition can be caused by physical and psychological reasons. These are contributory psychological and medical factors.
Besides the medical reasons, emotional stress and anxiety may also cause or increase the rates of bedwetting. Knowing the cause of the condition is necessary to know the most common way of managing nocturnal enuresis.
Bowel accidents are another such problem that is common in young children and is caused by encopresis or chronic constipation. This most times occurs when the children are not willing to use the toilet because of the fear of pain as a result of past experiences. This may lead to constipation and a soiling cycle in the long run.
The physical effects are not the only ones of encopresis. The disorder could cause the child to be ashamed, therefore, evading socialization to the level of being bullied. This can render this situation very emotional and hence challenging. Moreover, children will feel awkward, be in pain, and their self-esteem and they will not be able to engage in normal activities.
Children should be equipped with the right toilet training to prevent incontinence during childhood. The caretakers, especially the parents, must tell the children how to go to the toilet and be supportive and tolerant. Each child is different, and a child may go through the process at a slower rate as compared to other children.

Here are some practical strategies that parents and caregivers can use to support children in overcoming elimination disorders:
It is a slow process of familiarizing oneself with toilets. The children who will require additional help will be those who have problems with urinary incontinence complications or bowel control complications. It can be enhanced through open communication and a positive attitude toward bathroom routines.
The elimination disorders are adequately addressed by the nature of the disorder and its magnitude. Options include:
| Treatment Approach | Description | When It’s Used |
| Behavioral Therapy | Involves structured routines like scheduled bathroom breaks and reward systems. | Effective for managing bedwetting, encopresis, and potty training issues. |
| Medications | Includes medications such as desmopressin (for bedwetting) or stool softeners. | Used when behavioral strategies alone do not provide sufficient results. |
| Counseling | Psychological support for children dealing with stress or emotional issues. | Helpful when emotional distress or anxiety contributes to elimination issues. |
| Parental Guidance & Support | Educates parents on how to manage elimination disorders through patience and consistency. | Essential for helping parents implement effective strategies at home. |
| Dietary Adjustments | Adjustments to diet, such as increasing fiber intake, to aid in bowel control. | Used when constipation is a major factor contributing to encopresis. |
At Silicon Valley Recovery, we understand the stress that elimination disorders can cause for both children and their parents. We have a special group that works with the families and provides a personal approach to addressing the enuresis at night, encopresis, and other elimination issues of pediatrics. If your child is dealing with elimination disorders, reach out to us. Our specialists are here to guide you through the process and provide the support you need.
Contact Silicon Valley Recovery for the assistance and support that you require to develop long-term emotional health.

Poor capacity of the bladder or longer sleeping patterns are medical causes of bedwetting. This could also be a result of psychological strain.
Parents are recommended to visit the bathroom quite often, congratulate the successful use of the toilet, and consult a doctor in case they need it.
The strategies that could be used in toilet training are consistency, patience, and positive reinforcement. It is possible to avoid pressure and give incentives.
Pediatric elimination problems may influence social life, self-esteem, and emotional well-being. The parents will need to provide help, seek professional assistance, and encourage communication.
They require professional help in the event of the continuation of urinary incontinence after the normal age of self-control of their toilets or emotional disturbance.
The withdrawal symptoms of Concerta are likely to arise when the drug Concerta is stopped. These symptoms might be hard to control, yet now that you are aware of the mechanism of their occurrence and are taking appropriate care, you will cross the obstacles. Concerta is a stimulant medication applicable in treating ADHD and is suitable since it increases the brain density of dopamine. Although this is beneficial as far as focus and attention are concerned, abrupt withdrawal will result in a brain imbalance that will cause withdrawal. This guide will assist you in stopping Concerta, which will give you an understanding of the symptoms, the duration, and the way to overcome the withdrawal.
The withdrawal of concerta occurs when the body and the brain become used to the stimulant, and upon abandoning the use of the medication, you have to make a readjustment. Concerta is a drug derived from methylphenidate, which is a stimulant that influences the brain’s dopamine. On withdrawal, the body might become addicted to the drug, and hence withdrawal. The symptoms are different and depend on the duration of drug use, the force of the drug, and the quitting method, whereby you can quit suddenly or slowly.
The Concerta withdrawal can be attributed to the sensitivity of the body and the brain to the stimulant. Concerta raises the dopamine levels, and this boosts the concentration of focus, mood, and energy. The withdrawal symptoms will come as you will suddenly stop using it since your brain will produce less dopamine. This can be physically and emotionally unpleasant to them due to the resulting interference. Concerta may also be withdrawn following long-term use when the body has become used to the drug.
The withdrawal indicators of toncerta have symptoms that one must be aware of so that they can know what is occurring to them. The symptoms are either mild or severe and may impact your physical and emotional well-being. It is preferable to be ready for such challenges and learn how to deal with them.
Insomnia, fatigue, and altered sleep or appetite are some of the common side effects of Concerta withdrawal. On the emotional level, individuals are subjected to irritability, anxiety, depression, and mood swings. The effects occur when the body develops tolerance to the drug being taken, and these might be severe depending on the history of usage.
The Concerta withdrawal plan is individualized to each individual. The withdrawal symptoms, as a rule, start a few hours or days after quitting a drug. Such circumstances can be within days or a few weeks, depending on your personal circumstances.

During the process of Concerta detoxing, the body will get used to not using the stimulant. It is possible to speak about the worst days during the first weeks because, among the symptoms, irritability, sleepiness, and insomnia are also mentioned. The severity of the symptoms is likely to fade out during the process of detox, but mental disorders, such as anxiety or depression, may remain. It does not happen instantly, and you will not wake up feeling okay, although it can be achieved with patience and the help of good support.
Here’s a table outlining safe approaches to Concerta tapering:
| Approach | Description | Benefits | Considerations |
| Gradual Dose Reduction | Slowly decrease the dosage over time to minimize withdrawal symptoms. | Reduces the intensity of withdrawal effects. | Requires close monitoring by a healthcare provider. |
| Alternating Days | Taking Concerta on alternate days to allow the body to adjust. | Eases the body into lower dosages. | It can be challenging for some individuals to manage. |
| Microdosing | Reducing the dose in very small increments over time. | Minimizes abrupt changes in brain chemistry. | Requires precise dosing and guidance from a doctor. |
| Consulting with a Doctor | Regular check-ins with a healthcare professional throughout the tapering process. | Ensures a tailored and safe tapering plan. | Must be consistent in following medical advice. |
The key advantage of this source is that it can supply significant information on the way to safely terminate the use of Concerta to minimize the risks.
These measures will allow reducing the threats and make the withdrawal process easier.
Concerta withdrawal affects both physical and emotional health and requires treatment for both aspects. The psychological symptoms should also be addressed, just like bodily ones, as your body becomes used to living without the drug. Controlling energy and maintaining a regular schedule is also important in the process, as well as rest.
Time also needs to be allocated to take care of your mind. Discover some activities that are relaxing, like meditation, deep breathing exercises, or journaling, to overcome anxiety and mood swings. One can create a friend circle, family, or a counselor to make this time less lonely and more comprehending.
We know the problems that have surrounded the withdrawal of Concerta at Silicon Valley Recovery, and we are resolute to help you go through it. The answer concerning the need to help with a Concerta detox or help with tapering on Naltrexone will be found in our team of trained professionals, who are available to help you. We offer compassionate care to enable us to cope with the bodily and mental effects of withdrawal, to recover safely and successfully.
If you or a loved one is experiencing Concerta withdrawal, reach out to Silicon Valley Recovery Center for counseling and guidance as you navigate through the process.
The most common ones include exhaustion, anxiety, and lack of concentration. These symptoms can be managed through tapering and emotional support. A complete withdrawal without being dehydrated and instead feeding on healthy food will relieve the withdrawal pain as well.
Concerta withdrawal symptoms are usually manifested in several days to several weeks. It is anchored on such factors as dosage and duration of use. The symptoms can be cut through by gradually cutting the drug intake, which will cut down the withdrawal.
The detox is safe, and hence one should gradually withdraw the drug, with the assistance of a health professional. It is highly necessary to stay physically and emotionally fit so that the process can be reduced to withdrawal symptoms.
Concerta withdrawal insomnia can be managed by developing an excellent sleeping routine and reducing the use of caffeine. Sleep may also be improved using relaxation techniques, e.,g Deep breathing exercises during withdrawal.
Mindfulness and meditation could help to diminish the degree of anxiety and seek emotional support from loved ones or a counselor. The other method that will facilitate the nature of anxiety, as far as withdrawal is concerned, is progressive withdrawal with professional guidance.
The withdrawal symptoms of Ritalin may occur when a person ceases using Ritalin. The symptoms may be mild, profound, or moderate, and they can be addressed successfully given adequate care and counseling. Ritalin is one of the medications that is used as a treatment for ADHD. It affects the central nervous system and activates the level of dopamine in the brain.
Nevertheless, withdrawal symptoms are several effects that may occur when the drug is suddenly discontinued or incorrectly discontinued. In this article, we will take you through the process and also give tips on how you can easily overcome Ritalin withdrawal, whether you are having the symptoms or when assisting a loved one.
Ritalin detox occurs when the body adapts to the continuous use of the drug. Discontinuing Ritalin may result in a state of withdrawal due to a mismatch of the dopamine and norepinephrine balance. These neurotransmitters play an important role in mood, concentration, and energy control. Once a person becomes addicted to Ritalin has to come to terms with the withdrawal symptoms of the drug.
This may have some withdrawal effects, such as fatigue, irritability, depression, and difficulty in concentration. The National Institutes of Health (NIH) reported that patients with Methylphenidate use disorder have emotional disturbances related to withdrawal with time.
The form of the drug is the peculiarity of the withdrawal of Ritalin. Ritalin or Methylphenidate is a stimulant drug. In contrast to the other medications, stimulants lead to quick alterations in our neurotransmitters. This leads to withdrawal symptoms, which, in most cases, are very severe and may be physical and psychological.
Retinal withdrawal should be taken into consideration since it influences individuals. One should keep in mind that the symptoms are not permanent, and they may be treated using a proper plan.
The stimulant withdrawal symptoms should also be noted to be aware of how the body reacts to the withdrawal of such drugs as Ritalin. Such symptoms can vary, but some symptoms are common, such as fatigue, irritability, and lack of concentration. The body will respond by making people experience mood swings and emotional distress when they are used to a deficiency of the stimulant. These symptoms are a reaction of the body to the sudden withdrawal of the effects of the drug found to have changed the brain chemistry over the years. These symptoms vary in severity, with long-term users experiencing more intense reactions.
Stimulant withdrawal also presents other signs and symptoms such as bleeding, headaches, increased appetite increase and sleeping problems. Others might experience their level of apathy or lack of motivation, a state which is also known as the crash. Being aware of these signs early on can help individuals seek the appropriate care and support during detox. Knowledge of stimulant withdrawal will determine how to easily manage the transition and reduce the inflicted pain.
Ritalin withdrawal is associated with such common side effects as fatigue, irritability, depression, anxiety, and concentration difficulties. People can also feel hungry, have sleeping trouble, and some physical symptoms such as headaches. These are due to bodily adaptation to the intake of the stimulant, and depending on the experience, some of these effects may be less severe.

ADHD drug withdrawal may have many difficulties, both physical and psychological, and it will take time till the body adapts, as the following table summarizes the situation:
| Aspect | Description |
| Brain Chemistry Impact | ADHD drugs, such as Ritalin, have a direct influence on the amount of dopamine and, therefore, the withdrawal symptoms are more significant and harder to overcome. |
| Physical Symptoms | Most of the physical effects of withdrawal are fatigue, irritability, and sleeplessness, as the body adapts to the new reality of not having the medication. |
| Psychological Symptoms | Mood swings, anxiety, and brain fog are also most frequently experienced as the brain cannot quickly settle once again after the medication is discontinued. |
| Withdrawal Duration | The duration of the withdrawal process may differ based on the duration and extent of time the person took the drug, and could take between a few days and even a few weeks. |
Compared to other stimulant withdrawals, ADHD drugs have several factors. Firstly, Ritalin is commonly used in cases of long-term disorders, such as ADHD, and therefore its withdrawal is more complicated. The addiction of the body to the drug can get more ingrained, and the symptoms increase. Besides this, unlike other stimulants like amphetamines, Ritalin interacts with dopamine to cause greater psychological effects like depression or mood swings. These services and encouragement are needed during this phase to avoid relapse.
One of the safest ways of avoiding severe withdrawal symptoms is tapering or gradual reduction of your dose, also referred to as Ritalin tapering. You will find it easier to go through withdrawal from taking Ritalin, as your body will be used to it. This would help in minimizing risks such as anxiety, depression, and intense fatigue.
The following are a few of the guidelines that initiated the Ritalin tapering process:
Tapering of Ritalin can be a very simple process when done in the right manner and with inspiration.
It may prove more difficult to regain in situations involving individuals who got addicted to Ritalin. Ritalin addiction can be treated through therapy, counseling, and lifestyle alteration. The dependent people would, in a majority of cases, need some long-term help to keep them out of the drug Ritalin.
Other important aspects of the recovery process include:
Ritalin addiction is difficult to treat, but with the right approach, recovery is possible.
We know the issues associated with Ritalin withdrawal at Silicon Valley Recovery. Our mission is to support you in patient-centered care during your recovery and detox. Whether you are experiencing withdrawal symptoms from Methylphenidate or struggling with Ritalin addiction, our team is ready to assist you at every step. Ritalin withdrawal is not a reason to wait.
Contact Silicon Valley Recovery and receive the assistance needed to be on the road to recovery.

When discontinuing Ritalin, withdrawal is a result of an alteration in brain chemistry. Symptoms can be dealt with by gradual tapering and professional assistance. Its common symptoms include irritability, fatigue, and lack of concentration. Professional advice would also be useful since it would make the process of transitioning much easier and reduce the possibility of experiencing severe withdrawal symptoms.
Ritalin and other medications for ADHD have a distinct effect on brain chemistry, which usually results in more severe withdrawal symptoms than other stimulants. These drugs directly affect the dopamine levels and, therefore, it is harder to withdraw from these medications.
The tapering of Ritalin can lead to exhaustion, moodiness, and insomnia. These side effects are reduced by a slow withdrawal of the dosage. Water, exercise, and stress relief are also important determinants in alleviating the pain of discontinuing the use of Ritalin.
The interventions that should be used to overcome Ritalin dependency include a powerful support system, regular therapy, and medical advice. Professional assistance will guarantee a more efficient and safer process of overcoming the addiction to Ritalin and will also mean a substantial decrease in the possibilities of relapse.
Medical assistance involves treatment, drug administration, and observation during the withdrawal process to make it easy and safe. Physicians can assist in the modification of doses and symptom management, which will simplify the Methylphenidate withdrawal process and increase the recovery rates.
When it comes to prescription medications for anxiety, sleep disorders, and pain management, confusion often arises between Klonopin and opioids. Both impact the central nervous system, yet they operate fundamentally differently. Patients, caregivers, and even some healthcare providers sometimes ask: “is klonopin an opioid?”
Understanding the differences between these two classes of drugs is essential for safety, effective treatment, and preventing misuse. In this article, we explore Klonopin classification, its uses, side effects, addiction potential, and how it compares to opioids.
The Klonopin classification situates this medication firmly within the benzodiazepine drugs category. Benzodiazepines enhance the activity of gamma-aminobutyric acid (GABA), an inhibitory neurotransmitter in the brain. This results in a calming effect on the nervous system, which helps reduce anxiety, control seizures, and promote sleep.
In contrast, opioids function by binding to opioid receptors in the brain and spinal cord, directly altering pain perception and producing euphoria. Understanding this distinction is crucial because it clarifies that Klonopin is not an opioid, nor is it suitable for treating pain in the same way that opioids are. Its primary action is anxiolytic and sedative rather than analgesic.
Additionally, the pharmacokinetics of Klonopin, how the body absorbs, distributes, metabolizes, and excretes it differ significantly from opioids. Benzodiazepines generally have a longer half-life, which allows them to provide sustained therapeutic effects for anxiety and seizure disorders.
The comparison between Klonopin vs opioids is not merely academic; it has practical implications for patient care, safety, and addiction prevention.
| Feature | Klonopin | Opioids |
| Drug Class | Benzodiazepine drugs | Opioids |
| Primary Use | Anxiety, panic disorders, seizure control | Pain relief |
| Addiction Potential | Moderate if misused | High, especially with prolonged use |
| Mechanism | Enhances GABA neurotransmission | Binds to opioid receptors in brain and spinal cord |
| Sedative Effect | Yes, pronounced | Can occur, often accompanied by euphoria |
| Prescription Regulation | Controlled substance, Schedule IV in the U.S. | Controlled substance, Schedule II in most cases |
This table shows that while both classes affect the central nervous system, their therapeutic goals, mechanisms, and risks differ substantially. For example, Klonopin may sedate patients and reduce anxiety, but it does not relieve acute pain the way opioids do. Conversely, opioids carry a higher risk of euphoria-driven misuse and accidental overdose.
It is worth noting that combining Klonopin and opioids can significantly increase the risk of respiratory depression, coma, and death. This dangerous combination is a major reason why healthcare providers carefully monitor prescriptions when patients require multiple central nervous system depressants.
All medications come with potential adverse effects, and Klonopin side effects are no exception. Though generally safe under medical supervision, prolonged or high-dose use can cause significant issues. Common side effects include:
More serious, but less common, effects include paradoxical reactions like agitation or aggressive behavior, particularly in children and elderly patients. For patients taking Klonopin, monitoring these effects is essential, especially if they have pre-existing medical conditions such as sleep apnea, liver disease, or a history of substance use. Awareness and proactive monitoring can prevent complications and ensure safe therapeutic outcomes.
Klonopin uses extend far beyond treating anxiety. Understanding its diverse applications highlights why this medication cannot be compared directly to opioids:
Unlike opioids, which primarily address physical pain, Klonopin targets the emotional and neurological components of mental health conditions. This distinction underscores the importance of proper medication selection for each condition. For more insights into effective treatments for anxiety and seizure disorders, the American Psychiatric Association (APA) offers evidence-based guidelines.
For those new to prescription medications, differentiating benzodiazepine drugs and opioids is essential for safe usage:
This differentiation also highlights the role of non-opioid medications in treating certain conditions. Patients concerned about opioid misuse can explore safer alternatives like Klonopin for anxiety or seizures, reducing reliance on high-risk pain medications.
Non-opioid medications, including Klonopin, offer several key benefits compared to opioids:
For further insights into non-opioid alternatives and safe prescribing practices, the Centers for Disease Control and Prevention (CDC) provides guidance.
Despite being a non-opioid medication, Klonopin addiction is significant if misused. Physical dependence can occur with extended use, and withdrawal symptoms may include:
The risk of addiction is higher in patients with a personal or family history of substance use disorder. Understanding Klonopin side effects and monitoring usage closely can reduce this risk. Education and responsible prescribing are key to safe outcomes.
Healthcare providers follow strict Klonopin prescription guidelines to minimize risks:

Adhering to these guidelines ensures that patients reap the therapeutic benefits of Klonopin use while minimizing the risk of addiction or severe side effects.
Education is essential for safe medication use. Understanding Klonopin vs opioids empowers patients to make informed choices about their health. At Silicon Valley Recovery, individuals receive guidance on safe prescribing, risk management, and mental health support. For more understanding of benzodiazepine safety and responsible use, consult our experts today!
Klonopin classification is a benzodiazepine drug that targets GABA receptors to reduce anxiety and induce calm. Opioids, in contrast, bind to opioid receptors for pain relief and euphoria.
Klonopin uses focus on anxiety, seizures, and sleep disorders, while opioids primarily manage pain. Effectiveness depends on the condition being treated; using Klonopin for pain would be inappropriate.
Klonopin side effects include drowsiness, impaired coordination, memory issues, dizziness, and rare respiratory depression, especially when combined with other depressants.
It is classified as a benzodiazepine drug because it works on GABA neurotransmission rather than opioid receptors, producing sedative and anxiolytic effects instead of analgesia and euphoria.
Doctors follow Klonopin prescription guidelines – lowest effective dose, short duration, monitoring for dependence, patient education, and avoiding concurrent CNS depressants.
In today’s healthcare landscape, questions about medications and their classifications are more important than ever. With the rising concerns over opioid misuse, many individuals are curious about alternative treatments for pain and mental health conditions. One such medication is Trazodone, often prescribed for depression and sleep disorders. But a common question arises: is trazodone an opioid? Let’s dive deep into its classification, effects, and how it compares to traditional opioids.
Trazodone classification is essential for anyone considering this medication. Despite some misconceptions, Trazodone is not an opioid. Opioids, such as oxycodone, hydrocodone, and morphine, work primarily by binding to opioid receptors in the brain and spinal cord, significantly altering pain perception and producing euphoria. This mechanism is also why opioids have high addiction potential.
Trazodone, on the other hand, belongs to a class of non-opioid medications known as serotonin modulators. It primarily works by increasing serotonin levels in the brain, which helps regulate mood and sleep.
Unlike opioids, it does not target opioid receptors, and its potential for addiction is considerably lower. According to the National Institutes of Health (NIH), Trazodone is classified as an antidepressant medication, specifically a serotonin antagonist and reuptake inhibitor (SARI).
Understanding this distinction is crucial for patients and healthcare providers when discussing treatment options, especially in pain management or mental health care.
While both Trazodone and opioids can influence how a person feels physically and emotionally, their mechanisms and effects are fundamentally different:
| Feature | Trazodone | Opioids |
| Primary Use | Depression, anxiety, and insomnia | Pain management |
| Mechanism | Increases serotonin in the brain | Binds to opioid receptors in the CNS |
| Addiction Risk | Low | High |
| Sedative Effects | Moderate | Often strong, can impair breathing |
| Pain Relief | Limited; indirect | Direct analgesic effect |
| Prescription | Yes, regulated | Yes, tightly controlled |
From the table above, it’s clear that Trazodone and opioids serve different purposes. While opioids are primarily prescribed for severe pain, Trazodone is typically used for mental health and sleep disorders. However, it sometimes helps with pain indirectly by improving sleep quality and reducing stress.
Non-opioid medication options have become increasingly popular in the fight against chronic pain and the opioid crisis. Trazodone offers an alternative that does not carry the same risks of dependency and overdose associated with opioids.
Patients often benefit from knowing that a non-addictive alternative exists, especially when their treatment plan includes mental health considerations alongside pain management. The combination of low addiction potential and therapeutic effects on sleep and mood makes Trazodone a viable option in many scenarios.
While it’s a non-opioid, Trazodone is still a prescription medication. It must be used under medical supervision to avoid potential side effects, such as dizziness, low blood pressure, or, rarely, serotonin syndrome. The FDA provides extensive guidelines on safe prescribing practices for Trazodone.
One of the key benefits of Trazodone lies in its antidepressant properties. As a SARI, it enhances serotonin signaling in the brain, which can:
Interestingly, research shows that depression and chronic pain often occur together. Therefore, medications like Trazodone can indirectly contribute to pain relief alternatives by improving overall mental health, sleep quality, and emotional resilience.
As the opioid epidemic continues to affect millions, exploring non-addictive alternatives is critical. Here are some widely recognized options:
While Trazodone is not a traditional painkiller, its role as a non-opioid medication and mood stabilizer positions it as a safe adjunct in comprehensive pain management plans.
When comparing pain relief alternatives, Trazodone may not replace traditional opioids for acute or severe pain. However, it offers unique advantages:
The Mayo Clinic emphasizes that medications that improve sleep and mood can be supportive pain relief alternatives, especially in chronic conditions.
One of the distinguishing characteristics of Trazodone is its sedative effects. While opioids can induce heavy sedation and respiratory suppression, Trazodone provides a milder calming effect that helps patients relax and sleep better without dangerous side effects.
The sedative properties are dose-dependent, typically stronger at doses used for insomnia than for depression. Many patients report improved sleep onset and quality, which indirectly supports pain management and emotional regulation.
It’s worth noting that, like any prescription drug, Trazodone should not be combined with alcohol or other sedatives without consulting a healthcare provider, as this can increase the risk of excessive drowsiness or falls.
At Silicon Valley Recovery, Trazodone prescription medication guidelines focus on safe and responsible use. Patients are typically started on low doses, which are gradually adjusted to minimize side effects.
Regular monitoring of blood pressure, sleep patterns, and mood is essential. Healthcare providers pay close attention to patients with pre-existing conditions like heart or liver issues to ensure safe dosing. Abrupt discontinuation should be avoided, as it can lead to withdrawal symptoms such as dizziness or agitation.
When used responsibly, Trazodone is a valuable non-opioid alternative for mood regulation, sleep support, and adjunctive pain management. By following proper guidelines and working closely with medical professionals, patients can maximize the medication’s benefits while minimizing potential risks, supporting both mental and physical well-being throughout their recovery journey.
Trazodone is classified as a serotonin antagonist and reuptake inhibitor (SARI), which is a type of antidepressant. Unlike opioids, it does not bind to opioid receptors in the brain or spinal cord, meaning it does not carry the same risk of addiction or respiratory depression.
Yes, Trazodone can serve as a non-addictive alternative in some cases, particularly for chronic pain management. While it does not directly block pain signals like opioids, it can improve sleep quality and stabilize mood, which helps reduce the perception of pain over time.
The sedative effects of Trazodone are generally milder and primarily aimed at improving sleep. In contrast, opioids can cause deep sedation, respiratory suppression, and higher risks of drowsiness-related complications, making Trazodone a safer option for long-term use in many patients.
Trazodone works by increasing serotonin levels in the brain, which helps improve mood, reduce anxiety, and support emotional well-being. These antidepressant effects can indirectly aid pain management, as improved mental health often lowers the perception of chronic pain and enhances overall quality of life.
Yes, when taken under medical supervision, Trazodone is generally considered safe for those seeking non-opioid options. Its low risk of dependency, combined with benefits for sleep and mood, makes it a reliable choice in comprehensive pain management and mental health care plans.
Cocaine may promise euphoria, energy, and confidence, but the crash that follows can be brutal. Among its many mental health consequences, cocaine-induced anxiety is one of the most jarring and distressing. It’s the uneasy tremble beneath the high, the panic that creeps in after the last line fades. Anxiety is not merely a consequence of using cocaine to many people, it is a preoccupying state that haunts people even after the cocaine effects have subsided.
There exists a complex relationship between cocaine and anxiety, a relationship whose roots are in the neurochemical disorder and the emotional rubble that continues to exist even after the afterglow wears off. It may result in users having their hearts racing, being overcome by irrational fears, or even being in the clutches of a full-blown panic.
Cocaine induced anxiety is not some passing concern or some light-headedness. It is sometimes bitter, chaotic, and emotionally stalling. Learning about the relationship between this stimulant and the feeling of anxiety, as well as how to cope with its effects, would be instrumental in the process of breaking the chain of fear, panic, and addiction.
Cocaine-induced anxiety is the uncontrolled fear, restless uneasiness, and emotional distress that a person usually develops during or after using cocaine. It falls under the substance-induced anxiety disorder, an illness that has its causes in the direct symptoms emanating from drug interaction.
The type of anxiety can:
People experiencing stimulant-induced anxiety from cocaine may face:
Cocaine is not only a stimulating drug, but it also takes over the brain. Its high is euphoric, but it costs heavily to one’s sanity. Cocaine gives short-term highs and extensive emotional lows since it triggers neurotransmitters such as dopamine, serotonin, and norepinephrine. In the long run, such chemical pandemonium changes the way the brain functions and may cause permanent mental health problems.
To learn more about the interconnection between cocaine use and mental health, it will be helpful to consider the comparison between common effects:
| Mental Health Effect | How Cocaine Contributes | Short-Term Symptoms | Long-Term Impact |
| Anxiety Disorders | Overstimulates the central nervous system, increases cortisol and adrenaline | Racing thoughts, panic attacks, paranoia | Chronic anxiety, phobias, generalized anxiety disorder (GAD) |
| Depression | Depletes dopamine and serotonin after an initial high | Crash, sadness, emotional withdrawal | Persistent depressive disorder, suicidal thoughts |
| Psychosis / Cocaine Paranoia | High doses and long-term use distort perception and thinking | Delusions, hallucinations, and fear of being watched | Paranoid psychosis, schizophrenia-like symptoms |
| Mood Swings / Bipolar Symptoms | Dopamine spikes followed by crashes mimic manic-depressive cycles | Euphoric highs and irritable lows | Increased risk of bipolar-like behavior |
Cocaine addiction does not always manifest itself physically as seriously as the withdrawal of substances such as opioids or alcohol, but the psychological symptoms are devastating. Whenever a person abstains after a cocaine-intensive phase of usage, the brain, which has lost all of its dopamine and is stimulated to its limits, drags back. This is frequently referred to as the crack, but this may only be a start to the withdrawals, which may extend for a long, long time.
The knowledge that enables one to understand the effects of cocaine withdrawal is needed to encourage awareness and prevent relapses in terminology. Most of these symptoms are confused with different mental problems, such as anxiety and depression.

The typical cocaine withdrawal symptoms include the following:
The prevalence of all anxiety disorders is not related to trauma and stress, and is also genetically determined – direct substances cause some. Substance-induced anxiety disorder is one such diagnosis because the only thing that drives anxiety symptom arousal is a drug or being under the influence of a drug, or withdrawal. One of the most widespread culprits is the use of cocaine.
The condition is similar to other conditions like generalized anxiety or panic disorder, but the causative factors are incomparable. The anxiety may not only occur in the crash, but also when one is not on the cocaine, as the drug affects neurotransmitter systems in the brain.
This is the way that cocaine causes such substance-induced anxiety:
One of the most potent and scary psychological effects of cocaine use is called Paranoia. It insidiously crawls into your mind unnoticed, usually like hyper-awareness, or in other words, edgy caution, and before you know it, you find yourself in the depths of delusional behavior. Paranoia is not a temporary side effect to many users – instead, it is a lasting mental health problem that severely interferes with emotional equilibrium and routine life.
Cocaine paranoia features delirious suspicion of people, fear of being observed, stalked, or injured, and paranoia in general. Paranoia is directly related to overactivating the brain’s dopamine system, in terms of the brain parts involved in the perception of threat.
The most critical indicators of paranoia caused by cocaine are:
Cocaine and panic attacks often go hand in hand, an explosive pairing that can be emotionally and physically overwhelming. The stimulant nature of cocaine spikes heart rate, blood pressure, and sensory input, setting the perfect stage for a panic attack. For users already prone to anxiety, cocaine can act like gasoline on fire.
Recovery isn’t just about quitting a substance – it’s about healing the mind, regaining control, and rediscovering peace. Cocaine-induced anxiety can feel overwhelming, but you don’t have to face it alone. At Silicon Valley Recovery, compassionate, evidence-based treatment is available to help you or your loved one break free from the grip of addiction and anxiety.
Whether you’re struggling with withdrawal, managing persistent panic, or navigating paranoia, our team is here to support your journey every step of the way. With dual diagnosis care, personalized treatment plans, and 24/7 support, we’ll help you rebuild from the inside out.
Contact Silicon Valley Recovery today to speak with a specialist and begin the path to lasting healing.

Overstimulation of the nervous system, especially the wave of dopamine and norepinephrine in the brain, is the result of cocaine-induced anxiety. Restlessness, racing thoughts, paranoia, panic attacks, and intensified fear are the symptoms.
Cocaine has a lot of effects on emotional regulation. When cocaine is used, it manipulates the chemistry of the brain and tends to cause or exacerbate the feeling of anxiety. They may affect instantaneously when in use or over time, leading to the development of chronic anxiety disorders as well as panic attacks.
An important psychological side effect of cocaine is stimulant-induced anxiety when it is used repeatedly or in higher doses. It aggravates stress reactions and may result in generalized anxiety that resembles other health disorders.
Cocaine use results in paranoia; this makes individuals mistrust other people, avoid social networks, and become emotional. It destroys engagement with the world on a mental level, and in the long run, it destroys the sanity of the mind, as any interaction is scary and may be a cause of psychosis.
These tools are cognitive behavioral therapy (CBT), mindfulness, adequate nutrition and rest, and the help of addiction specialists. Severe and long-standing recovery may necessitate dual diagnosis treatment, which includes both mental health and addiction.
When people think of cocaine use, the focus often lands on its psychological and addictive effects. But what does cocaine do to your nose? The truth is that snorting cocaine can cause severe damage to the nasal tissues that silently develops and worsens over time. The consequences can be painful and irreversible, including frequent nosebleeds, nasal congestion, septum perforation, and cartilage damage.
Cocaine constricts the blood vessels in the sensitive nasal tissues, leading to tissue death, sinus infections, and, in the worst cases, a collapsed septum. Medical experts indicate that the effects of chronic intensive use of cocaine are listed as major causes of damage and destruction of nasal tissue, as well as the loss of smell among substance users. In this blog, we are going to have a deeper insight into how cocaine affects the health of your nose, the symptoms you need to be aware of, and how recovery can be made in case some damage has already been done.
Even though snorting cocaine can get you high in a matter of minutes, it equally destroys the nerve-sensitive tissues deep within your nose without your knowledge. Cocaine also shrinks blood vessels, blocking the supply of oxygen and nutrients in the nasal tissues. This sluggish circulation eventually makes the tissue weak, causing inflammation and infections, and even resulting in structural damage. Repeated use only worsens these problems, and in most circumstances, such damage cannot be repaired.
These are some of the most frequent nasal maladies that are triggered by cocaine:
Snorted cocaine and other forms obviously affect the nasal system negatively. The drug constricts blood vessels in the nose, reducing the flow of oxygen‑rich blood to the soft tissues. A lack of appropriate circulation causes the tissues to dry up, crack, and even die, resulting in a wide range of nasal problems. The effects tend to initiate slowly yet become severe in the case of continuous abuse.
Cocaine has some of the most damaging effects on nasal health, including:

Tissue damage from snorting cocaine is among the most severe consequences of the drug. Blood flow is inhibited by cocaine, denying the body tissues of oxygen and nutrients. The result of this is inflammation, scabbing, and eventual erosion of the soft tissue and cartilage hidden within the nose. This may lead to unpleasant and disfiguring problems such as septal perforation and collapse of the nasal bridge with time.
The various stages and types of cocaine-affected smoke-induced nasal damage are described in the table below:
| Type of Damage | Description |
| Nasal Irritation | Redness, burning, and discomfort due to repeated chemical exposure |
| Mucosal Dryness | Dry nasal passages that lead to cracking, itching, and scabbing |
| Tissue Inflammation | Swelling of the nasal lining causes congestion and pain |
| Ulceration | Open sores inside the nose caused by chronic irritation |
| Septal Perforation | A hole in the nasal septum due to erosion of cartilage |
| Nasal Collapse | Breakdown of structural support leading to a sunken or misshapen nose |
| Chronic Sinus Infections | Blocked or damaged tissue increases the risk of frequent infections |
Among the most dangerous complications of the nose, which are provoked by the long-term use of cocaine, is septal perforation. The septum is the thin strip of cartilage that divides both nostrils. The tissue and cartilage may start to die when blood to this region is repeatedly interrupted by cocaine, and this usually causes a hole, or what is also referred to as a perforation.
This situation may cause great discomfort and may result in permanent nasal problems, such as:
Common symptoms of nasal damage among cocaine snorters are frequent nosebleeds. Cocaine also dehydrates the sensitive lining found on the inside of the nostrils and makes the blood vessels used weak and easy to burst. The mucous membranes may be inflamed and damaged even with low doses of the drug when its use is repeated.
This is the reason that when using cocaine, frequent nose bleeds are a common phenomenon:
The other problem that daily users of cocaine experience is nasal congestion. The medication causes irritation and swellyness on the lining of the nose that causes excessive secretion of mucus, which makes one feel blocked constantly. With time, this may create difficulty in breathing through the nose and result in chronic sinus issues.
The following are the major reasons behind congestion in the case of cocaine use:
Among the potentially more devastating long-term consequences of snorting cocaine are the slow-moving, but extraordinarily caustic side effects, known as gradual smell loss as a consequence of cocaine snorting, more commonly referred to in medical circles as anosmia. Cocaine destroys the nose stuffing and the smell-picking-up receptors. By repeatedly using it, your sense of smell might be permanently damaged, with nerve damage being the cause.
This is how cocaine can result in loss of smell:
Nose health complications may also occur during the excessive use of cocaine, or it may include severe conditions such as nosebleeds and nose congestion, as well as nose septum perforation, the loss of smell, and irreversible damage to tissues. Not only are these effects painful, but they may necessitate surgical operations or cause permanent disability. It is essential to know how cocaine affects your nose so that you can notice early signs of destruction and seek assistance on time.
Whether you or a loved one is having a hard time with cocaine consumption or has related complications to the nose, there is help to be found. Contact Silicon Valley Recovery today to begin the journey toward healing and recovery.

Symptoms are repeated nose bleeding, nose stuffiness, crusts, anosmia, and apparent nasal septum soreness or gap. Such symptoms can intensify over time with ongoing use.
Cocaine decreases blood circulation to the tissues of the nose, and this deprives the septum of oxygen. This will gradually cause degeneration of tissue and the formation of a gap in the cartilage between the nostrils.
Cocaine dries up the nasal lining, and this way, weakens the blood vessel walls and also they become disjointed. There is a persistent loss of blood when these tissues are damaged by the repetition of their usage.
It causes inflammation of the nasal cavity, which enhances the formation of mucus, leading to cases of a stuffy nose or even a blocked nose. The long-term consequences of chronic usage are congestion and sinus infection.
Yes, long-term cocaine abuse can erode the cartilage in the nostrils, leading to the collapse of nasal structures and perforation of the septum. In severe cases, this damage may require surgical reconstruction.
It’s strange how something that looks so harmless at first can cause damage inside the brain. Methamphetamine, more often called meth, isn’t just some quick high people chase at parties. It actually changes the way the brain functions. Not just during use, but long after. People often assume that once the drug wears off, things go back to normal. That’s not really the case.
The reality? Methamphetamine brain effects don’t just fade away. They leave a mark on how someone thinks and feels. It also affects how they remember things. These changes go beyond a temporary mood swing or foggy day. They affect parts of the brain tied to motivation, decision-making, and emotions. If you’ve ever wondered how meth affects someone mentally. Or, why it’s so difficult to walk away from, this is where it starts. In this article, we’ll take a look at what happens in the brain when meth is involved.
Let’s start with the basics, your brain’s wiring. It’s a network of electric and chemical signals doing their thing, nonstop. And meth crashes that system. More specifically, it hijacks your brain’s dopamine levels, which are the currency for pleasure, motivation, and reward.
Here’s how it plays out:
Altered brain chemistry affects your mood, motivation, and sleep. To feel normal, people start chasing that first high.
In the beginning, meth might seem like a magic fix. Energy becomes sky-high. Your confidence is off the charts.
But here’s what’s actually happening behind the scenes:
| Effect | What’s Really Going On |
| Euphoria | Extreme dopamine release overwhelms brain pathways |
| Alertness | Stimulant effects crank up brain activity and attention |
| Suppressed Appetite | Brain signals related to hunger get overridden |
| Sleeplessness | Meth disrupts circadian rhythm and sleep chemicals |
| Hyperfocus | Neural circuits are overstimulated, often obsessively |
These are signs your brain is being pushed past its limits. That crash feels brutal because your system has been drained dry. People often report intense irritability, confusion, and even aggression once the effects wear off. It feels like the brain is trying to reboot, but it’s not ready.
Long term use of meth can lead to both chemical and physical damage of brain tissue.
One of the major issues is the neural damage. Repeated exposure to meth alters yopur focus and memory.
Meth shrinks brain structures tied to cognitive function, emotion, and memory.

This is where it gets scary. Long-term meth use is tied to significant drops in mental sharpness. You might experience the following:
Everything around you becomes slower, glitchier, and way more frustrating than it used to be. And unfortunately, some of these changes can stick around even after someone quits.
The brain handles more than focus and memory. It’s your emotional center, too. Meth use, especially long-term can alter this aspect of your brain.
According to the National Library of Medicine (NLM), long-term use is deeply linked with mental health struggles and neuronal damage, including:
People often think the drug “brings out” mental illness. But in reality, it creates it, or at least mimics it. The brain’s emotional control panel is basically short-circuited. And even people with no prior diagnosis can develop symptoms that look a lot like schizophrenia or bipolar disorder after heavy meth use. The worst part? These symptoms sometimes hang around long after the drug is gone from the system.
We already talked about dopamine, but it’s not just dopamine levels that meth alters. Meth throws your entire neurotransmitter sytem into chaos.
Here’s a quick look at how this plays out:
| Neurotransmitter | What It Does | How Meth Affects It |
| Dopamine | Pleasure, reward, and motivation | Causes a huge surge, then long-term depletion |
| Serotonin | Mood stability, sleep, and digestion | Disrupted balance leads to mood swings |
| Norepinephrine | Alertness, arousal | Overstimulated leads to jitteriness and panic |
| Glutamate | Learning, memory | Altered signaling, tied to cognitive issues |
When these chemicals are thrown out of sync, your system is thrown out of balance. Mood. Sleep. Memory. You might feel “off” without knowing why. It’s a reflection of the subtle damage that meth has done to your brain cells.
This imbalance isn’t always easy to fix. Sometimes it takes months (even years) of being clean for the brain to go back to normal.
Thankfully, the brain is incredibly adaptive. Recovery is possible if someone gets the right support and stays off the drug long enough.
Healing doesn’t happen overnight. It follows a pathway like this:
Not everyone heals the same. Age, length of use, and genetics all play a role. But science shows the brain is capable of incredible recovery. Neuroplasticity (the brain’s ability to rewire) is a real phenomenon. You just have to give it time and the right environment.
If you’re reading this and thinking, “This is hitting way too close to home”, you’re not alone. Meth addiction is hard, and letting go is tough. But it’s possible.
Silicon Valley Recovery offers personalized support to help you or someone you love step away from meth for good. Their programs focus on not just detoxing the body but truly rebuilding brain chemistry, emotional resilience, and long-term mental health.
The journey’s not easy. You’ll have days that feel impossible. But with structured care, real guidance, and a team that gets what meth recovery actually takes, you’ve got a real shot at healing. You don’t have to go through it alone. Contact Silicon Valley Recovery today to start your healing journey.

When someone takes meth, it floods the brain with dopamine. At first, it feels incredible. But later, your brain starts slowing down its own dopamine just to keep up, and that’s where the trouble starts.
It knocks everything out of balance, your focus, memory, and clear thinking get cloudy. Even when someone stops using, things still feel “off” for a while.
Yes, absolutely. The longer someone uses it, the more it messes with the brain’s wiring, especially the parts that deal with judgment and cravings. After a while, it’s not just about willpower anymore; your brain is fighting against you.
It doesn’t just touch one chemical; it scrambles a bunch of them. This change can make it hard to sleep, remember things, or even stay calm. It’s not always obvious at first, but over time, you start to notice.
People sometimes start feeling paranoid, anxious, or even see things that aren’t there. The scary part is that it’s your actual brain structure changing in response to the drug. Getting back to baseline can take a long time.
If you or someone you know has been prescribed a white pill that is marked as M365 and you are not sure what it is and its uses, then you’re in the right place. The M365 pill appears like an ordinary white tablet, but that is not all about it. This is a drug that comprises two different drugs, called acetaminophen and hydrocodone. They are strong medications combined to help reduce pain. It is quite important to learn the contents in the M365 pill because each component has its role to play and also works differently in the body. Though an effective medicine, it is quite easy to abuse and end up becoming addicted to it or overdosing on it.
This article will break down what M365 entails, the substances it contains, the side effects, and how you can find relief with it in the safest way possible.
M365 pill is a powerful analgesic that contains two different components, hydrocodone and acetaminophen. They are both used in treating moderate to severe pain, especially after surgeries and injuries. On one hand, hydrocodone is a potent pain reliever (analgesic), and on the other, acetaminophen can be easily accessed as an over-the-counter medication sold as a headache or fever reducer.
Although the pill M365 might appear as a generic drug, it is not a generic drug and can only be prescribed by a doctor. This is because of how strong it is, and not to forget its abuse potential. Just like other painkillers, it can have side effects, especially when it is taken without proper medical guidance or taken for too long.
M365 pill is composed of two major components, and they are acetaminophen and hydrocodone bitartrate. The M365 tablet is oval-shaped and is coated in white with the following ingredients:
Each M365 pill consists of the following composition:
| Tablet | Hydrocodone Bitartrate USP | Acetaminophen USP |
| 5mg/325mg | 5mg | 325mg |
| 7.5mg/325mg | 7.5mg | 325mg |
| 10mg/325mg | 10mg | 325mg |
These are the other inactive materials found in these tablets they include magnesium stearate, crospovidone, povidone, microcrystalline cellulose, pregelatinized starch, stearic acid, and silicone dioxide.
All these are what make the M365 pill ideal as a moderate to moderately severe pain-related drug. It is prescribed only by the doctors when other medications against pain was prescribed and has not worked. This is the reason why it is very important to know what is inside it in order to make people use it in a safer way and prevent side effects.
Due to the main objective of the M364 pill, which is the reduction of moderate or atypically severe pain, it is usually prescribed following an operation, severe injuries, dental surgery, or chronic pain that can not be controlled by other medications.
Here are some of its common uses and benefits:
| Common Uses | Benefits |
| Post-Surgical Pain Relief | Helps manage pain during recovery. |
| Injury-related pain | Useful for broken bones, sprains, or deep bruising. |
| Dental Pain | Often prescribed after a tooth removal or oral surgery. |
| Chronic Conditions | Helps individuals manage long-term pain when other pain medications don’t work. |
The most important benefit of the M365 pill is how the combination of both hydrocodone and acetaminophen helps to block pain and provide individuals with the comfort they need.
Similar to most painkillers available on the market, the M365 pill is also packed with side effects, and this can occur either to a moderate or severe extent and in various forms in the body, especially when it’s not used correctly.
Here are the most common side effects of the M365 pills:
| Hydrocodone | Side Effects |
| Drowsiness and Dizziness | Makes you sleepy or lightheaded |
| Slow Breathing | It can make it hard to breathe perfectly. |
| Addiction Risk and Mood Changes | They affect emotions and can also lead to opioid dependence. |
| Acetaminophen | Side Effects |
| Headache, mild nausea | Individuals may experience discomfort in the head or stomach. |
| Liver damage, allergic reaction, or skin rash | Too much usage can harm your liver or cause allergic reactions. |
Common side effects of M365 pill (combined)
| Drowsiness, dizziness | It may make you feel sleepy or off balance. |
| Constipation | You may experience harder or less frequent bowel movements. |
| Nausea, headache | You can get an upset stomach or an uncomfortable pain in your head. |
| Slow or Shallow Breathing | Breathing becomes too weak or too slow. |
| Liver Damage | Extremely high dosage and excessive use can cause damage to your liver. |
| Severe Allergic Reaction | May experience swelling, rash, a racing heart, and difficulty breathing |
| Addiction | The opioid content makes it habit-forming, and one can easily develop dependency. |
It is significant to understand these risks to ensure that the M365 pill can be used safely and only when it is necessary.
Comparing the M365 pill with other pain relievers, the difference in the ingredients, strength, and side effects should be noted. The two ingredients contained in the M365 pill are quite powerful and may produce serious side effects, and are only taken under supervision.

Other painkillers, such as Tylenol (acetaminophen), Advil (ibuprofen), or Aleve (naproxen), are less serious. They are used to treat common illnesses like headaches, fevers, or common body aches. Because there’s a lower risk of addiction, these medicines can be safely used to treat mild pain. One should always talk to his or her health professional when choosing a pain reliever.
Due to the high potency of the M365 pill, it must be taken safely in order to prevent severe adverse effects or dependence.
Here are some key safety tips:
Using the M365 pill safely should be your priority, because if used carefully, it can become an effective part of your pain management routine, helping you enjoy a life without pain.
Living with pain wears you down. And not just physically. It messes with your head, throws off your sleep, and makes simple things feel harder than they should. After a while, anything that brings relief starts to look like a lifeline.
For some individuals, that’s where pills like M365 come in. At first, they help. They take the edge off. But if pain starts showing up more and more, at work, before bed, during moments that used to be fine without anything. That’s when it might be time to step back. Not with blame, but with curiosity. What’s really going on here?
It’s easy to miss the shift when you’re in it. One day you’re managing pain, and before you know it, the pills are managing you.
Needing help doesn’t make you weak. It doesn’t mean you’ve failed. It just means something’s gotten too heavy to carry on your own. At Silicon Valley Recovery, we don’t come at you with judgment or lectures. We meet you where you are, listen to your story, and figure things out together.
Our team knows what it’s like when life gets tangled. The fear, the shame, that feeling of not being sure who you are anymore. Sometimes, just talking it out is the first real step. You don’t need a plan or a perfect explanation. You just need a place to start.
If you’re wondering whether things have gone too far, that’s enough of a reason to reach out. You’re not alone in this. Not anymore.

It’s something people take for fevers or regular pain, and headaches. It doesn’t fix the actual thing causing pain, but it tells the brain to dial it down.
For headache relief, it helps, yes, but not if it’s from swelling. Ibuprofen is better for pain and swelling. Acetaminophen is also easier on the stomach, though, so some people prefer it.
Yes. It’s a generic version. It has hydrocodone plus acetaminophen, so it’s stronger, used when the pain’s more serious, not for a random sore muscle.
Liver problems mostly, if you overdo it. Some get rashes, feel dizzy, or even just sick after a while. It also doesn’t always show right away, either.
Stay under 4,000 mg in 24 hours. Also, check all your medications. Acetaminophen hides in a lot of them, and people don’t realize they’re doubling up.
Have you had back pains that just show up and refuse to leave? Maybe it started after hauling something heavy, or maybe it crept in after sitting too long, slouched over a desk, not moving much. You probably tried the basics: a little stretching, maybe a hot bath, some over-the-counter medication. But the ache stuck around. Then your doctor handed you a small white pill stamped with “AN 627.”
That little tablet isn’t random. It’s prescribed for a reason, and it does something specific in the body. But unless someone explains it properly, it’s easy to feel unsure or even a little hesitant about taking it. So let’s get into it, what the 627 pill is used for, how it works, and what to watch for. This article will help you understand what you’re taking and why it might (or might not) be the right call.
The AN 627 pill contains Tramadol Hydrochloride 50 mg. This is a prescription pain reliever. It’s used to treat moderate to moderately severe pain. It’s a synthetic opioid, which means it’s not as strong as morphine or oxycodone, but it still affects your brain’s pain receptors.
It is typically used for:
Here’s a short description of what it looks like:
It’s a Schedule IV controlled substance, meaning it has some potential for dependence, especially if misused, but is generally considered safer than more potent opioids.
It’s important for you to also know what’s in the AN 627 pill so you can know how it works and what to watch for, especially if you have allergies or sensitivities.
| Ingredient | Function | Notes |
| Tramadol Hydrochloride 50 mg | Active pain-relieving component | Acts on opioid receptors in the brain |
| Inactive ingredients | Binders, fillers, and preservatives | May include lactose, magnesium stearate, etc. |
Your doctor won’t just toss out AN 627 like you give candy to a kid. Usually, it only comes into the picture when the regular pain relief, like ibuprofen or Tylenol, just isn’t cutting it anymore. Maybe your back’s been acting up from too many hours hunched over a laptop. Or maybe you pulled something reaching for that one rogue sock under the bed or at the gym, and now your whole side hurts when you breathe.
This pill steps in when the pain is loud enough to mess with your day, whether that’s keeping you from sleeping, working, or even just walking around like a normal person.
The main benefit of it is that it helps take the edge off moderate to moderately severe pain without completely knocking you out.
Here’s where it’s commonly used:
| Condition | How AN 627 Helps | Typical Use Duration |
| Back pain | Relieves deep tissue and nerve discomfort | 3 to 10 days (short-term) |
| Muscle spasms | Calms the nervous system’s pain response | Often used with muscle therapy |
| Post-op recovery | Reduces surgical pain during healing | 1 to 2 weeks, depending on severity |
| Fibromyalgia flare-ups | Dulls widespread nerve-related pain | As needed during flare-ups |
The icing on the cake with tramadol (the active ingredient in the 627 pill) is that it doesn’t just block pain like most opioids; it also boosts serotonin and norepinephrine, two brain chemicals that help with both pain control and mood. So, it’s not unusual for people to feel slightly better emotionally, too, especially if the pain has been dragging them down.
That said, this pill isn’t a “set it and forget it” fix. It works best when combined with rest, maybe some physical therapy, or other long-term strategies. It’s more or less like a tool in your toolbox. It’s not the whole solution, but a helpful part of the process when you really need it.
Let’s say you take your first dose of the AN 627 pill and suddenly feel a little sleepy or dizzy. That’s absolutely normal, but it’s still something to pay attention to.
Like most prescription medications, Tramadol (the active ingredient in AN 627) comes with a few trade-offs. It eases pain, yes, but it can also make you feel a little off while your body adjusts.
Here are some of the more common side effects:
Most of these side effects are mild and tend to fade after your body gets used to the medication, usually within a few doses.
However, there are still a few side effects that are less common, but a lot more serious and life-threatening, including:
According to the CDC, even prescription opioids like Tramadol can lead to overdose or addiction risk if not taken as directed, especially when mixed with alcohol, benzodiazepines, or other sedatives.
So while the AN 627 pill can absolutely bring relief, it’s smart to stay aware of how your body reacts and keep your healthcare provider in the loop.
The AN 627 pill can interact with several other medications, potentially increasing your risk of serious side effects. Here’s a breakdown of some of the drugs to avoid while taking the AN 627 pill:
| Medication Type | Why It’s a Concern | What to Do |
| SSRIs/SNRIs (antidepressants) | May trigger serotonin syndrome | Tell your doctor before combining |
| Benzodiazepines | Increased risk of sedation and slowed breathing | Use only under close supervision |
| Other opioids or alcohol | Overdose risk increases significantly | Avoid mixing completely |
| MAOIs | A very dangerous interaction that can lead to seizures | Must wait 14 days after stopping MAOIs |
Even though this pill can be really helpful, it’s not the right fit for everyone. If any of the things listed below sound like you, make sure your doctor knows before you start taking it:
Also, it’s not typically recommended for kids under 12 or teenagers recovering from tonsil or adenoid removal due to increased breathing risk.
Talking with your healthcare provider is absolutely important before starting AN 627, especially if:
During the consultation, your doctor may ask:
If everything is ok, then they’ll recommend:
If you or someone you care about is taking the AN 627 pill and starting to notice signs of overuse, mood swings, or a growing dependence, then you need to ask for help. These things can sneak up on anyone, even when the medication was prescribed and used with the best intentions.
At Silicon Valley Recovery, we help people who are looking for a healthier, more balanced way to manage pain and feel more in control. Whether you’re concerned about how a prescription is affecting your day-to-day life or just want a plan that doesn’t leave you relying on pills long-term, we’ve got your back.
Here’s what we offer:
Reach out to Silicon Valley Recovery today to learn more or schedule a completely confidential consultation.

It’s mainly for pain that’s a little too much for Tylenol or Advil to handle, as a muscle relaxant for sore muscles, a bad back, or pain after surgery. It takes the edge off so you can function.
It works by calming your brain’s pain response and also helping your body chill a bit, which is very helpful when your muscles are all tensed up.
Not really. It’s not like drugs like ibuprofen. It doesn’t reduce swelling and has no anti-inflammatory benefits. But it does help your brain stop panicking about the pain. So the inflammation is still there, you just don’t feel it.
Some people feel a bit sleepy, dizzy, or nauseous at first, which is nothing too wild, but definitely something to keep an eye on. If things get weird (like confusion or trouble breathing), don’t mess around, call your doctor.
It’s used for more than just back pain. People take it for post-surgery pain, chronic pain flare-ups, and even conditions like fibromyalgia. Basically, anytime pain is messing with your day, and needs to be dialed down.
Millions of individuals worldwide have clinically diagnosed sleep issues, with complaints of lack of sleep or excessive drowsiness. The prevalence of this condition varies depending on the population and is higher in the older generation.
Hypersomnia and insomnia are among the most common sleep disorders. And they have profound effects on mood and productivity.
Over the years, insomnia has become the face of sleep disorders. But hypersomnia may seem unfamiliar to many. Indeed, both conditions differ, but they potentially pose the same health risks. So, understanding the natures of hypersomnia and insomnia is crucial in seeking appropriate medical treatment.
In this article, we’ve discussed the clear differences between hypersomnia vs insomnia. Moving on, we’ve also highlighted strategies for coping with both disorders.
Hypersomnia means excessive sleepiness. People with this condition feel unusually sleepy during the day, despite sleeping all through the night. Hypersomnia is a medical diagnosis with features of lack of alertness during the day.
With insomnia, you can’t fall asleep or stay asleep, even upon exhaustion. It’s one of the sleep disorders that greatly contribute to poor sleep quality.
People have different sleep patterns, so insomnia varies for individuals. The lasting duration forms the basis for classifying insomnia into acute and chronic.
| Features | Acute insomnia | Chronic Insomnia |
| Duration | A few days or weeks. | Lasts for three months or more. |
| Stressors | It’s triggered by work, family, or life events. | Underlying medical conditions, psychological disorders, or behavioral factors. |
| Symptoms | Symptoms include difficulty sleeping and staying asleep, or waking too early. | Manifestations are similar to acute insomnia except they’re more persistent. |
| Effects | Effects can be relatively mild. | The aftermath can be more severe on health and daily life. |
The risk factors for hypersomnia can be medical conditions or lifestyle-related.
Sometimes, you may think it’s insomnia, but it’s just stress, health issues, or the aftermath of some poor habits.

Hypersomnia can seriously affect everything from your job to your relationships. The struggle impacts concentration, memory, and alertness. Therefore, it affects performance and increases the risks of accidents.
Other effects include anxiety, irritability, and mood changes. Due to immobility, hypersomnia can also cause other medical conditions originating from reduced muscle strength and lung capacity.
Sometimes, depression may develop, like in insomnia. Cases of incessant headaches, dizziness, and cold extremities have also been recorded.
| Short-Term Effects of Hypersomnia | Long-Term Effects of Hypersomnia |
| Fatigue | Work and school impairment |
| Difficulty concentrating | Increased risk of mental health issues |
| Irritability | Social isolation |
| Decreased energy levels | Relationship challenges |
| Mood changes | Potential accidents and injuries |
The effects of a lack of sleep on relationships aren’t subtle. From decreased emotional connection, communication deficits, to brewing conflicts, you risk truncating important bonds.
When you haven’t slept in a while, it’s hard to connect with your partner emotionally. You might be perceived as withdrawn and less likely to share your vulnerabilities. Without intervention, intimacy gradually fades off. As a consequence, this makes it difficult for a sleep-deprived individual to feel close and supported.
The constant irritable state from lack of sleep also increases conflict. This may explain why you react harshly to situations that normally wouldn’t bother you. The heightened stress levels also make it difficult to cope with relationship challenges.
The remedies for sleep issues are multifaceted. And their effectiveness may vary depending on individuals. However, certain strategies are proven and are crucial starting points.
| Strategies | Description |
| Adjust your lifestyle | To avoid interfering with night sleep, have minimal daytime naps. Consider limiting your caffeine use, practice relaxation, exercise regularly, and prioritize a balanced diet. |
| Be more intentional about sleep | Practice good sleep hygiene by having a regular bedtime schedule. This helps to set your body’s circadian rhythm. In addition, ensure your bedroom is comfortable and devoid of unpleasant sounds. |
| Consider standard techniques | Cognitive behavioral therapy can address thoughts and actions contributing to sleeplessness. The use of medications and light therapy are also helpful. |
Hypersomnia isn’t your fault, but it can make daily life harder. To help adjust, these are some coping suggestions.
Introducing some self-care routines into your practices is the best bet at alleviating insomnia symptoms.
When hypersomnia or insomnia starts to affect daily life, it’s getting serious! Don’t wait till symptoms last for weeks, or your performance at work starts taking a downward turn. Go find a specialist to confide in.
Again, since sleep and mental health are connected, you may benefit from a therapist, too. Sleep experts or your primary healthcare physician can also be your first contact.
Do you feel your irregular sleep pattern is related to some mental health concerns? Silicon Valley Recovery specializes in sleep problems, with experts ready to listen.
If you’re struggling with sleep, don’t shrug it off! Come where help is. Contact Silicon Valley Recovery to talk to someone who understands.

Hypersomnia and chronic insomnia are opposite terms. The former makes you remain drowsy even after an adequate night’s rest. But chronic insomnia keeps you from getting the rest in the first place and lasts for about three months.
Frequent drowsiness impacts crucial aspects of your daily life, like your work and relationships. By disrupting your normal biological clock and reducing restorative sleep, sleep deprivation affects your sleep quality.
Sleep apnea can cause both hypersomnia and insomnia. Interestingly, one may lead to the other. It can disrupt your sleep so much causing you to feel too tired or unable to sleep at all.
Circadian rhythm can explain excess or absent sleep. In hypersomnia, you need to address the altered biological clock. But for insomnia, it’s more important to synchronize the internal sleep clock with the environment.
Narcolepsy, hypersomnia, and insomnia account for sleep inappropriateness. They all cause excessive daytime sleepiness. But narcolepsy includes sleep attacks (cataplexy), sleep paralysis, and hallucinations.
It’s not unusual for kids or teens to lash out. They get frustrated, boundaries feel tight, and emotions boil over. But then there are moments when the behavior feels off. Not just moody or stubborn, but like something deeper is going on.
That’s when terms like conduct disorder vs oppositional defiant disorder are tossed around. If you’re not a mental health professional, they can sound pretty similar. At a glance, both involve trouble following rules. It could be frequent arguments and a lot of stress for everyone involved. But they’re not the same thing.
One tends to involve more calculated behavior that hurts people. They break serious rules or cross legal lines. The other is about strong emotional reactions. This could be holding onto resentment. From the outside, it can be tough to tell which is which.
Are you worried about your child or trying to help someone else’s? Knowing the difference between these two can make a big impact. Not just in understanding what’s going on, but in figuring out what kind of support actually helps. So let’s get into it.
Mixing these conditions up is common. The names sound technical, and symptoms can overlap.

Conduct Disorder, or CD, is the more intense of the pair. It’s not just a kid acting out now and then. This is about repeated behavior that crosses serious lines. Breaking rules, hurting people (sometimes physically), lying, stealing. This happens without showing much, if any, guilt. What sets it apart is how detached it can seem. There’s often a coldness to it, and the usual “I feel bad” response isn’t there.
Then there’s Oppositional Defiant Disorder (ODD). It’s still disruptive; however, it is more emotional than aggressive. A child with ODD might constantly argue, push back against rules, or get angry. Especially when things don’t go their way. They might lash out at parents or teachers, not because they want to hurt you, but because they feel misunderstood. That emotional charge is hard to miss.
Here’s something worth noting: just because a child has ODD doesn’t mean they’ll go on to develop CD. Defiance and emotional struggles should be addressed early. This can prevent things from spiralling.
Both of these disorders mess with behavior in intense ways, but the actions are different.
People with CD might:
What’s scary is how normal this can seem to them. The emotional detachment is what often separates CD from other behavioral issues.
Now with ODD, you’ll often see:
Unlike CD, there’s usually some guilt or remorse with ODD. They don’t have cold, calculated behavior.
Why does this even happen? There’s no single cause; it’s more of a perfect storm of biological, psychological, and environmental factors swirling together.
Let’s start with genetics. According to research from the National Library of Medicine (NLM), these disorders run in families. That doesn’t mean they’re guaranteed to show up, but family history matters. Then there’s the brain. Children with either disorder often show differences in the areas responsible for emotional regulation and impulse control.
Other common factors include:
These factors can increase the risk of these disorders manifesting.
Here’s a table to break it down clearly:
| Risk Factor | Conduct Disorder | Oppositional Defiant Disorder |
| Genetic predisposition | Strong link | Moderate link |
| Early childhood trauma | Common trigger | Can contribute |
| Parenting style | Neglect or harsh discipline | Inconsistent discipline |
| Brain structure/function | Differences in the prefrontal cortex | Issues with emotional regulation |
| Environmental stressors | High impact | High impact |
Just because these risk factors exist doesn’t mean a child will develop CD or ODD. But it does mean we should be attentive.
Here’s the good news: with the right help, things can get better. These aren’t life sentences, they’re starting points for recovery.
CD often needs a full-on, multi-layered approach. You can’t discipline your way out of it.
One of the most important pieces here is consistency. No mixed messages. No false threats. Boundaries need to be rock-solid, or nothing changes.
ODD treatment focuses more on emotional coaching and structured environments.
It helps to rewire emotional responses rather than “fixing” bad behavior. This also takes time and consistency.
If left untreated, both of these disorders can cause a lot of long-term damage. This could be academically, socially, emotionally, or even legally.
Children with conduct disorder are at a higher risk for:
They often get labeled as “bad kids” instead of kids who need mental health treatment. That stigma can shut down opportunities before they even start.
With ODD, the risks are a little different but still serious:
Early intervention isn’t just helpful, it’s critical. It’s the difference between a kid spiraling and a kid recovering.
If any of this is ringing alarm bells for someone you care about, don’t wait. The sooner you get support, the better the outcomes.
At Silicon Valley Recovery, we understand that behavioral issues aren’t just surface-level problems. We dive deep to understand what’s really going on beneath the outbursts, the aggression, the defiance.
Whether it’s impulse control, antisocial behavior, or working through past trauma, our team builds custom care plans that meet kids where they are, without judgment.
Contact Silicon Valley Recovery today. Start a conversation that could change everything.

Conduct disorder involves more severe behaviors like violence or criminal activity. ODD is typically marked by emotional outbursts, defiance, and anger without harmful intent.
In CD, defiance often comes with deliberate rule-breaking and disregard for others’ rights. In ODD, it shows up as stubbornness, arguing, and refusal to follow directions, mainly with authority figures.
Aggression in CD is usually physical and intentional, with antisocial patterns. ODD may include verbal aggression but typically lacks the calculated or harmful behaviors seen in CD.
CD tends to involve a deeper disregard for rules and authority, while ODD is more reactive. Children with ODD often lash out when frustrated or challenged, but don’t plan rebellion.
Both affect emotional regulation, but ODD is more emotionally volatile. Peer relationships tend to suffer in both cases, though CD behaviors may result in more social isolation or peer rejection due to safety concerns.
Have you ever talked to someone you love? Someone who’s clearly struggling, and catch them in yet another lie? That’s the thing with alcoholics’ deception. It doesn’t always look like a flat-out lie. Sometimes it’s half-truths. Sometimes it’s silence. And sometimes, it’s a performance that’s so convincing, even they start believing it.
But why does this happen? Why do people battling addiction so often turn to deception? Even with the people who care about them most? It’s not always about being manipulative. More often than not, it’s tangled up in fear, shame, and this primal need for self-preservation. In this article, we’ll talk about the behaviors and psychology of alcoholics’ deception, the ripple effects, and how you and your loved one can find support.
Not all lies are malicious. A lot of them are born from pain, confusion, or just plain panic. For someone dealing with addiction, lying can become second nature, almost like a reflex.
Here’s why those lies happen more often than you’d think:
For some, it’s a form of control. When life feels like it’s spinning out, a well-placed lie can create a brief illusion of order. It gives a sense that everything’s still manageable (even when it’s not).
The why behind alcoholics’ deception goes beyond just avoiding trouble. They’re trying to protect a fractured sense of self. A person caught in the grip of addiction is often battling an intense internal war. On one side, there’s the craving, the desperate need for alcohol that overrides logic. On the other hand, there’s the guilt, the shame, the quiet knowledge that something is very wrong.
And lying becomes a survival tool. A way to keep the two sides from crashing into each other.
Here’s how that plays out:
| Psychological Driver | How It Fuels Deception |
| Cognitive Dissonance | When actions (like drinking) don’t match values (like loving family), lying “reconciles” the gap. |
| Ego Defense Mechanisms | Denial, projection, and rationalization help the person avoid blame or guilt. |
| Addiction Hijacks Logic | The brain’s reward system is rewired to prioritize drinking over honesty or morals |
| Trauma and Shame Cycles | Past trauma fuels emotional pain, and alcohol numbs it; lying protects that cycle from being broken |
| Fear of Identity Loss | Admitting the truth might mean facing an entirely new, terrifying reality. Lying preserves the old self, for a while. |
If you’ve ever tried to talk to someone who’s deep in this headspace, you already know how complicated it gets.
If you’ve been around someone struggling with alcohol long enough, you’ve probably heard a few of these:
You might recognize some of these statements. They’ve become all too familiar in homes touched by alcohol misuse. But not every lie is loud or obvious. Sometimes it’s things not said. A half-hearted “I’m fine.” A quiet deflection when someone asks how the night went. Maybe it’s a look, or a shrug that doesn’t match the mood. This deception still chips away at trust. Even if no words are spoken.
The person lying isn’t always doing it to hurt anyone. Often, they believe their version of the story. Or they need to believe it, because the real version is too hard to face.
The emotional damage from alcoholics’ deception is real. It chips away at trust, sometimes in ways that feel impossible to fix. You want to believe the person. You try. But every time you catch them in another lie, it stings a little deeper.
Here’s what often happens:

It’s not just romantic partners or parents; it can be anyone. Friends, siblings, coworkers. Deception doesn’t discriminate. It burns bridges across the board.
Denial is one of the sneakiest parts of addiction. It’s also one of the hardest to crack. You’ve probably heard this one before: “I don’t have a problem.” Simple. Dismissive. And, tragically wrong.
But here’s the thing, denial isn’t always a choice. It’s often a subconscious defense, a way the brain shields itself from unbearable truths.
Let’s break this down a bit:
| Denial Type | What It Looks Like |
| Minimization | “It’s not that bad.” “At least I’m not doing drugs.” |
| Justification | “I had a hard day. I deserve this.” |
| Blame Shifting | “If you weren’t always nagging me, I wouldn’t drink so much.” |
| False Control | “I can quit whenever I want – I just don’t want to right now.” |
| Selective Memory | “I don’t even remember doing that. Are you sure it happened?” |
You can’t talk a person out of denial if they’re not ready. But when cracks start to form, when the lies stop working even for them, that’s when change can maybe begin.
So, how do you know if someone’s lying about their drinking? It’s not always obvious. Some people are really good at covering their tracks. But there are definitely signs. And once you see the patterns, it’s hard to unsee them.
You might notice:
Alcoholism recovery is possible. It’s hard. But not impossible. The road back starts with honesty. And not just from the alcoholic, but from everyone involved. If there’s been manipulation, denial, or years of emotional landmines, healing takes time. And patience. And probably many uncomfortable conversations.
Recovery isn’t just about quitting alcohol. It’s about building a new way of living, one where lying isn’t necessary for survival.
Here’s how support can actually help:
| Support Strategy | Why It Matters |
| Family Therapy | Rebuilds trust and opens communication in a safe space. |
| Accountability Partners | Encourages honesty and helps track real progress. |
| Boundaries | Prevents enabling and encourages responsibility. |
| Group Support (like AA) | Provides understanding and accountability from people who get it. |
| Mental Health Counseling | Tackles underlying issues like trauma, anxiety, or depression. |
If you’re the one offering support, don’t forget – you matter too. You can’t pour from an empty cup. Set boundaries. Seek help. Talk to someone. Because you’re part of this story, too, and your healing counts just as much.
If you’ve made it this far, there’s a reason. Maybe you’ve seen these patterns up close. Maybe you’re living them. Either way, you don’t have to figure this out alone. Addiction is brutal, but recovery doesn’t have to be.
At Silicon Valley Recovery, we get it. The lies, the guilt, the spiral of shame and fear. We’ve walked people through it all. Our approach isn’t about blame. It’s about healing. About showing up for the messy truth and working from there.
Whether you’re struggling yourself or watching someone you love fade behind the curtain of alcoholics’ deception, it’s okay to ask for help. In fact, it might be the bravest thing you’ve ever done. Contact Silicon Valley Recovery. Let’s face this together.

They lie to fool others. Sometimes, they’re trying to fool themselves, too. Facing an addiction can feel overwhelming. It becomes a way to avoid that discomfort, even if it hurts the people around them.
When someone knows deep down they’ve let people down, or let themselves down, it’s easier to cover it up than sit with that guilt. Shame has a way of making people hide, and lying becomes the shield.
They might be scared of losing something, their job, a relationship, or both. And when your brain is screaming “protect yourself,” even if that means bending the truth, lying starts to feel like the safer option, at least in the moment.
Some individuals might twist the story, shift blame, or make you question what really happened. That kind of thing often comes from desperation, not always cruelty. But it still causes damage.
Denial helps them avoid that. It makes the drinking seem “not so bad,” even when everything says otherwise. It helps them build a bubble that’s hard to pop.
You’ve probably heard the names naltrexone and Narcan thrown around when people talk about opioids. Maybe on the news, maybe in recovery stories. They’re both used to fight the effects of opioids, but the way they work is completely different. One is something you reach for in the middle of an overdose. The other is more for staying clean in the long run. Usually, after someone’s already detoxed, and want to stay that way.
Are you trying to make sense of which one does what? Or you’re worried about someone close to you? In this article, we’re going to look at the difference between naltrexone vs Narcan. We’ll discuss how they’re used. When they come into play, and where they fit into addiction recovery. We’ll also go over things like opioid withdrawal. What emergency overdose reversal is, and how medication-assisted treatment fits into the bigger picture of getting clean.
Let’s start with naltrexone. It’s not the medication used in a crisis or right after someone overdoses. Instead, it’s more of a tool that’s used later in the process. Once someone’s already been through detox and is trying to stay clean. It’s been around for a while and is often used in recovery programs. It provides support to people dealing with opioid addiction. It can also help treat alcohol dependence.
Here’s what makes it stand out:
It binds to the same receptors in the brain that opioids do. It, however, doesn’t trigger the feel-good rush. It simply makes it impossible for opioids to attach.
Here’s why a lot of recovery programs use it:
Now let’s talk about Narcan. Unlike naltrexone, this one is used for emergencies, those terrifying moments when someone’s overdosing and every second counts. It acts fast. You’ve probably seen stories where someone was unconscious, and within minutes of getting Narcan, they were breathing again. That’s what this drug is made for.
It’s widely carried by first responders, healthcare workers, and even regular individuals who want to be ready in case someone around them overdoses. It’s become a big part of harm reduction strategies, especially with how common overdoses have become in recent years.
| Feature | Narcan |
| Purpose | Reverses opioid overdose instantly |
| How it’s given | Nasal spray or injection |
| Speed | Kicks in within 2–3 minute |
| How long it lasts | Around 30–90 minutes |
| Accessibility | Over-the-counter in many places |
Narcan is a brand name for naloxone. It is another opioid antagonist. It’s designed to pull opioids off brain receptors. It won’t cure addiction, but in that moment when someone’s not breathing, Narcan can save their life.
So here’s where things really start to separate. Even though naltrexone vs Narcan sounds like they’re doing similar things, they’re used in completely different situations.
Naltrexone is for people who are no longer using opioids but need help staying clean. It’s all about managing cravings and preventing relapse. You don’t use it when someone’s overdosing, it takes time to work, and has to be taken regularly.
Narcan, on the other hand, is for the exact moment of crisis. If someone’s overdosing and their breathing slows or stops, Narcan steps in. It removes the opioids from their receptors almost instantly. It’s a lifesaving intervention, not a long-term treatment.
One more thing, naltrexone requires that a person be detoxed already. Starting it too soon can throw someone into intense opioid withdrawal, which is dangerous and incredibly painful. Narcan doesn’t have that issue. It’s designed to act fast without any preparation.
So yeah, same family of drugs (opioid antagonists), but very different roles.
Let’s break down how each one is used, because timing, ease of use, and setup really matter here.
Naltrexone:
Narcan:
One of the biggest differences here is access. Narcan is meant to be simple. You don’t need medical training to use it. Naltrexone, though, takes some planning and oversight to start and maintain.
Deciding between Narcan and naltrexone depends on where someone is in their journey. One saves lives in a moment of crisis, and the other supports people over the long haul. They’re not competing treatments, they serve different purposes.
| Factor | Naltrexone | Narcan |
| When it’s used | After detox, for relapse prevention | During an overdose |
| Form | Daily pill or monthly injection | Spray or injection |
| Who uses it | Prescribed for stable patients | Anyone, including bystanders |
| Goa | Long-term addiction recovery | Immediate overdose reversal |
| Mental health support | Often paired with counseling | Not applicable in isolation |
So if someone is in active recovery, working with a provider, and looking to stay clean, naltrexone might be part of their plan. But if someone is at risk of overdosing, or around people who are, Narcan should absolutely be close by.
In the big picture of addiction recovery, both Narcan and naltrexone have something meaningful to offer. Narcan isn’t just a rescue tool; it’s a second chance. It gives people the opportunity to survive long enough to get help. That’s a huge deal in communities hit hard by opioid overdoses.
Naltrexone, though, is what can help once someone decides they want out of the cycle. It gives people a fighting chance to say no. A great tool to avoid relapse.
These aren’t rival medications, they’re teammates. One keeps the heart beating, the other helps rebuild a life.
Recovery isn’t easy. It’s also not always clear where to begin. But knowing the difference between emergency tools like Narcan and ongoing options like naltrexone is a start. If you or someone close to you is facing the challenges of substance use disorder, you don’t have to figure it out alone.
At Silicon Valley Recovery, we take a full-picture approach. We look at not just the physical side of addiction, but also the emotional, social, and psychological parts. Whether you need a plan to stay sober, guidance on medication-assisted treatment, or just someone to talk to about what’s next, we’re here for it.
Reach out to Silicon Valley Recovery today and take that first, solid step toward something better.
Narcan works fast in emergencies, kicking opioids off receptors to restore breathing. Naltrexone isn’t for emergencies. It is used in long-term prevention and support after detox.
Narcan is key for saving lives during an overdose. Often given to friends, family, or responders. Naltrexone helps reduce relapse risk later on, making it part of a broader harm reduction plan.
Not really. It can’t be used during withdrawal; it actually makes symptoms worse if opioids are still in your system. It’s for use after detox, as part of a long-term treatment plan.
Unlike methadone or buprenorphine, naltrexone has no addictive properties. It doesn’t cause a high and doesn’t require daily clinic visits. This makes it ideal for certain recovery paths.
Narcan can mean the difference between life and death. Quick use can restore breathing in minutes. This gives people enough time to get emergency help and survive the overdose.
Drugs like Adderall can help significantly reduce ADHD symptoms. It helps you focus and stay on track. Especially on days your brain wants to do everything except what’s on your to-do list. But then comes a big life shift – you’re pregnant.
And suddenly, the pill that’s helped you keep it together becomes a big question mark. “Can I keep taking Adderall during pregnancy? Will it hurt the baby? What happens if I stop?”.
The answers to this question aren’t always black and white. There’s a lot of gray area when it comes to stimulant medications, pregnancy risks, and mental health.
In this article, we’ll break down what the science says. Focus on what doctors recommend and what real alternatives are out there for ADHD management during pregnancy.
Adderall has two active ingredients, amphetamine, and dextroamphetamine. These stimulants help boost focus. They also increase dopamine and norepinephrine levels in the brain.
If you’ve been on Adderall, you probably know how it works. It makes it easier to concentrate. You manage impulsivity and navigate everyday responsibilities better. It helps when you’re chasing deadlines. Great for juggling family life, or just trying to get through the day without feeling overwhelmed.
Some of the benefits of Adderall include:
Prescription medications could affect fetal health. This is why you should be extra cautious.
So, what does research say about Adderall during pregnancy? Unfortunately, there’s no simple answer. There haven’t been large-scale, controlled studies on pregnant women (for obvious reasons). Most of what we know comes from observational studies, case reports, and animal testing.
Still, here’s what current research suggests:
| Observation | What Studies Show |
| Increased risk of low birth weight | Seen in some cases, especially with consistent high-dose usage |
| Higher chance of premature delivery | Possibly linked to stimulant-induced stress responses |
| Fetal growth restriction | Noted in some animal studies and select human case reports |
| Withdrawal symptoms in newborns | Babies exposed regularly may show signs of irritability and fatigue |
It’s worth noting that these findings are trends. They are not certainties. Some studies identify these risks clearly. Others find little to no impact. But we do know that Adderall is classified as a pregnancy category C drug by the FDA. This means animal studies suggest possible fetal harm. Human data is limited.

The CDC recommends that women speak with their doctor before starting or stopping any medications during pregnancy. Particularly those that could influence fetal health, like stimulant medications.
Let’s break this down even further. When it comes to how Adderall might impact a developing baby, here are some key concerns that researchers and doctors look at:
| Potential Risk | Likelihood | Notes |
| Congenital heart defects | Low to uncertain | Seen in limited studies; more research is needed |
| Premature birth | Moderate | Higher in women using high-dose Adderall or multiple medications |
| Low birth weight | Moderate | Especially if Adderall use affects maternal appetite or nutrition |
| Neonatal withdrawal symptoms | Moderate to high | Can include sleep issues. Irritability, or feeding difficulties |
The FDA lists Adderall as a pregnancy category C drug. This means animal studies show adverse effects on the fetus. However, there aren’t well-controlled studies in humans.
Are you dealing with intense ADHD symptoms? Your doctor might still recommend continuing Adderall. This will usually be at the lowest effective dose. This will also be with routine monitoring.
If symptoms are manageable, you can try other approaches. Your doctor might suggest adjusting or stopping Adderall during pregnancy. This is to lower potential risks.
Stopping Adderall during pregnancy can feel overwhelming. The idea of managing without it might seem impossible. But there are options. Proven ones that many women turn to. Especially when stimulant medications aren’t ideal during pregnancy.
Therapy and lifestyle tweaks are great alternatives. Mindfulness and nutritional shifts are also great. They can help manage ADHD without Adderall. It just takes some planning, flexibility, and the right support.
Here are the safest and most effective alternatives:
| Alternative | What It Is | How does it help |
| Cognitive Behavioral Therapy (CBT) | Structured talk therapy that. It builds habits and routines | Improves time management and focus. Helps with emotional regulation |
| Mindfulness & Meditation | Practices like breathing or guided meditations | Helps with mood swings, anxiety, and attention span |
| Nutrition & Lifestyle Tweaks | Omega-3s, protein and exercise. Also, sleep, and hydration | Supports brain health and reduces brain fog |
| ADHD Coaching | support with ADHD-focused professionals | Breaks tasks into manageable steps. This builds structure |
| Non-Stimulant Medications | Options like Wellbutrin (when truly needed) | Considered when symptoms are severe and unmanaged |
These strategies have helped numerous pregnant women stay on track. Feel balanced without compromising fetal health.
Make sure to consult your doctor before changing your routine. Together, you can build a plan. One that supports both your mental health and your baby’s development.
Don’t rely on medication to manage ADHD. Here are a few things you can do:
These approaches can be game-changers, especially when combined with occasional medication.
Every person’s journey is unique, so don’t skip the check-ins with your care team, especially:
These are the areas you’ll need to cover during conversations with them:
ADHD is a lot to handle already. Adding pregnancy into the mix can feel overwhelming. That’s why Silicon Valley Recovery is here to support the whole picture.
We offer Individualized consultations to weigh medication choice and timing, therapeutic support, like prenatal mindfulness, CBT, and life coaching, ADHD-friendly planning tools, so you don’t have to go at it alone, transition support, whether you’re tapering meds or switching approaches and a qualified, friendly team that will work with you without making you feel like you’re being judged, just partnership.
So whether you’re thinking of staying on Adderall, considering an alternative, or wanting supplemental support during pregnancy and beyond, we’re here for you every step of the way. Contact Silicon Valley Recovery to get started today.

Using Adderall has been linked to an increased chance of low birth weight. Some report early delivery and rare birth defects like gastroschisis. Still, most studies find these risks remain low and manageable with oversight.
Yes! Options include methylphenidate or non-stimulants like Strattera. Therapy techniques such as CBT and mindfulness also help. All should be reviewed with your doctor.
Animal studies show some risk. However, most human studies, especially large reviews, don’t find a significant rise in birth defects. Overall, the risk remains small.
Adderall is a Category C drug, meaning animal studies show potential risk. Human data is, however, limited. It signals that careful monitoring and discussion with your providers are important.
Adderall does pass into breast milk. Because its effects on babies are not well-studied, experts typically recommend waiting or using other ADHD strategies for breastfeeding safety.
Modern society experiences one of its most destructive substances through the harmful use of crystal methamphetamine which society recognizes as meth. The National Institute on Drug Abuse reports that 1.6 million Americans used methamphetamine during the past year, leading to substantial growth in substance abuse incidents. A condition known as “meth face” describes the noticeable physical breakdown of someone’s face that occurs when they use methamphetamine over extended periods. Methamphetamine abuse results in permanent physical and emotional damage to its users.
The numerous destructive effects of methamphetamine upon the body become most visible through the facial tissue. The markers of meth face include facial sores, skin picking and meth mouth and sudden shifts in skin appearance. Methamphetamine damages the body to create visible wounds that reveal the extent of addiction damage while affecting users’ physical and mental well-being. This blog will investigate meth face origins, alongside its physical and mental effects, and the permanent damage done to substance abusers and their lives.
Methamphetamine damage extends beyond brain functions since it causes substantial bodily harm to the facial area. The telltale symptom of meth face manifests as severe skin damage along with facial sores and accelerated tooth decay. Visible marks on the body demonstrate how meth ravages both physical health and emotional stability of users.
The common hallucination of bugs crawling beneath the skin leads individuals to itch and dig at their faces compulsively. After stopping drug use, the damage to skin and scarring continues to produce painful sores that survive drug exposure. Meth mouth emerges from dry mouth, poor dental care and acidic saliva to produce broken teeth while destroying gums. The rate at which skin ages contributes to a physical appearance that makes users seem older than their actual age.

The physical effects of methamphetamine addiction affect more than appearance because it damages various parts of the body. Methamphetamine destroys the body through multiple destructive mechanisms. The skin condition known as meth face demonstrates all the physical destruction from regular drug abuse while identifying continued substance abuse issues. Every area of the human body experiences the widespread negative effects that develop from methamphetamine addiction, while the face remains the most visually noticeable manifestation.
Skin damage represents one of the most significant consequences of methamphetamine drug abuse. Rapid weight loss among Meth users results in sagging skin and wrinkling together with decreased collagen production which drives up skin aging. Meth addiction causes the skin to become fragile because addicts often experience malnutrition and dehydration which are common characteristics of drug abuse.
Methamine abuse beyond creating meth face causes detectable bodily signs which impact various parts of the human body. The physical modifications methamphetamine creates inside the body function as clear indicators of the dangerous substances it releases into the system.
Individuals suffering from Meth Addiction display the following group of physical indicators:
Individuals who use methamphetamine typically develop visible skin and facial damage which doctors refer to as meth face. The drug produces adverse effects on the skin, resulting in dehydration and deterioration, leading to permanent changes in facial features.
Skin dehydration caused by meth leads to sagging and dryness that results in an unhealthy appearance of the skin. Lack of moisture in the skin increases its susceptibility to both irritation and damage.
While under the influence of meth, users often develop hallucinations which drive them to compulsively pick their skin resulting in face-specific painful sores and scars.
Meth usage elevates cortisol in the blood leading to acne conditions and skin infections that result from restrictive pore circulation and improper cleansing.
People who use meth experience dry mouth leading to tooth decay which results in meth mouth and final tooth loss that modifies their facial structure while creating a sunken facial appearance.
Methamphetamine contributes to the rapid destruction of collagen and elastin, resulting in premature aging of the skin with wrinkling and sagging.
The prolonged exposure to methamphetamine leads to dental destruction that medical professionals call meth mouth. When consuming the drug, saliva production decreases, causing dry mouth that facilitates bacterial growth and speeds up the process of tooth decay. Methamphetamine use contributes to extensive dental cavities while causing severe gum disease and eventually leading to severe tooth loss.
Substance abusers commonly avoid taking care of their teeth because methamphetamine consumption disrupts their ability to perform regular dental practices. The fast-acting damage to teeth results from dry mouth together with forgotten dental care and constant sugar desires, which causes teeth to turn black or break apart or disappear. Methamphetamine addiction produces two alarming signs, which include both apparent tooth destruction and facial tissue destruction that results in permanent impacts to eating, speaking, and smiling abilities.
The visible manifestations of meth face and meth mouth represent only two of the extensive physical impacts that methamphetamine damages throughout the whole body. The drug’s extremely stimulating nature produces various symptoms through its destructive impact on regular bodily functions, which leads to wide-ranging harm throughout the user’s lifetime. Some of the major physical consequences related to crystal meth consumption follow in this table.
| Physical Symptom | Description |
| Severe Weight Loss | Meth suppresses appetite, leading to extreme weight loss and a gaunt appearance. |
| Dilated Pupils | Meth causes the pupils to dilate, resulting in unnaturally large eyes. |
| Increased Heart Rate | The drug accelerates the heart rate, leading to potential heart problems. |
| Hyperactivity | Users often experience extreme restlessness, excessive movement, and tremors. |
| Sweating and Overheating | Meth causes excessive sweating and body temperature regulation problems. |
| Skin Burns and Sores | Due to intense scratching or the effects of the drug, skin becomes damaged. |
Methamphetamine use leads to physical changes that create serious mental health consequences. Appearing changes to the face function as perpetual evidence of drug damage that impose substantial mental health challenges to users. The physical descent of users induces both social discrimination and shame while advancing their emotional disorder and anxiety to levels that become severe depression.
Meth face generates such heavy psychological distress that users tend to isolate themselves and become more depressed which drives them to continue drugs as their primary coping mechanism. Patients who battle meth addiction need help to recover from both their drug-induced physical problems and their resulting emotional and mental health damage.
Facial features, dental and skin damage, which become obvious to others, result in major emotional harm to a person’s sense of self.
Methamphetamine abuse signs that are apparent in the body create challenges for users because they face social rejection, which reduces their ability to connect with others.
The physical breakdown combined with social isolation risks depression and anxiety development at times when users feel entrapped by their body appearance.
Shame and guilt become almost overwhelming emotions for meth users that block their ability to find help or start recovering from their addiction.
Some individuals experience emotional failure that drives them back to drugs while trying to escape their physical damage-related distress.
The effects of methamphetamine abuse like meth face might seem permanent at first but suitable medical assistance alongside recovery programs will help people heal. Those who dedicate themselves to healing can achieve both emotional and physical wellness recovery. Through detoxification, along with proper nutrition and dental care combined with therapy, individuals can undo the damage from methamphetamine abuse. Through dedicated care and treatment programs, many people can restore their physical health and rebuild the foundation of their lives.
Silicon Valley Recovery offers complete treatment plans that supply essential resources so patients can learn addiction recovery methods and discover the path to wellness. Contact our team today to start your healing process and recover your physical and emotional well-being.

Weight loss and facial sores and tooth decay (meth mouth) and skin damage result from an addiction to methamphetamine due to dehydration and compulsive behaviors.
Hallucinations from Crystal meth usage creates a sensation of bugs beneath the skin that drives users to continuously scratch themselves leading to extensive skin injuries.
The drug-induced drying effect of methamphetamine causes severe tooth decay and gum disease which doctors call Meth mouth.
Long-term methamphetamine abuse destroys multiple body systems, creating enduring changes that affect both physical and cognitive abilities as well as dental well-being and overall health.
Drug addiction causes wrinkled, sagging skin combined with dilated pupils, while also resulting in acne, facial sores, tooth decay, and sunken features because of methamphetamine use.
It is well known how important it is for a patient to trust their doctor. When you discover your mental health condition or mood disorder requires you to take prescription medication to either get rid of the symptoms that bother you or lessen their negative impact on your life, carefully listen to the instructions given to you by your mental health care provider. Ativan is one of the drugs that can help an individual to cope with their illness as well as cause intense side effects.
In this guide we will discover Ativan effects and find out what it feels like when taken. We will also understand its impact on the body and mind, including potential side effects and risks, so that you know when you are supposed to get medical assistance as a patient with a prescription.
Ativan is a popular prescription medication whose main purpose is to treat the manifestations of anxiety, sleep disturbances, and all types of seizures. The response to this drug may vary based on dosage and individual factors such as metabolism and weight of the individual – it is advised to take a small amount to get the relief you need and follow the instructions of the doctor; besides, elderly patients are usually prescribed lower doses of Ativan.
Ativan onset of action also depends on the method of administration:
As for the Ativan duration of action, you can expect Ativan effects to last for about four to six hours. People with higher sensitivity will notice the impact of Ativan on their physical and mental state as well as its sedative effects longer.
Right after a patient takes Ativan, they will feel less anxious, their stress levels and blood pressure will be lower, and they will be able to concentrate on a certain activity or topic, especially if before the pill or injection they were on the verge of an anxiety attack. Many patients reported that prior to using Ativan, drowsiness made it difficult for them to feel more present and alert to their surroundings. One of the key Ativan sensations is increased mental clarity – your mind is not clouded, and you can focus your attention on what is important to you.
![]()
Despite all the positives associated with Ativan, dizziness and lack of coordination are among the main physical sensations of this drug. You may fall asleep very soon after you take this medication since the tension in your body and confusion in your mind no longer prevent you from doing so. Still, muscle relaxation may be dangerous for individuals who plan to stay awake and, for instance, get behind the wheel – you will find it hard to concentrate on a task that requires your undivided attention.
As for the mental health consequences of Ativan, relaxation naturally affects both the body and the mind of the patient for a limited period of time. The more you use this medication, the more likely it is for you to experience diverse feelings caused by Ativan:
Let us take a closer look at the most common Ativan side effects – research has shown that around ten percent of people who took this medication reported various adverse effects:
| Side Effect | Description |
Lower Blood Pressure | Ativan will lower your heart rate and blood pressure for a short period of time – although this is good for anxiety and people who feel like they are about to have a panic attack, it causes fatigue and nausea |
| Loss of Balance Control | You may be unsteady and dizzy, walking close to the wall in order to lean on it if you suddenly faint – it is easy to feel like you are spinning despite not moving at all |
Seizures | If Ativan is misused or abused while the prescription was made for seizures, the seizures may only become more frequent – in this case, the doctor might prescribe a different medication or advise you to receive round-the-clock care to prevent this from happening again |
Depression | Although Ativan is often prescribed for anxiety – specifically, to avoid future mental health issues and depressive episodes – this medication can worsen your depression due to the combination of Ativan effects like fatigue, poor concentration, and permanent sadness |
Overdose | While overdoses are rare, it is still possible to abuse this medication – if a patient exhibits unusual sleepiness, their behavior lacks coordination, and they are excessively sweating, make sure they did not take a larger dose of Ativan against the doctor’s orders |
Unfortunately, patients who use Ativan for a considerable amount of time, as well as individuals who fail to adhere to instructions given to them by their doctors, may become addicted to this medication – they cannot function without a dose of Ativan or they need to increase the dosage to still have the same Ativan experience their bodies have become accustomed to.
Be mindful of the following signs that may indicate Ativan addiction:
The individual uses Ativan without taking into account the advice of the mental health professional who prescribed it in the first place.
It is impossible for a person to stop taking Ativan without outside interference.
The patient no longer cares about their work, studies, or home life and cannot find enjoyment in hobbies and activities they used to love prior to starting their prescription medication.
Ativan is taken even against the advice of the doctor or obtained illegally to allow the person to continue its use.
Ativan is typically prescribed by doctors to patients with anxiety, insomnia, and epileptic seizures – it has a calming effect on a person’s mind and body, making them feel secure and physically relaxed so that their symptoms do not bother them while Ativan is doing its job.
Before you are truly familiar with how Ativan affects your concentration and alertness, it is not recommended to drive and operate heavy machinery while you are under the influence of this medication. As for other types of work, you may find it difficult to stay focused on a particular task or memorize information so try to take Ativan in your free time and on a day off – of course, you should discuss this matter with a doctor.
The majority of doctors recommend taking Ativan for a limited period of time – the symptoms can be dealt with right away, and if additional treatment is required, you can talk to your doctor about it. It may be dangerous to take Ativan for longer than a few weeks since it is highly addictive and many patients develop a tolerance to this medication.
If someone close to you stopped consulting with a doctor about Ativan and related medication, started procuring Ativan behind their physician’s back, or the dose of Ativan they require to feel calm and stable now is much higher than what it was several weeks ago, it is likely they have developed a dependence and you should seriously talk to them about it.
While the withdrawal syndrome is not as severe as alcohol withdrawal, it is still hard to go through several days or weeks of craving Ativan, increased anxiety, headaches, and vomiting. Besides, many patients develop depression after they no longer have access to this medication so make sure a doctor guides you in your recovery.
Ativan (also known as Lorazepam) is a medication whose primary purpose is to treat anxiety – basically, your nervous system slows down, and you worry less about your past, present, and future. Despite all the positive impacts of this drug, there are side effects that do not always depend on the age of the patient, other medications they take for other disorders and conditions, or the dosage of the drug.
In our guide we will learn more about the adverse effects of Ativan, examine how it impacts the body and the mind of the person who takes it, and understand the specifics of addiction to this type of medication. We will also discover how Lorazepam may impact blood pressure, look at its potential effects on cardiovascular health, and key factors to consider when managing hypertension.
Lorazepam side effects – unintended and unwanted consequences of using a drug – may vary from patient to patient. They also depend on the dosage of the medication the person took – the higher the dosage, the more likely it is the individual will cope with various issues. The most common Ativan adverse reactions are as follows:

The positive effects Lorazepam will cause include relaxation of muscles, elimination of muscle pain, and prevention of seizures that may threaten the life of the person – when a doctor prescribes you Ativan, you can trust this drug to be effective in the right dosage.
However, since Ativan may make the person drowsy, clumsy, and disoriented, it increases the chances the individual gets accidentally injured – the physical sensations of the person on Ativan can be compared to the state of drunkenness – in both cases, the individual may have blurry vision and struggle with their coordination.
Patients prescribed to take Ativan must be particularly careful when they operate heavy machinery or engage in other activities that may harm them and people around them – their physical functions may be affected even further if the individual takes other sedatives or drinks alcohol.
Ativan adverse reactions will be evident both for the individual taking the medication and others around them – despite the fact that it helps with anxiety and jitteriness, your emotional state may not be the same one you are used to. Research has shown that many patients feel empty and lack the energy to participate in activities and events they enjoy after taking Lorazepam to be able to sleep at night.
If the dosage is not calculated correctly or this is just the wrong benzodiazepine for this particular individual, they will feel confused and tired. Moreover, sometimes the medication backfires – anxiety returns, sleep patterns are broken once more, and the patient is agitated and worried until the drug is out of their system.
Unfortunately, if you misuse Ativan, an overdose may occur – in case you are not following the specific instructions of the doctor or you have access to this drug and are using it without medical supervision, your body might become overwhelmed by the medication you took.
Remember that you do not have to worry about overdose if you are guided in your recovery by a mental health professional. Make sure you always take the right dosage – a high dose of Lorazepam may be fatal for a patient, in particular when this person decides to combine this medication with other drugs whose side effects can be unpredictable. Research has shown that Lorazepam abuse risks are higher for people who often mix Ativan with alcohol, drugs whose purpose is to relieve pain, antidepressants and similar benzodiazepines meant to treat anxiety, and sleeping pills.
It is vitally important to recognize Lorazepam overdose symptoms to provide urgent medical assistance to a person in need – here is what you should be on the lookout for if you suspect someone in your vicinity is going through an Ativan overdose:

When you take Ativan for a considerable amount of time, your body becomes accustomed to it – physically and mentally you adapt to the presence of this medication in your system, and you may struggle to take care of your regular duties when there is no drug available for you to take. An abrupt dose reduction or full discontinuation of use might cause withdrawal – various mental and physical complications that often require medical intervention. Here is a list of the most common Ativan discontinuation symptoms you may experience:
Lorazepam addiction treatment should be selected based on the symptoms of the patient and their medical history but usually it encompasses the following methods of treatment:
| Approach | Description |
| Medical Supervision | Although the Ativan withdrawal timeline depends on the dosage the person has gotten used to as well as their health in general, within three or four days since the last administration of this drug you may experience the most serious symptoms – seek professional help, and the doctor will ensure the withdrawal symptoms are minimized |
| Residential Treatment | In the most severe cases of addiction, staying at a rehabilitation center where you are monitored round-the-clock and get to attend therapy on a daily basis while your body is going through drug detox and adjusting to your healthy lifestyle can be the best solution for a patient |
| Individual Counseling | Open up to a therapist – they will be able to pinpoint the causes of your addiction and explore coping mechanisms designed for people in your position to prevent relapses and continue with their recovery for years to come |
| Group Therapy | Whether you were struggling with Ativan adverse reactions in the past or you are worried about challenges that may appear in the future now that you are not relying on drugs to cope with anxiety or insomnia, talking to your peers who have gone through the same experience may be very therapeutic |
| Lifestyle Changes | In case one of the consequences of Ativan addiction and its use, in general, was its negative impact on your cardiovascular health, you should keep your hypertension under control – exercise to get rid of extra weight, limit the amount of alcohol you are consuming, sleep eight hours per night, and quit smoking |
The purpose of this medication is to help patients with anxiety – Ativan has a calming influence on the nerves and brain of the patient, they worry less, sleep more, and no longer have panic attacks that bothered them in the past.
It is essential to follow the instructions the doctor provides you with regarding the use of Lorazepam – like many other prescription drugs, it is highly potent and may cause seizures and coma if administered incorrectly.
If you are worried someone else close to you may be addicted to Ativan, pay attention to their behavior – they will keep using Lorazepam in doses higher than prescribed, spend a long time recovering from the drug once it is administered, and put their life on hold as they are focusing on this medication at the expense of their personal and professional aspirations.
Patients with various cardiovascular diseases must warn their physicians about their diagnoses before getting an Ativan prescription – in certain cases, it causes hypertension or hypotension, impacts heart rhythm, and even increases the odds of cardiac arrest.
Although initially you may benefit from Lorazepam and the stress relief it brings you, it is easy to develop an addiction to this medication just like it happens with many antidepressants whose dosage is supposed to be regulated. Luckily, addiction treatment helps people recover from their dependence without major complications in the future – reach out to a mental health professional and free yourself from addiction.
The main use of morphine is to provide considerable relief to patients with chronic illnesses and severe injuries. Even though the pain relief and additional effects of morphine will fade away within four to five hours, the morphine detection time is longer than that – in particular, hair follicle testing will indicate the presence of morphine in the human body for up to three months.
Let us discover how long morphine stays in the system, outline the factors that influence its detection time, and figure out what is important to know about different drug testing methods.
Morphine refers to a prescribed opioid medication – its purpose is to relieve the pain by releasing dopamine. Due to this fact, using morphine without a proper prescription or in high doses can often lead to misuse of this drug and addiction. This is a highly addictive substance a person can develop a tolerance to – they will need to increase the dosage again and again to feel the same euphoria and no longer experience pain. Morphine withdrawal is also dangerous since without medical intervention, it may even lead to the death of the individual.
Morphine clearance time largely depends on two internal organs of a person – kidneys and liver:
It is important to conduct blood tests to check how a patient is responding to morphine as medication as well as figure out if the individual was using morphine for recreational purposes in case it has an influence on their job in the process of pre-employment drug screening. The detection of morphine in blood is possible for twelve hours since it was last used. Recently, more methods of sensitive detection have been utilized – it allowed to raise the detection window to one day. Either way, the half-life of morphine lets the drug metabolize and eliminate itself from the bloodstream within two hours, which makes the testing harder, especially when we consider the higher morphine metabolism rate of some people undergoing tests.
Urine analysis remains the most common way to figure out whether the person used morphine or not. When it comes to the duration of morphine in urine, the detection window may vary from 24 to 72 hours since the last dose. There can be exceptions to the general rule – for example, a person who heavily used morphine will retain it in their system for five or six days, while an individual with an unusually fast metabolism will test negative quicker.
It is also important for medical professionals to remember the state of kidneys and liver, the age of the patient, and their hydration level will impact the results of the urine test – interpret the results of the test accordingly after you talk to a person and discover more about their medical history and health condition.
The detection of morphine in saliva is possible for a short period of time. While it is a non-invasive way to learn whether the person was taking morphine or not, which makes it relatively easy in comparison with other methods, there are only two days since the last use to detect the presence of morphine. Note that this window may be slightly different because of the person’s metabolism, the frequency of morphine administration, and the doses they have been taking.
The accuracy of this method is lower due to certain factors that may influence the results such as the oral health of the individual or the latest meal they had which is why it is recommended to rely on other tests combined with the saliva test to get an accurate result.
If you suspect a person has been using morphine in the last few months, there is only one way to know it for sure – carry out a hair follicle drug test. Testing facilities can identify the use of morphine for up to ninety days – they only need a hair sample no longer than 1.5 inches from the person’s head. This method is considered reliable since the hair follicle will show the use of morphine regardless of how frequent the drug use has been.
Additionally, the detection window varies based on the hair you are testing – for instance, if you are using hair taken from the armpit or another body part where hair usually grows slower, it is possible to know with certainty morphine was used almost a year ago. This is a valuable tool for both legal and clinical professionals even though it is impossible to determine when exactly the drug was administered.
Morphine retention duration is determined by certain factors of a pharmacological and physiological nature – it is necessary to understand them in order to correctly prescribe the dosage to patients, predict how long the effects of morphine will last, and assess the results of morphine screenings. Here are a few factors affecting morphine duration:
| Factor | Description |
Age |
The older a person gets, the more changes in their body composition are – there is less lean body mass and more body fat, which will affect the distribution of morphine. As the person ages, the morphine half-life can be prolonged from its usual two to three and a half hours. Additionally, the side effects can have more of an impact on an elderly person’s health – they may deal with hypoventilation and unusual sleepiness |
Physical Condition |
Various illnesses and the state of health, in general, will also influence the morphine detection time. For instance, the condition of the liver will impact the processing of morphine – the drug can be active for longer and become more toxic for the patient. Doctors should pay attention to the gut microbiome since it can modify the analgesic effects of morphine |
Dosage and Frequency of Use |
Apart from the individual traits of a patient, medical providers are supposed to be careful when administering the initial dose and deciding how often morphine is going to be used. While the higher dose has its benefits – the presence of morphine in the system lasts longer – there are also potential side effects and possible addiction. It is necessary to start with a small dose and increase it slowly based on the patient’s reaction |
While short-term side effects of morphine can be overcome, especially if the person is physically strong and there are no serious illnesses that undermine their health (for example, if the individual was given morphine because of an injury), there are long-term consequences of lasting morphine use you should be warned about:
While other methods of testing can only confirm morphine was administered in the last few hours or days, a hair follicle test will provide information about morphine use over the last three months, making it the preferred method of many screening facilities.
Although a urine test is a popular way to verify someone took morphine, there are certain factors that may undermine its accuracy such as the health of the person’s kidneys and liver and potential dehydration of the tested individual.
The age of the person will influence the results of the morphine screening, just like the general state of health, the dose that was administered, and the frequency of use.
When a patient abruptly stops using morphine, there may be unpleasant symptoms – anxiety, hot flashes, nausea, and diarrhea. In some instances, the withdrawal is so severe there is no other choice but to seek medical help – talk to your healthcare provider before making the decision to no longer take morphine.
If you suspect someone you know well may be addicted to morphine, be on the lookout for any suspicious behavior, check how much morphine they take to cope with their pain, and try to detect if their mental and physical performance has declined. Luckily, there are ways to treat this addiction so advise the individual you care about to seek professional help immediately.
While certain drugs can be used legally and treat the most severe symptoms of physical and mental illnesses, improper use of these drugs and substance abuse will seriously harm the health of the person. By understanding drug classifications, medical professionals are able to prescribe the right dosage and warn their patients about the potential consequences of illicit drug use – this is particularly relevant for stimulant drugs like amphetamines and sedatives like depressants.
In this guide, we will discover the differences between amphetamines and depressants through thorough amphetamines and depressants comparison, explore how they affect the body, and learn why their effects are considered opposites.
Depressants are drugs that inhibit neurotransmitters in the central nervous system. They slow down the activity between brain neurons – after you take an antidepressant, you will experience drowsiness, intense relaxation, and relief from pain.
Since the messages between the brain and the body are no longer transmitted at the same speed, the individual on depressants will struggle with coordination and concentration – in particular, their reaction time will become slower. Make sure you avoid combining depressants a doctor prescribed you for a sleep disorder or anxiety with alcohol, muscle relaxants, antipsychotics, and opioids – sedating effects are much stronger.
Depressant drug examples are as follows:
Prolonged administration of depressants or failure to follow instructions given to you by your medical provider can lead to various adverse effects – here is a short list of issues you may deal with when there is no moderation in depressant use:
| Effect | Description |
Disorientation and Confusion | If you take a large dose of depressants or improperly use them, you may have to deal with low coordination, slowed breathing and heart rate, and confused thoughts. It is not uncommon for an individual who takes depressants to fall asleep suddenly while they are busy with an important task |
Chronic Tiredness | Constant fatigue, insomnia, depressive episodes, and panic attacks are frequent effects of depressant drugs – beware of these symptoms because they indicate the dependency on the depressant as well as a growing craving for it |
| Problems With Vision | Blurred vision is a common side effect depressant users experience. Some people have reported the symptoms of paranoia, which are possible if you were abusing depressants |
Overdoses | When a significant amount of depressants is taken, an overdose can be the worst consequence for an individual in question. Make sure you are familiar with the signs of overdose – excessive vomiting, unresponsive state despite being awake, and slowed down breathing – and contact emergency services right away |
Amphetamines are powerful stimulants which means they will significantly speed up the human body. Here is where the stimulant and depressant differences lie, and this is evident by the names given to these substances – the function of the central nervous system is enhanced when the amphetamines are administered.
Amphetamine drug classification includes drugs like dextroamphetamine, which is legally produced and designed to treat narcolepsy, and methamphetamine, manufactured illegally and used to experience temporary euphoria. The effects of either type can be felt immediately – from a random burst of energy that makes you excited and restless to sweating and dilated pupils. If you administer illegal amphetamines, and especially if you share needles with other drug addicts, the consequences can be more severe – from vein damage to various infections including HIV.
Although in some cases, medical professionals will prescribe amphetamines to manage the symptoms of illnesses such as Attention Deficit Hyperactivity Disorder (ADHD), this drug is often manufactured and distributed illegally. Athletes may use amphetamines to boost their performance, while individuals addicted to drugs take amphetamines for recreation, which further affects their dependence on this stimulant.
Both depressants and amphetamines effects vary based on the overall health of the individual taking these drugs, their age, and other medications this person may take of their own volition or following the advice of the doctor. Here are the most common side effects of amphetamine use you can expect:
| Effect | Description |
Lack of Sleep | Amphetamines and similar drugs will cause insomnia – you will not be able to fall asleep after spending several hours in bed or you will wake up very early feeling fatigued and agitated at the same time. This may be dangerous since there may be an impulsive desire to get access to other medications that will not necessarily make you feel better |
Cognitive Impairment | As a consequence of a previous side effect, a person who does not sleep well will exhibit a lack of concentration, memory issues, and an inability to make decisions when they are forced to do so |
Erratic Speech | It is easy to spot a person using amphetamines by how fast they talk – if their speech has no pauses, it is rapid, and it is impossible to discern what they are talking about, it may be the effect of central nervous system stimulants |
Mood Fluctuations and Disorders | Sudden changes in an individual’s emotional state can threaten their relationships with others. While mood swings can be a bother for someone else, anxiety and constant stress that come as a result of this emotional instability will be a big disadvantage for a person using amphetamines regularly |
Amphetamines will increase your heart rate and accelerate your breathing – you will feel intense joy, energy, alertness, and performance no matter what task is at hand. Depressants, in contrast, will make you feel relaxed and sleepy as well as lower the awareness in your brain which makes them perfect for panic attacks and insomnia.
Remember that despite the disparity between depressants and amphetamines, both categories of drugs have a high potential for abuse and quick addiction. Whether you are not sure about the side effects you may have heard about before, you are planning to drink alcohol or take other medications while you are undergoing treatment based on amphetamines or depressants, or you were ever interested in taking these drugs for recreation, get medical advice first and avoid putting your health and life in danger.
In certain cases, the best treatment of medical conditions requires the prescription of stimulant drugs. As long as the health care provider is sure this is the best course of action, and the doses of a particular drug are meticulously calculated, the use of amphetamines is legal to help with narcolepsy, hyperactivity, and obesity.
While amphetamines can make you feel euphoric, self-confident, sociable, energetic, and clear-minded, the harmful effects of amphetamine use will put your health and life at risk – from visible weight loss, increased heart rate, and memory loss you can easily go to tremors, seizures, tooth decay, and overdose.
Do not experiment with addictive substances on your own – even if it seems like a smart idea, the opposite effects of stimulants and depressants will put your internal organs – kidneys, liver, and heart – in danger. Consult with a doctor if the amphetamines prescribed to you cause irritability, fatigue, or nausea.
It is easy to confuse the withdrawal symptoms you experience after no longer using depressants with typical signs of flu – the withdrawal will begin with body aches, headaches, sleep disturbances, and restlessness. However, soon after a person whose withdrawal is not given medical attention will feel a rapid heartbeat and a high blood pressure which may lead to hallucinations and seizures – this is why make sure you get professional help before coming off depressants.
If you drink while you are in the process of treatment with depressants, you will get drunk much quicker – the intoxication will increase the chances of experiencing nausea, sleeping troubles, and losing consciousness; moreover, it is not safe to drive in this condition as well as risk overdosing. It is essential to discuss with the doctor how frequently you plan to drink alcoholic beverages – it is likely they will advise you to stick to sobriety while you are undergoing treatment in order to avoid any issues arising from the combination of drugs and alcohol in your body.
Understanding dual diagnosis—the simultaneous presence of addiction and a mental health disorder—can be a game changer for those struggling with these challenges.
This blog post will explore what dual diagnosis is, why integrated treatment is essential, the available treatment options, the importance of a strong support system, the challenges faced in treatment, and inspiring success stories that highlight hope and resilience. Let’s dive in!
Dual diagnosis refers to the condition where an individual experiences both a substance use disorder and a mental health disorder at the same time. This combination complicates the recovery process and can lead to a cycle of worsening symptoms, making treatment more challenging.
For instance, someone with depression may turn to alcohol to cope, which, in turn, exacerbates their depression. Recognizing the dual nature of these issues is crucial for effective treatment.
Many mental health disorders are often found alongside substance use disorders. Some of the most common co-occurring disorders include:
| Disorder | Description |
| Depression | Individuals may self-medicate to escape feelings of sadness or hopelessness. |
| Anxiety Disorders | People with anxiety may use substances to manage their symptoms, leading to dependency. |
| Post-Traumatic Stress Disorder (PTSD) | Trauma survivors might turn to drugs or alcohol as a means of coping with their distress. |
Understanding the interplay between these disorders can help individuals and professionals tailor treatment strategies to address each person’s unique needs.
Integrated treatment is the process of addressing both addiction and mental health disorders simultaneously. This approach is crucial because treating one condition without addressing the other can lead to poor outcomes. For instance, if someone receives treatment for substance abuse, but their underlying depression is ignored, they may relapse into substance use as a way to cope with their untreated mental health issues.
Research shows that individuals receiving integrated treatment are more likely to achieve lasting recovery. This comprehensive approach addresses the complexity of dual diagnosis, allowing for more effective care and support.

An effective integrated treatment program typically includes several key components:
| Therapy | Therapeutic approaches like Cognitive-Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT) help manage addiction and mental health issues. |
| Medication Management | Medications, such as antidepressants or those designed for addiction treatment, can help stabilize mood and reduce cravings. |
| Support Groups | Support groups like Alcoholics Anonymous (AA) or Narcotics Anonymous (NA) provide a sense of community and accountability. |
| Holistic Approaches | Holistic therapies, such as mindfulness, yoga, or art therapy, enhance emotional and physical well-being. |
| Family Involvement | Engaging family members in treatment provides additional support and fosters healthier relationships. |
Various therapy options can be beneficial for individuals with dual diagnosis. Here are a few commonly used approaches:
| Cognitive-Behavioral Therapy (CBT) | CBT is one of the most effective therapies for treating both addiction and mental health disorders. This approach focuses on identifying and changing negative thought patterns and behaviors. For example, CBT helps individuals recognize triggers for substance use and develop healthier coping strategies. |
| Dialectical Behavior Therapy (DBT) | Originally developed for borderline personality disorder, DBT has shown effectiveness in treating addiction and co-occurring disorders. It emphasizes emotional regulation, distress tolerance, and interpersonal effectiveness. DBT helps individuals develop skills to manage intense emotions and reduce impulsive behaviors. |
| Motivational Interviewing | Motivational interviewing is a client-centered counseling style that helps individuals find their own motivation for change. This approach is particularly effective in the early stages of treatment, as it fosters self-empowerment and encourages individuals to explore their ambivalence toward recovery. |
Medication-assisted treatment (MAT) is an essential component of treating addiction, particularly for opioid and alcohol use disorders. MAT combines medications with counseling and behavioral therapies to provide a holistic approach to recovery. Some commonly used medications include:
| Methadone and Buprenorphine | These medications help manage withdrawal symptoms and cravings for opioid addiction. |
| Naltrexone | Used for both alcohol and opioid dependence, naltrexone blocks the euphoric effects of these substances, helping to reduce cravings. |
| Disulfiram | This medication is prescribed for alcohol use disorder. It causes unpleasant reactions when alcohol is consumed, discouraging individuals from drinking. |
Integrating MAT into a comprehensive treatment plan can significantly improve recovery outcomes for individuals with dual diagnosis.
A robust support system is vital for successful recovery from dual diagnosis. Family members and friends can provide encouragement, understanding, and motivation. However, family members need to educate themselves about addiction and mental health disorders. This knowledge will enable them to offer empathetic support without enabling harmful behaviors.
Here are a few tips for family members to support their loved ones effectively:
| Educate Yourself | Learn about dual diagnosis to understand what your loved one is going through. |
| Encourage Open Communication | Create a safe space for your loved one to share their feelings and experiences without judgment. |
| Set Boundaries | Establish healthy boundaries to protect your own well-being while supporting your loved one. |
| Attend Family Therapy | Participating in family therapy can help heal relationships and improve communication. |
Support groups play a crucial role in recovery. These groups provide a safe environment for individuals to share their experiences and learn from others facing similar challenges. Popular support groups include:
| Alcoholics Anonymous (AA) | A fellowship of individuals who share their experiences to help others recover from alcoholism. |
| Narcotics Anonymous (NA) | Similar to AA but focused on helping those with drug addiction. |
| SMART Recovery | A science-based approach to addiction recovery that emphasizes self-empowerment and motivation. |
In addition to support groups, numerous community resources are available to individuals facing dual diagnosis. Local mental health organizations, rehabilitation centers, and hotlines can provide valuable assistance and information.
Despite increasing awareness of mental health and addiction, stigma remains a significant barrier to treatment. Many individuals fear judgment or discrimination, preventing them from seeking help. Educating the public about dual diagnosis and promoting empathy can help reduce stigma.
Overcoming stigma involves fostering understanding and compassion. Share stories of recovery and emphasize that addiction is a complex issue that affects many people. Encourage open conversations about mental health and addiction to normalize these discussions.

Individuals seeking treatment for dual diagnosis may face several obstacles, including:
| Access to Care | Limited availability of integrated treatment programs can make it challenging to find appropriate care. |
| Cost of Treatment | Financial constraints can deter individuals from pursuing necessary treatment options. |
| Awareness of Dual Diagnosis | Some individuals may not realize they have both an addiction and a mental health disorder, leading to inadequate care. |
To navigate these challenges, individuals should:
| Research Local Resources | Look for local treatment centers that specialize in dual diagnosis. |
| Seek Financial Assistance | Explore options for financial aid, insurance coverage, or sliding scale fees to make treatment more affordable. |
| Advocate for Yourself | Be proactive in seeking help, and don’t hesitate to ask questions or express concerns during the treatment process. |
Dual diagnosis affects not only you but also your loved ones. If you or anyone you know is afflicted with a dual diagnosis, keep in mind that you are not alone; many face this, and help is always available to whoever may need it. However recovery can get very lengthy and complex, taking much time, effort, and commitment. Success is indeed possible for this kind of recovery when the right help and support come into place.
Its ok to reach out for help, whether it’s talking to a good friend who will listen, reaching out to a support group that understands them, or a mental health professional who truly will be of help. Take the first step toward your recovery today because you deserve a healthier, happier life.
Dual diagnosis refers to the condition where an individual experiences both a substance use disorder and a mental health disorder simultaneously.
Integrated treatment addresses both addiction and mental health issues simultaneously, leading to better recovery outcomes and reducing the risk of relapse.
Effective therapies include cognitive-behavioral therapy (CBT), dialectical behavior therapy (DBT), and motivational interviewing.
Family members can educate themselves, encourage open communication, set healthy boundaries, and participate in family therapy.
Yes, support groups like Alcoholics Anonymous (AA), Narcotics Anonymous (NA), and SMART Recovery provide support for individuals with dual diagnosis.
Anxiety can feel like a constant burden, holding you back from enjoying life and making progress in your personal or professional world. If you’re feeling overwhelmed, it might be time to explore your options for anxiety treatment. Choosing the right approach can make all the difference. Whether you’re seeking help for the first time or exploring new methods, understanding the available treatments is key to moving forward.
Anxiety is more than occasional stress or worry. It’s a persistent feeling of dread or unease that can disrupt your daily activities, relationships, and overall well-being. While many people experience some level of anxiety, anxiety disorders involve a higher level of intensity and duration, interfering with daily functioning.
Recognizing anxiety symptoms is the first step toward seeking treatment. Common signs include:
If any of these sound familiar, you might benefit from exploring anxiety treatment options tailored to your needs. Remember, anxiety can manifest differently in everyone, so it’s important to talk to a healthcare professional to get an accurate diagnosis.
There is no one-size-fits-all solution for treating anxiety. The best approach should be personalized to your specific needs. Below are some of the most effective treatments for managing anxiety.
Cognitive Behavioral Therapy (CBT) is one of the most widely used methods for treating anxiety. It helps individuals change negative thought patterns that fuel anxiety. Through structured sessions, patients learn to identify, challenge, and replace harmful thoughts with healthier, more realistic ones. If you’re looking for a proven way to address anxiety, CBT is a good option to consider.
For many people, therapy alone isn’t enough. Medication can be an effective tool for reducing anxiety symptoms, especially in cases of moderate to severe anxiety disorders. Commonly prescribed medications include Selective Serotonin Reuptake Inhibitors (SSRIs) and Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs), which work by balancing the brain chemicals that affect mood and anxiety.
However, medication isn’t for everyone. Some people respond better to therapy, while others may benefit from a combination of both. It’s important to find what works best for you, under the guidance of a doctor.
Mindfulness-based therapies and relaxation techniques have gained popularity as effective tools for managing anxiety. These strategies focus on staying present and gaining control over your thoughts and emotions. Guided meditation, yoga, and breathing exercises are common mindfulness practices that can be a powerful way to reduce anxiety symptoms.
While these methods can be used independently, many people find combining mindfulness with other treatments provides the best results.
Regular physical activity has been proven to lower anxiety. Exercise reduces stress hormones like cortisol while increasing endorphins, which are natural mood lifters. Engaging in activities like running, swimming, or even walking can significantly improve mental health and reduce anxiety.
Choosing the right anxiety treatment depends on factors such as the severity of your anxiety, your personal preferences, and your lifestyle. Here are a few key considerations:
In some cases, mild anxiety may improve over time with self-care. However, chronic or severe anxiety often requires treatment to manage symptoms effectively. Without intervention, anxiety may persist or worsen.
No, medication isn’t always necessary. Many individuals find relief through therapy, mindfulness, or other non-medication approaches. However, medication can be vital for those with more severe anxiety or those who don’t respond to other treatments.
Therapy duration varies by individual. Some people may experience
improvement after just a few sessions, while others may need several months or more. Cognitive Behavioral Therapy (CBT), for example, is often short-term and goal-oriented but is tailored to the individual’s needs and progress.
Some people may wonder whether professional help is essential. While it can be tempting to manage anxiety on your own, professional guidance can provide you with the tools and strategies to handle anxiety more effectively. Early intervention can prevent anxiety from worsening and ensure you’re receiving the right treatment for your specific needs.
Addiction is a multidimensional process and for many people in this world, it is very personal. It is not just about use or dependence, but very often an addiction comes from the complex interrelation of psychological, traumatic, and genetic factors.
Fully comprehending why a person would get addicted requires an understanding of these causes or reasons. When one looks beyond this simple issue of addiction, there comes an appreciation of the struggle and the use of better approaches to its treatment.
| Interconnected Factors | Addiction is influenced by mental health, trauma, and genetics, requiring a holistic approach. |
| Focus on Root Causes | Addressing underlying causes is vital for sustainable recovery. |
| Comprehensive Treatment | Effective treatment integrates mental health support, trauma healing, and genetic awareness. |
In this post, we’ll dive into the mental health connection to addiction, the role of trauma, and how genetics may influence a person’s susceptibility to addiction. Each of these areas contributes to a clearer picture of how addiction takes hold and how recovery must address these root causes.
Addiction is so importantly linked with mental health. Many individuals who suffer from an addiction have other problems, either simultaneously or shortly arising from mental health issues, each of which exacerbates the others in a no-end cycle. It is crucial to learn how the development of mental health disorders contributes to addiction and what consequences it will have for treatment.
Anxiety, depression, bipolar disorder, and PTSD are just some of the mental health conditions that considerably heighten one’s risk of developing an addiction. Mostly, individuals suffering from a mental health condition that is either left unaddressed or poorly treated resort to using substances for relief as a way of self-medication. Though this might momentarily relieve them from the emotional and psychological distress they are experiencing, their dependence on such substances typically escalates into an addiction over time.
A person afflicted with acute anxiety might turn to alcohol or drugs to “calm their nerves” or ease discomfort in social situations, for example. Remedies like that are temporary and do little if anything to cure the anxiety problem instead they will make them dependent upon such substances to get them through the day and eventually create more serious ones. In fact, it is said that 50% of people with a severe mental disorder develop a substance use disorder at some point in their lifetime. A correlation such as this points to the fact that addiction can start in the field of mental health.
Self-medication is a very serious problem for all people who suffer from any kind of mental health disorder and addiction problems. Most of them use drugs or alcohol to reduce their emotional pain or in order to be distracted from psychological struggles. Unfortunately, it creates a vicious circle.
The vicious cycle tends to follow a common pattern: anxious, depressed, or just very stressed people try to find temporary relief with the use of substances.
The behavior of reaching for a substance when a downturn occurs is reinforced by the fleeting relief they get from the substance itself. The body gradually becomes accustomed to the substance, and more and more is required to produce the effect. It becomes a vicious circle of addiction, while the initial mental health condition goes unaddressed.
This is a dangerous cycle, for substances could further deteriorate a mental health condition, setting a vicious cycle that is ever-hard to reverse.

Trauma is another significant factor in the development of addiction. Most addicts report some sort of traumatic experience sometime in their life, either physical, emotional, or psychological. Traumatic reactions can last for decades, many times presenting themselves as addiction, while the person attempts to deal with the long-lasting effects of his experiences.
Trauma can have a profound effect on mental health. When someone experiences a traumatic event, it can leave deep emotional scars that are difficult to heal. For some, the pain of trauma is so overwhelming that they turn to substances as a way to numb or escape these feelings.
Trauma can take many forms, including:
When trauma is left unaddressed, it can lead to mental health disorders like PTSD, depression, or anxiety. These conditions, in turn, can increase the likelihood of substance abuse as individuals try to manage their emotional pain.
The connection between childhood trauma and addiction in adulthood is well-documented. The experience of abuse by a family member or caregiver drives an individual to a highly probable continuance of their addiction throughout their lifetime. This is the reason trauma has an effect on normal emotional development and the ways of coping. This can cause a hindrance in handling a stressful situation or an emotionally difficult situation as well.
A child who develops under abuse will subsequently always seek survival means from the feelings, for example, through dissociation from emotions or being addicted to some sort of substance later in life. Traumatic events during the growing years form a blueprint for later addiction.
The shock of childhood trauma casts long shadows in the brains of survivors, particularly in systems that govern emotion, memory, and decision-making. Therefore, the capability to regulate their feelings in a healthy way is significantly curtailed in traumatized individuals and often drives them toward seeking refuge in substances.
Along with mental health and trauma, genetics also proves to be one of the important factors that influence the effects of addiction. Though environment and personal experiences matter a lot, it is true that some individuals have a genetic predisposition toward addiction.
Current literature indicates that addiction normally runs in the family. This strong genetic linkage underlying addiction is supported across a wide variety of cases. For instance, if a person has a family that is afflicted with addiction problems, then that person has a much higher predisposition to the having same problems.
Though no single “addiction gene” has been found, studies have identified that a person’s genes may contribute to their risk for addiction. An individual may inherit the tendency toward drug addiction as determined by genetic factors affecting the rewarding feelings they experience when using an addictive substance.
In fact, various studies demonstrate that 40-60% of addiction liability originates from an individual’s genes. This kind of association makes it obvious that a person’s family medical history is a significant prognostic factor in determining the addictive propensity of a patient.

Addictive genes are just one part of the jigsaw of addiction. Epigenetic, a term describing how the ambient environment interacts with the expression of genes, is the sum of all causes of addiction. Even in those people with a genetic component to addiction, life events and the ambient environment can “switch on” or “switch off” whatever predispositions might be hardwired into the person’s brain.
While someone genetically predisposed toward addiction will never experience the torture of addiction if they happened to grow up in an extremely nurturing home where healthy coping mechanisms are modeled, for example, someone without a family history of addiction may become entangled into addiction if they have witnessed great traumas or mental health issues. Epigenetics illustrates, however, that where the body sets the base, it’s truly environmental influences that create all the difference between turning a person into an addict or not.
While mental health, trauma, and genetics are significant factors in addiction, they often do not operate in isolation. In most cases, addiction is the result of multiple overlapping factors. Understanding the interplay between these elements is key to getting a complete picture of why addiction occurs and how to treat it best.
Addiction is rarely caused by just one factor. For example, someone may have a genetic predisposition to addiction, but if they grow up in a stable, supportive environment, they may never develop a substance use disorder. On the other hand, someone with no family history of addiction might become addicted due to untreated mental health issues or unresolved trauma.
It’s important to recognize that addiction is a complex condition with multiple contributing factors. Focusing on just one aspect, such as mental health or genetics, is not enough to fully understand or treat addiction.
When it comes to treating addiction, addressing the root causes is essential for long-term recovery. Simply focusing on the addiction itself without looking at the underlying mental health issues, trauma, or genetic predispositions will not lead to lasting change. A comprehensive approach is necessary to break the cycle of addiction and support meaningful recovery.
Comprehensive addiction treatment takes into account the whole person, not just their substance use. This means addressing mental health issues, past trauma, and any genetic predispositions that may have contributed to the addiction. For example, someone with a dual diagnosis of addiction and mental health issues will need treatment that addresses both conditions simultaneously.
Holistic treatment approaches, which include therapies such as cognitive-behavioral therapy (CBT), trauma-informed care, and family therapy, can be effective in addressing these underlying issues. By focusing on the root causes of addiction, individuals have a better chance of achieving lasting recovery.
Understanding the root causes of addiction, mental health, trauma, and genetics, is crucial for effective treatment and recovery. By recognizing how these factors interplay and contribute to addiction, we can develop more comprehensive treatment approaches that address the whole person.
Ultimately, addressing the underlying causes of addiction not only helps individuals recover but also promotes healthier communities. As we work toward breaking the cycle of addiction, let’s focus on understanding and treating the factors that lead individuals to substances in the first place.
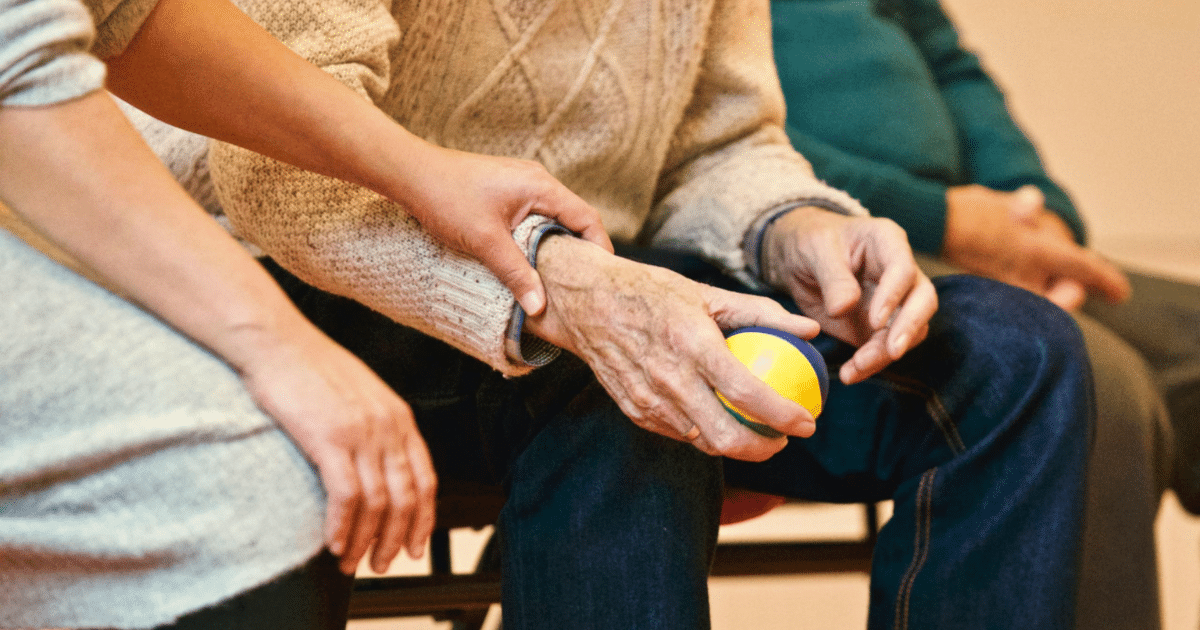
Mental health issues can increase the likelihood of substance use, as individuals often self-medicate to alleviate emotional pain. This can lead to a cycle of addiction.
Experiencing trauma can leave lasting emotional scars, leading individuals to seek relief through substances, which can escalate into addiction if left unaddressed.
Yes, genetics can play a significant role in addiction susceptibility. Individuals with a family history of addiction are at a higher risk.
Self-medication refers to the practice of using substances to cope with mental health issues, which can lead to dependency and addiction.
Effective addiction treatment should include therapy for mental health issues, trauma-informed care, and support for any genetic predispositions to ensure comprehensive recovery.
Understanding the complex relationship between mental illness and drug addiction is crucial for anyone seeking recovery or supporting a loved one through it. These two issues often intertwine, creating a challenging cycle that can be difficult to break.
However, with the right mental health services, it’s possible to address both issues and pave the way toward lasting recovery. In this post, we’ll explore the connection between mental health and drug addiction and the importance of dual diagnosis treatment in effectively managing both conditions.
Mental health challenges and drug addiction are deeply connected. It’s not uncommon for individuals struggling with mental health concerns to turn to drugs or alcohol as a way to cope with their symptoms. This self-medication might provide temporary relief but often leads to a worsening of both the mental health condition and the substance use disorder.
For example, someone dealing with severe anxiety may use alcohol to calm their nerves. Initially, it might seem like a helpful solution, but over time, the person becomes dependent on alcohol, leading to addiction. Misuse of alcohol can worsen their anxiety, creating a vicious cycle where both conditions feed into each other.
Mental health disorders often contribute to the development of substance misuse. Conditions such as generalized anxiety disorder, panic disorder, depression, PTSD, and bipolar disorder can be overwhelming, and individuals may turn to substances in an attempt to manage their symptoms. This section will explore how specific mental health issues can lead to substance abuse and the importance of addressing both simultaneously.
Self-medication is a term used to describe the use of substances like drugs or alcohol to manage mental health symptoms without professional guidance. While it may offer short-term relief, this practice can be incredibly dangerous and often leads to addiction. The substances used for self-medication can alter brain chemistry, worsening mental health concerns over time.
For instance, someone with depression might use prescription drugs or stimulants like cocaine to feel more energetic. However, the effects are temporary, and as the drug wears off, the individual may feel even worse than before, leading to a cycle of increased use and dependency. Over time, this can result in full-blown addiction, compounding the initial mental illness.
Just as mental health disorders can lead to substance abuse, drug addiction can also exacerbate existing mental health conditions or even trigger new ones. This creates a dangerous cycle where both the addiction and the mental health disorder fuel each other, making it difficult for the individual to break free without professional help.
Dual diagnosis treatment is a specialized approach to treating individuals with co-occurring mental health and substance use disorders. It recognizes that these two issues are often interconnected and must be addressed for effective treatment.
The National Institute of Mental Health and Mental Health Services Administration recommend integrated approaches to address both mental health and addiction issues in tandem. This can lead to sustained recovery by tackling both issues simultaneously.
The National Institute on Drug Abuse also supports this dual approach, recognizing the impact of illicit drug use on the brain, which can worsen mental health conditions. Dual diagnosis treatment integrates mental health care and addiction treatment, ensuring both conditions are addressed in a coordinated manner, increasing the likelihood of long-term success.
An effective dual-diagnosis treatment program is comprehensive and personalized, addressing all aspects of the individual’s mental health and addiction. It includes a variety of therapeutic approaches, medication management, and behavioral health services to ensure long-term recovery.
Every individual is unique, and their treatment plan should reflect that. An effective dual diagnosis treatment program tailors the plan to the individual’s specific needs, considering their mental health concerns, substance use history, and personal circumstances.
This personalized approach ensures that all aspects of the individual’s health are addressed, including physical health and behavioral health. The treatment plan may include a combination of therapy, medication, and recovery services tailored to the individual’s needs.
Recovery from dual diagnosis doesn’t end with treatment. Building a strong support system is essential for maintaining long-term sobriety and mental health. Public health organizations like Mental Health America emphasize the importance of community support for people with substance use and mental health issues. An effective dual-diagnosis treatment program includes aftercare planning and support services to help individuals transition from treatment to everyday life.
Key components of support systems and aftercare include:
Seeking help for dual diagnosis is crucial for anyone struggling with both a mental disorder and a substance use disorder. These conditions are often intertwined, and treating one without addressing the other can lead to relapse and ongoing struggles. Health services that offer dual diagnosis treatment provide a comprehensive approach that addresses both conditions simultaneously, increasing the chances of successful recovery.
It’s important to seek help as soon as possible if you or a loved one is struggling with both a mental health disorder and substance use. Common risk factors for substance use include mental health challenges like anxiety, depression, and trauma. Signs that it’s time to seek help include:
The connection between mental health and drug addiction is complex, but understanding this relationship is key to effective treatment and recovery. Dual diagnosis treatment offers a comprehensive approach that addresses both mental health disorders and substance misuse, providing individuals with the tools they need to break free from the cycle of addiction and mental health decline.
With the right treatment and support, including resources from organizations like the National Institute on Drug Abuse, it’s possible to achieve lasting recovery and wellness. Remember, recovery is a journey, and with the right mental health treatment and support, it can lead to a fulfilling and healthy life.
Dual diagnosis refers to the co-occurrence of a mental health disorder and a substance use disorder, a critical area of focus in both mental health services and addiction treatment.
According to the National Survey on Drug Use and Health, dual diagnosis is more common than many realize. About 50% of individuals with a mental health disorder also struggle with substance use issues.
In today’s fast-paced work environment, workplace burnout has become increasingly prevalent. Employees in many fields often feel overwhelmed and stressed, struggling to balance work and personal life. For your well-being and the organization’s success, it’s important to spot signs of burnout and use effective strategies to prevent it.
Before diving into strategies, it’s essential to understand what workplace burnout entails. Burnout isn’t just feeling tired or stressed occasionally; it’s a state of emotional, physical, and mental exhaustion caused by prolonged stress or excessive workload. Symptoms of burnout include feelings of hopelessness, lack of control, and decreased motivation.
Common symptoms include:
Identifying these signs early can help individuals proactively avoid burnout before it escalates.
Setting clear boundaries between work and personal life is crucial for preventing burnout. Here are some actionable steps:
By establishing boundaries and prioritizing self-care, individuals can create a healthier work environment and reduce the risk of burnout.
Organizational culture plays an essential role in employee well-being. Companies that foster a supportive work environment can help prevent burnout. Key strategies include:
Building a supportive work culture enhances employee satisfaction, boosts productivity, and reduces turnover rates.
Continuous learning and skill development are not only beneficial for career growth but also for preventing burnout. Here’s how:
Investing in professional development shows employees that their growth is valued, which can significantly contribute to job satisfaction and reduce burnout.
Prioritize self-care by ensuring adequate sleep, nutrition, and exercise. Set boundaries to manage workload and avoid overcommitment. Practice relaxation techniques like meditation or deep breathing. Seek support from friends, family, or professionals. Take regular breaks and disconnect from work-related activities. Reflect on personal goals and values to realign priorities.
To prevent burnout at work, prioritize self-care by maintaining a healthy work-life balance. Set clear boundaries, take regular breaks, and ensure you get enough rest. Practice stress-reducing activities like exercise or meditation. Communicate openly with your manager about workload and seek support when needed. Regularly assess your goals and adjust them to stay aligned with your personal and professional values.
Strategies for avoiding burnout include setting boundaries to maintain a work-life balance, prioritizing self-care activities such as exercise and adequate sleep, seeking support from friends, family, or professionals, and taking regular breaks to recharge. Additionally, practicing mindfulness or meditation can help manage stress levels and prevent burnout.
To avoid burnout, prioritize self-care by setting boundaries and ensuring regular breaks. Manage your workload by delegating tasks and focusing on what’s essential. Maintain a healthy work-life balance by dedicating time to hobbies and relaxation. Stay connected with supportive colleagues and friends. Regularly assess your goals and adjust them to align with your well-being.
Successful people avoid burnout by setting clear boundaries between work and personal life, prioritizing self-care, and ensuring regular breaks. They focus on time management, delegate tasks, and maintain a supportive network. Regular exercise, mindfulness practices, and hobbies also play a crucial role in maintaining balance and preventing burnout.
Prioritizing self-care is the first strategy for burnout prevention. This involves ensuring adequate rest, maintaining a balanced diet, and engaging in regular physical activity. Setting boundaries to manage workload and taking breaks to recharge are also crucial. By focusing on self-care, individuals can build resilience and reduce the risk of burnout.
In conclusion, preventing workplace burnout requires a proactive approach addressing both individual and organizational factors. Employees can mitigate stress and maintain well-being by establishing clear boundaries, fostering a supportive work culture, and investing in professional development. Employers play a crucial role in creating environments where employees can thrive, ultimately leading to higher productivity and retention rates.
In addiction recovery, social media is increasingly recognized for its potential to support individuals during rehabilitation. As technology continues to intertwine with everyday life, strategically leveraging social media platforms can significantly augment traditional rehab methods. This blog explains how social media can be effectively utilized within rehabilitation programs, drawing insights from leading practices and studies in the field.
Social media platforms like Facebook, Instagram, and Twitter have transformed how individuals communicate, share experiences, and seek support. In the context of rehab, these platforms offer unique opportunities to:
By bridging geographical barriers, social media helps individuals to connect with others who share similar experiences, creating a virtual support network that extends beyond physical boundaries. This is particularly useful in outpatient rehab facilities where patients may feel isolated.
Unlike traditional support groups that meet at scheduled times, online communities and resources are available round-the-clock, providing continuous support whenever needed. This is especially important for those dealing with co-occurring disorders, as they may require support at unpredictable times.
Rehab facilities can tailor content based on individual needs, providing personalized guidance and encouragement through targeted messaging and interactive platforms. A personalized matching process for content delivery can enhance the effectiveness of support.
Ensuring strict privacy settings and guidelines to protect the identities and confidentiality of participants is paramount. This is crucial for maintaining the trust of individuals in recovery.
Sharing evidence-based information on addiction, recovery techniques, and mental health can empower individuals with the knowledge and tools to manage their journey effectively. Educational posts on platforms like social media channels can provide valuable insights into overcoming addiction.
Encouraging active participation through polls, Q&A sessions, and live discussions fosters engagement and community bonding. These interactions can mimic real-life relationships and provide a sense of human interaction that is often missing in digital platforms.
Exposure to particular content or individuals online may trigger cravings or negative emotions, necessitating careful content curation and moderation. Monitoring social media addiction treatment content can help mitigate these risks.
Ensuring platforms comply with HIPAA regulations and implementing strong security measures to protect user data and maintain confidentiality is crucial. Addressing these concerns can prevent potential negative consequences for users.
The integration of artificial intelligence (AI) and machine learning in social media platforms could revolutionize rehab support by analyzing user data to anticipate relapse triggers and provide preemptive support. This could significantly improve the outcomes of addiction treatment programs.
Immersive VR experiences could simulate real-life scenarios for individuals to practice coping mechanisms and resilience skills in a controlled environment. This can be an innovative addition to traditional addiction rehab programs.
Social media can be a double-edged sword in mental health. While it offers support and connectivity, it can also contribute to issues like social media addiction, which requires specialized social media addiction counseling. Balancing these aspects is critical for effective addiction treatment.
Rehab centers must establish guidelines for social media usage to prevent it from becoming a distraction or a source of stress. Setting specific phone times and limiting cell phone usage can help maintain focus on recovery.
Using a well-crafted social media marketing strategy, rehab centers can reach potential clients and share success stories. This not only helps in building a robust online presence but also showcases the positive impact of their programs.
Social media in health care serves as a platform for patient engagement, education, and support. It allows health professionals to share information, promote health awareness, and connect with patients. It also facilitates peer support among patients and can be used for public health campaigns. However, it requires careful management of privacy and accuracy to ensure reliable information dissemination.
Social media can influence drug abuse by normalizing substance use, providing platforms for buying and selling drugs, and exposing users to peer pressure. It can also spread misinformation about drug effects and safety. However, it can be a tool for prevention and recovery support by connecting individuals to resources and communities focused on sobriety and health.
Social networks offer support and connection, reducing feelings of isolation for those in recovery. They provide a platform for sharing experiences and advice, fostering a sense of community. Access to resources and information is enhanced, helping individuals stay informed about treatment options. Encouragement and accountability from peers can motivate continued sobriety and personal growth.
The media plays a crucial role in preventing drug abuse by raising awareness, providing accurate information, and shaping public perceptions. Through campaigns, news reports, and educational programs, media can influence attitudes and behaviors, promote healthy lifestyles, and highlight the consequences of drug use. It serves as a platform for experts to share insights and for communities to engage in dialogue about prevention strategies.
The media can influence drug use and addiction by shaping public perceptions and attitudes. It often glamorizes drug use, downplays risks, and normalizes behavior through movies, music, and social media. This portrayal can lead to increased curiosity and experimentation, especially among impressionable audiences, contributing to the spread of misinformation and potentially encouraging substance use.
Encourage open communication about the risks and consequences of drug use. Support community programs that educate and provide resources for prevention. Foster environments that promote healthy lifestyles and coping mechanisms. Advocate for policies that limit access to drugs and provide support for those at risk. Engage in activities that build self-esteem and resilience among youth.
The use of social media in rehab represents a promising avenue for enhancing support, connectivity, and personalized care in addiction recovery. By leveraging these platforms thoughtfully, rehab facilities can complement traditional methods with modern, accessible resources that empower individuals throughout their recovery journey.
As technology continues to grow, so will the opportunities to innovate and improve addiction treatment strategies, making recovery more attainable and sustainable for those in need.
Incorporating social media into rehab programs isn’t just about embracing technology—it’s about harnessing its power to transform lives positively. Whether through online support groups, educational content dissemination, or personalized coaching, the potential impact of social media on rehab outcomes is undeniable.
By staying current with the latest trends and best practices for integrating social media into rehab programs, facilities can ensure they provide comprehensive, adequate support to individuals seeking recovery from addiction.
Abuse, in its various forms, has profound impacts on mental health, with depression being a common consequence. Whether it’s financial abuse, physical violence, or sexual exploitation, understanding how abuse leads to depression is crucial for both victims and those around them. This blog explores this complex relationship, delving into research and expert insights to provide a deeper understanding.
Abuse encompasses physical abuse, sexual violence, emotional harm, and psychological abuse. It often occurs within relationships of power and control, leaving deep scars on victims’ mental and emotional well-being. Common forms of abuse, such as domestic violence and intimate partner violence, can leave lasting physical symptoms, emotional distress, and psychological maltreatment. Each type of abuse, including technological abuse and digital abuse, contributes to a heightened risk for depression and other mental health concerns.
These experiences often result in traumatic events, bodily injury, and mental distress, which have far-reaching consequences for emotional and physical health.
Victims of abuse often experience intense emotional distress, including feelings of fear, shame, and guilt. These negative emotions can lead to a persistent sense of worthlessness and contribute to major depression. Abusive behavior, such as constant criticism and reproductive coercion, especially during childhood abuse, can exacerbate feelings of sadness and guilt, increasing the prevalence of depression.
Abuse can distort one’s perception of self-worth and safety, leading to negative thought patterns. This cognitive impact includes a heightened risk for depression and the development of adult psychiatric conditions such as bipolar disorder and generalized anxiety disorder. Stressful life events, especially those involving abusive partners or signs of abuse, can lead to a significant difference in mental health outcomes compared to individuals without such histories.
Many abuse survivors develop post-traumatic stress disorder (PTSD), which can manifest in symptoms such as flashbacks, hypervigilance, and avoidance behaviors. Traumatic experiences and chronic pain from past abuse can lead to comorbid anxiety and exacerbate symptoms of depression. Childhood trauma and child sexual abuse are significant factors influencing the development of PTSD.
Abuse is strongly correlated with the onset of depression. Research indicates that individuals who experience abusive situations, particularly during childhood or adolescence, are at a significantly higher elevated risk of developing depressive disorders later in life. The prolonged exposure to trauma, constant monitoring, and emotional distress rewires the brain’s responses, predisposing individuals to mental health challenges.
Abuse experienced in early life stages can have enduring effects on brain development and emotional regulation. Types of child abuse, including physical restraint and non-consensual sexual acts, often lead to a higher prevalence of depression and other mental disorders in adulthood. Adverse childhood experiences significantly impact emotional health and developmental outcomes.
The longer the duration and the more severe the abuse, the higher the likelihood of developing depression. Persistent forms of maltreatment, such as corporal punishment and verbal abuse, contribute to an increased risk for depression. The consequences of childhood maltreatment are well-documented in studies, particularly regarding previous statements made about the enduring emotional harm suffered.
The availability of supportive relationships and access to mental health resources can mitigate the impact of abuse on mental health outcomes. Protective factors, such as parental warmth and supportive environments provided by family, friends, and community organizations, play a crucial role in reducing the negative impact of abuse.
Victims of abuse may internalize a sense of helplessness and hopelessness, contributing to depressive symptoms. This pattern of behaviors used by abusers often leads victims to feel powerless, creating a vulnerability to depression.
Persistent abuse can erode self-esteem, making individuals more susceptible to depressive thoughts and behaviors. Feelings of worthlessness and low self-esteem are common symptoms associated with abusive relationships and depression.
Some survivors may resort to maladaptive coping mechanisms such as substance abuse or excessive texting in attempts to manage their emotional pain. These coping mechanisms, though often detrimental, are commonly used to deal with emotional trauma and further exacerbate depressive symptoms.
Recognizing the signs of abuse and seeking appropriate support are essential steps in breaking free from the cycle of abuse and depression. Social withdrawal and a loss of pleasure in activities are common symptoms among survivors, making it crucial to seek help.
Cognitive-behavioral therapy (CBT), trauma-focused therapy, and support groups can help survivors process trauma and develop healthier coping strategies. These treatment methods are essential for addressing the psychological impact of abuse, including cases of sexual coercion and institutional abuse that may require prescribed medications or follow-up treatments.
Encouraging open communication and offering non-judgmental support can empower survivors to seek help. Non-judgmental family support and legal protection are vital for recovery and resilience.
Non-profit organizations and shelters provide safe havens and comprehensive support services for abuse survivors. These resources can include access to financial control assistance, medical care, and legal protection.
Challenging myths and misconceptions that blame victims for the abuse helps shift societal attitudes toward empathy and understanding.
Recognizing cultural factors influencing perceptions of abuse encourages inclusive support strategies.
Abuse is any action that intentionally harms or injures another person. It can take many forms, including physical, emotional, sexual, and psychological harm. Abuse can occur in various settings, such as homes, workplaces, or institutions, and can affect individuals of any age, gender, or background. Recognizing the signs of abuse is crucial for prevention and intervention.
The 10 types of abuse include physical, emotional, sexual, financial, digital, neglect, psychological, verbal, cultural, and spiritual abuse. Each type involves different harmful behaviors, such as physical harm, manipulation, control, or exploitation, impacting the victim’s well-being and autonomy. Recognizing these forms is crucial for prevention and support.
1. Prioritize your physical health by maintaining a balanced diet, regular exercise, and sufficient sleep.
2. Establish a support network of trusted friends, family, or support groups.
3. Practice mindfulness and relaxation techniques to manage stress and anxiety.
4. Set boundaries to protect your emotional and mental well-being.
5. Engage in activities that bring joy and fulfillment to nurture your spirit.
Stay calm and composed. Responding with anger can escalate the situation. Set clear boundaries by expressing that the behavior is unacceptable. Use assertive communication to convey your feelings without aggression. If necessary, remove yourself from the situation to protect your well-being. Seek support from friends, family, or professionals if the abuse continues.
Set boundaries and communicate clearly. If the behavior continues, consider limiting contact or seeking support from friends, family, or professionals. Prioritize your well-being and safety. If necessary, involve authorities or legal measures to protect yourself. Remember, it’s important to take care of your mental and emotional health in these situations.
Verbal abuse can manifest as name-calling, insults, or derogatory remarks aimed at belittling or demeaning someone. It may involve yelling, screaming, or using a harsh tone to intimidate or control. Verbal abuse can also include gaslighting, where the abuser makes the victim doubt their own perceptions or feelings. It often involves constant criticism, humiliation, or threats, creating a toxic environment.

Life is a journey encompassing a myriad of experiences, both joyous and challenging. While we eagerly embrace the highs, we may often find ourselves feeling overwhelmed or ill-prepared for the lows. Creating a mental health toolbox is an invaluable way to proactively equip ourselves with the necessary tools and techniques to navigate the complexities of life and foster emotional well-being and resilience.
With a proactive approach to mental health, an individual can develop personal coping mechanisms, healthy habits, and a support network, enabling them to weather the storm and emerge stronger. In this article, we will explore the key components of creating a mental health toolbox that will empower you to thrive, irrespective of life’s challenges.
Have you ever found yourself at a loss for how to effectively manage stress, anxiety, or other emotional challenges? By creating a mental health toolbox, you take control of your emotional well-being. Just as one cannot predict every obstacle that life may present, being equipped with an array of coping strategies ensures you are prepared to face any challenges head-on.
Resilience is the ability to bounce back from adversity and navigate through life’s difficulties. A mental health toolbox is a vehicle to cultivate resilience as it helps you discover, develop, and implement strategies that foster emotional strength and adaptability. The more tools at your disposal, the better equipped you are to endure setbacks and emerge stronger.
Self-awareness is the cornerstone of creating a mental health toolbox. This crucial first step involves understanding your emotions, triggers, needs, and strengths. Cultivating self-awareness empowers you to respond to challenging situations rather than react impulsively. Here are techniques to enhance self-awareness:
Every individual is unique, and so are their coping mechanisms. It’s essential to identify strategies that resonate with you and cultivate a diverse range of tools that address various aspects of your emotional well-being. Here are some approaches to consider:
In addition to coping strategies, fostering healthy habits is vital for maintaining emotional well-being. These habits play a significant role in supporting mental health by establishing a strong foundation for resilience. Consider incorporating the following practices into your routine:
Certainly! Here is an FAQ answer for “How to build a mental health toolkit?”:
A mental health toolkit is a set of personalized strategies and resources to help manage stress and emotional challenges. Start by identifying your stressors and the activities that help you relax. Include practices like deep breathing, journaling, or exercise. Consider professional resources such as therapy apps or support groups. Regularly update your toolkit to ensure it meets your evolving needs.
The 5 C’s of mental health are Connection, Compassion, Coping, Contribution, and Confidence. Connection emphasizes the importance of relationships and community. Compassion involves showing kindness to oneself and others. Coping refers to effectively managing stress and emotions. Contribution highlights the value of helping others. Confidence is about building self-esteem and belief in one’s abilities.
A mental health box, also known as a self-care kit, is a personalized collection of items and tools that help you relax, manage stress, and enhance your well-being. Include things that engage your senses, such as soothing teas, calming scents, or fidget toys. It’s important to customize your box with items that resonate with your personal preferences and needs for optimal mental health support.
What items should be included in a mental health kit?
A mental health kit can include items that promote comfort and relaxation such as calming teas, stress balls, journals, or art supplies. Personalize the kit with items that resonate with you like favorite books, soothing music playlists, or reminders of positive affirmations. Consider including a list of contacts for friends, family, or professionals you can reach out to when needed.
A mental health toolbox is a set of strategies, techniques, and resources that individuals can use to support their mental well-being. It includes coping mechanisms, self-care activities, mindfulness practices, and professional resources, all tailored to help manage stress, anxiety, and emotions effectively. This personalized collection empowers individuals to handle mental health challenges proactively.
A wellbeing box can include a variety of items aimed at promoting mental and emotional health. Consider including items such as herbal teas, essential oils, a journal, a cozy blanket, a stress ball, or a mindfulness coloring book. The goal is to fill the box with items that encourage relaxation, mindfulness, and self-care, helping to create a personal sanctuary for moments of stress or anxiety.
Creating a mental health toolbox is a powerful step towards enhancing emotional well-being and building resilience in the face of life’s challenges. By cultivating self-awareness, identifying coping strategies, and embracing healthy habits, you equip yourself to tackle adversity with grace and emerge stronger.
We invite you to embark upon this journey of self-discovery and empowerment, harnessing the infinite potential within you to create a mental health toolbox that is uniquely yours.

Art has long been recognized as a powerful medium for self-expression, but its therapeutic benefits go far beyond aesthetics. Creative expression through artistic mediums like painting, drawing, sculpting, and even writing can unlock emotions, ignite personal growth, and serve as a catalyst for healing. This comprehensive guide delves into the world of healing through art, showcasing how creativity can restore emotional well-being and ignite self-discovery.
Within every brushstroke, every pencil stroke lies the potential to transform pain, grief, and trauma into a tangible form. Art therapy harnesses creativity as a means to navigate deep-seated emotions and experiences that may be difficult to articulate through traditional forms of communication. By tapping into the realms of imagination, individuals can find solace, healing, and empowerment.
Art provides a safe space for individuals to express themselves without judgment or fear. Through the act of creation, emotions can be externalized and released, fostering a sense of catharsis and emotional restoration. Painting, drawing, and sculpting become vehicles for unlocking buried emotions, allowing individuals to visually communicate what words often fail to convey.
a. Painting a New Canvas: Exploring the Emotions Within
Painting offers a vibrant and versatile platform for self-expression. The burst of colors, brushstrokes, and textures can reflect the full spectrum of human emotions. Whether it’s abstract or realistic, art therapy allows individuals to paint their journeys, embracing their pain while simultaneously paving the way for healing and transformation.
b. Sculpting: Shaping our Emotions into Concrete Forms
Sculpting allows the tactile exploration of emotions. It gives individuals the opportunity to mold and shape their feelings in a tangible manner, providing a hands-on approach to healing. Working with clay or other sculpting materials, individuals can create physical representations of their emotions, fostering a deeper understanding of their experiences.
c. Creative Writing: Penning Emotions on Paper
Words have the power to heal, and creative writing allows individuals to narrate their emotions, thoughts, and experiences on paper. Journals, poetry, or even short stories become vessels for releasing emotions, offering a sense of release and clarity. Guided writing exercises can also help navigate complex emotions, leading to profound insights and personal growth.
Healing through art provides individuals with a unique pathway to self-discovery, empowerment, and emotional restoration. It offers an opportunity to delve deep into one’s psyche, addressing buried traumas and fostering resilience. Through the act of creation, individuals often find a renewed sense of purpose, connection, and well-being.
“Silicon valley recovery saved my life!! I was addicted for 20 years and no support! I lost everything and hit my “Rock bottom”. I didn’t know how to stop or where to start. Luckily, I found Silicon Valley Recovery! At first I was hesitant because I was so used to using drugs and alcohol and couldn’t see a life without numbing my pain, my life stressors, or my depression and anxiety. The beautiful facility made it allow myself to open up to treatment and look at my use and disect what needs to change within myself and work from there. Also, the staff showed me the way and taught me the tools to have a regular life. I have seen the light at the end of the tunnel!! Thank you Silicon Valley Recovery for your empathy, knowledge and happiness you’ve given me that I can now carry with me in my healthy future!” – Sammy Garcia
In the realm of healing through art, creativity becomes the catalyst for emotional restoration. Art therapy provides individuals with a safe space to unlock and express their emotions, fostering self-discovery, healing, and personal growth. Through painting, sculpting, and creative writing, individuals can unleash their inner artists, transforming pain into beauty and trauma into resilience. The transformative effects of healing through art are undeniable, offering a pathway to emotional well-being and empowering individuals on their journey of healing.
Silicon Valley Recovery is a safe, relaxing environment where you can comfortably experience authentic healing. Our highly-trained staff for Drug and Alcohol Addiction Treatment is dedicated to helping you find freedom from your addiction and discover a greater sense of self and purpose. We help you do this with personalized care and evidence-based practices. This heart-centered and scientific approach is tailored to meet each person’s needs. Being in treatment doesn’t need to feel like being in treatment.
Mental Health Awareness Month has a rich history, dating back to its first recognition in 1949. Today, its significance is more profound than ever before. Acknowledging and appreciating the crucial role that mental health plays in our overall well-being is of utmost importance. This month-long observance offers a unique opportunity to intensify our efforts in raising awareness about mental health and ensuring that individuals in need receive the treatment and support they deserve.
Over the years, Mental Health Awareness Month has evolved into a powerful platform for education, advocacy, and destigmatization. It serves as a reminder that mental health is not isolated from other concerns but rather an essential component of our overall health and quality of life. Our mental well-being directly impacts our physical health, relationships, work productivity and overall happiness.
In the face of unprecedented challenges brought about by recent global events, the importance of mental health awareness has become even more pronounced. The pandemic has triggered a surge in mental health issues, including anxiety, depression, and loneliness, affecting people from all walks of life. This situation underscores the urgency of addressing mental health needs and ensuring that individuals have access to the resources and support necessary for their well-being.
Mental Health Awareness Month is a vital initiative aimed at spreading awareness about mental health and promoting well-being. At Silicon Valley Recovery, we understand the significance of mental health and are committed to providing support and resources to individuals struggling with mental health issues. In this blog post, we will delve into the significance of Mental Health Awareness Month, discuss the connection between mental health and addiction, and highlight ways to support mental well-being during the recovery journey.
Mental health and addiction are closely intertwined. Many individuals facing addiction also grapple with underlying mental health conditions such as anxiety, depression, or trauma. Conversely, substance abuse can worsen existing mental health issues or even trigger new ones. It is crucial to address both mental health and addiction simultaneously to achieve lasting recovery.
Mental Health Awareness Month plays a crucial role in promoting understanding, empathy, and support for those dealing with mental health challenges, including addiction. This observance encourages open conversations, raises awareness about available resources, and empowers individuals to seek help when needed. By highlighting the importance of mental health in addiction recovery, we can foster a more compassionate and effective approach to treatment.
One of the biggest obstacles individuals face when seeking help for addiction is the persistent stigma associated with substance abuse and mental health conditions. Mental Health Awareness Month aims to break down these barriers by fostering a culture of acceptance and understanding. By educating the public and challenging misconceptions, we can create an environment that encourages individuals to seek help for both their mental health and addiction without fear of judgment or discrimination.
Supporting mental well-being is an integral part of the addiction recovery process. Here are a few tips to enhance mental health during the journey to recovery:
During Mental Health Awareness Month, it is crucial to highlight the resources available to those in need of addiction recovery and mental health support. We offer comprehensive addiction treatment programs that address the unique needs of individuals facing mental health challenges. Our dedicated team of professionals is committed to providing compassionate care and helping individuals on their journey toward mental well-being and lasting recovery.
To support Mental Health Awareness Month and promote well-being, we encourage everyone to take action. Here are a few ways you can get involved:
Mental Health Awareness Month presents a vital opportunity to promote understanding, break the stigma surrounding addiction and mental health, and provide support for those facing these challenges. By raising awareness, offering resources, and supporting mental well-being, we can create a community that prioritizes mental health in addiction recovery. If you or someone you know is struggling with addiction or mental health issues, contact us today. Remember, taking care of your mental health is crucial for leading a fulfilling and healthy life, and we are here to support you every step of the way. Together, let’s embrace the journey of recovery and build a brighter future.
Addiction is a complex disease that can have significant physical, emotional, and psychological effects on individuals. Often, addiction and mental health are intertwined, and individuals struggling with addiction may also be dealing with mental health issues such as anxiety, depression, or trauma. This blog will discuss the connection between addiction and mental health and why understanding this link is critical to effective treatment and long-term recovery.
Many individuals struggling with addiction also have underlying mental health disorders. This co-occurring condition is known as dual diagnosis, which means that an individual is dealing with addiction and mental health disorders. According to the National Institute on Drug Abuse (NIDA), approximately 50% of individuals with substance use disorders also have a co-occurring mental health disorder.
Some common mental health disorders associated with addiction include anxiety disorders, mood disorders such as depression or bipolar disorder, post-traumatic stress disorder (PTSD), and personality disorders. Substance use can exacerbate the symptoms of these disorders, which can also contribute to the development of addiction.
Addiction can significantly impact mental health, exacerbating or contributing to the development of mental health disorders. Substance use can affect the levels of neurotransmitters in the brain, which can contribute to mood disorders such as depression or anxiety. Additionally, addiction can also cause physical changes in the brain, affecting decision-making, impulse control, and other executive functions.
In addition to the physical effects, addiction can also have significant emotional and psychological impacts. Individuals struggling with addiction may experience feelings of shame, guilt, and self-blame. They may also work with low self-esteem, difficulty regulating emotions, and other mental health issues that can contribute to substance use.
Mental health disorders can also play a significant role in the development of addiction. Individuals with mental health disorders may use substances to self-medicate or alleviate the symptoms of their disorder. For example, individuals with anxiety disorders may use drugs or alcohol to alleviate feelings of anxiety, while those with depression may use substances to alleviate feelings of sadness or hopelessness.
Furthermore, some mental health disorders can increase the risk of addiction. For example, individuals with bipolar disorder or borderline personality disorder may be more likely to engage in impulsive behavior, including substance use. Additionally, individuals with a history of trauma or PTSD may turn to substances to cope with the distressing memories and emotions associated with their experiences.
Given the complex connection between addiction and mental health, it is essential to take an integrated treatment approach that simultaneously addresses both issues. Integrated treatment involves addressing both addiction and mental health disorders in a coordinated and comprehensive manner. This approach can improve treatment outcomes and promote long-term recovery.
Integrated treatment may involve a combination of cognitive-behavioral therapy (CBT), medication-assisted treatment (MAT), and other evidence-based practices. Additionally, it may include addressing other underlying issues, such as trauma or relationship problems, that may contribute to addiction or mental health disorders.
One of the biggest challenges in addressing addiction and mental health is the stigma associated with these issues. Society often believes that addiction is a moral failing or a lack of willpower and mental health disorders are a sign of weakness or instability. These beliefs can prevent individuals from seeking treatment and contribute to feelings of shame and isolation.
It is essential to break down the stigma associated with addiction and mental health and promote a more compassionate and understanding approach to these issues. This involves recognizing that addiction and mental health disorders are medical conditions that require treatment and support, rather than judgment and condemnation.
Individuals with dual diagnosis often face unique challenges in their recovery journey. These challenges can include managing addiction and mental health symptoms, addressing the underlying issues contributing to these conditions, and navigating the complex healthcare system. Support groups and peer support programs can be valuable resources for individuals with dual diagnosis, providing a sense of community, accountability, and access to resources and tools.
At Opus Health, we offer support groups and other resources designed to support individuals with dual diagnosis. Our programs are led by experienced professionals who understand the unique challenges of addiction and mental health and can provide guidance and support on the path to recovery.
Addiction and mental health are closely intertwined, and understanding the connection between these issues is critical to effective treatment and long-term recovery. Integrated treatment programs that address both addiction and mental health disorders can improve treatment outcomes and promote lasting recovery. By breaking down the stigma associated with addiction and mental health and providing support and resources for individuals with dual diagnosis, we can help more people achieve and maintain sobriety and mental wellness.
Addiction and mental health are closely intertwined, and effective treatment requires addressing both issues simultaneously. At Silicon Valley Recovery Health, we offer integrated treatment programs designed to meet the unique needs of individuals with dual diagnoses. Our comprehensive approach includes evidence-based therapies, medication-assisted treatment, and other resources to support long-term recovery.
If you or a loved one are struggling with addiction and mental health issues, don’t wait to seek help. Contact us today to learn more about our programs and how we can help guide you on the path to recovery.
Addiction and mental health are closely intertwined, with each potentially influencing the other. Mental health disorders, such as depression and anxiety, can increase vulnerability to substance abuse. Conversely, addiction can exacerbate or trigger mental health symptoms, creating a cycle that complicates treatment.
Dual diagnosis refers to the condition where an individual has both a mental health disorder and a substance use disorder simultaneously. It highlights the interplay between mental health issues and addiction, requiring integrated treatment approaches to address both aspects effectively for better recovery outcomes.
Yes, addiction and depression often co-occur. Both can influence each other; depression might lead some individuals to self-medicate with substances, while addiction can exacerbate or trigger depressive symptoms due to its physical and emotional impacts.
The four C’s of addiction are Compulsion, Craving, Consequences, and Control. Compulsion refers to the overwhelming urge to engage in a behavior. Craving involves the intense desire for the substance or activity. Consequences are the negative outcomes that result from the behavior. Control signifies the inability to regulate or stop the behavior despite these consequences.